Medical expert of the article
New publications
X-rays of a child's and adult's leg
Last reviewed: 04.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
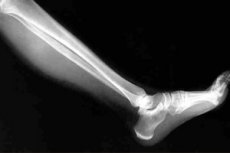
The X-ray method of examining the lower extremities – leg X-ray – is fundamental in traumatology and orthopedics and no less important in rheumatology, since it allows doctors to visualize bones and bone structures, evaluate and differentiate their changes in diseases and pathologies of the musculoskeletal system and make the correct diagnosis.
Indications for the procedure
In traumatology, indications for X-ray examination of leg bones include fractures and cracks, joint injuries (dislocations, damage to the knee meniscus, etc.); bruises, sprains, and ligament ruptures.
X-rays are prescribed to patients with diseases of the bones and joints of the lower extremities (tuberculosis, arthritis, arthrosis, osteoarthrosis, periostitis, etc.), congenital anomalies and acquired deformations of bones and their joints (osteochondrodysplasia, hip dysplasia), contractures or ankylosis of joints, inflammation of their synovial membrane, rheumatic lesions of periarticular tissues, bone cancer (osteosarcoma), etc.
Preparation
No preliminary preparation is required before performing an X-ray examination of the legs. The patient exposes the areas of the limb that need to be examined, removes jewelry and all metal objects.
Parts of the body that are not being examined are protected from radiation by aprons with lead plates.
Technique X-rays of the leg
To obtain a high-quality image – with sufficient contrast and sharpness – the technique for conducting this examination must be followed (taking into account the voltage of the X-ray tube and the radiation field), for which the radiologist or X-ray laboratory technician is responsible.
To obtain adequate X-ray signs of bone and joint diseases on images in standard projections – frontal (anterior or posterior) and lateral – the correct positioning of the limb by the radiologist is especially important. Depending on the localization of the structures being examined and the clinical data, oblique projections are also used, and X-rays of the leg joints can be taken in a bent or straightened position. In most cases, the position of patients on the X-ray table is supine. [ 1 ]
According to the methodological guidelines for positioning the limb being examined, the position of the bone or joint is fixed by placing rollers and sandbags underneath.
Modern clinics use digital X-rays with an analog-to-digital converter, which produces very high-quality images in electronic form - with a shorter exposure time and with minimal radiation exposure to the body. [ 2 ]
In addition, given certain problems with identifying initial pathological disorders in joints with osteoarthritis and other joint diseases on conventional X-rays, more sensitive microfocus X-ray machines are now used.
See more details - Radiography
In complex cases, for example, when there is a suspicion of a hip fracture in elderly people who are difficult to transport to a medical facility, an X-ray of the leg at home is possible, which is carried out by the appropriate specialists using a special mobile X-ray machine.
X-ray of toes
In cases of trauma, in the presence of ankylosing spondylitis, Reiter's disease, psoriatic or gouty arthritis, in cases of osteoarticular panaritium, in cases of defects of the toes (polydactyly or syndactyly), an X-ray of the toes is prescribed - phalanges, metatarsophalangeal and interphalangeal joints.
To obtain a direct projection (dorsoplantar) image, the foot is placed on the sole in a lying position with the knees bent. An image of each toe from the side is taken with the foot placed laterally and each toe fixed in an abducted position.
X-ray of the shin
X-rays of the tubular bones of the leg (fibula and tibia) are taken in direct (posterior) and lateral projections, capturing their ends - with the tibiofibular joint connecting them in the proximal part, and the fibrous ligament (syndesmosis) from the distal end.
Direct projection is achieved by placing patients on their back (with straightened legs), while lateral projection requires placing the corresponding leg on the side, while the healthy limb should be bent.
X-ray of the hip
If it is necessary to perform an X-ray of the hip, the tubular femur is examined in projections similar to those for an X-ray of the shin. For a direct posterior projection, the patient must lie on his back with both legs straight. The lateral projection, accordingly, requires the body to be positioned on its side; in this case, the leg being examined must be bent at the knee and brought forward, and the other is pulled back.
An X-ray of the femoral neck is taken to look for damage (a crack or fracture) to the narrowing area at the top of the thighbone that runs at an angle and connects it to the epiphysis, the top rounded part called the head of the femur.
An X-ray is mandatory for aseptic necrosis of the femoral head – avascular osteolysis of the bone tissue located under the articular cartilage, the so-called epiphyseal subchondral plate, which develops due to insufficient blood supply. In children, aseptic necrosis is called Legg-Calve-Perthes disease.
In this pathology, an increase in the X-ray image in the frontal and lateral projections is practiced.
Since the early stages of osteolysis are not visible on an X-ray, specialists use other instrumental diagnostic methods: magnetic resonance imaging and bone scintigraphy.
X-ray of the joints of the legs
X-rays of the joints of the legs (hip, knee, ankle, foot joints) are performed not only for the purpose of establishing or clarifying a clinical diagnosis, but also before surgical intervention (removal of osteophytes, joint endoprosthetics), as well as to monitor the results of conservative therapy.
Details on how it is carried out:
- X-ray of the ankle joint
- X-ray of the ankle
- X-ray of the knee joint in two projections
- X-ray diagnostics of osteoarthritis of the knee joints (gonarthrosis)
Standard X-rays of the hip joint are taken in two projections: direct (lying on the back with the legs straightened and the feet rotated towards each other, or also on the stomach - with the part of the pelvis raised on the side of the healthy leg) and lateral - lying on the side with the leg bent. If the mobility of the joint is limited, the X-ray is taken in a semi-sitting position (the body is tilted back with support on the arms extended behind the back).
A frontal image of both joints is also taken to compare the anatomical structures of the damaged joint with the healthy one.
In lateral projection images, the patient should be positioned with the limb abducted at the hip joint, and in case of its contracture – without abduction. In addition, the view of the hip joint from behind is provided by irradiating the joint from the back at an angle (from top to bottom), for which the patient should be sitting.
If it is necessary to conduct an X-ray examination of the condition of the periarticular tissues, they resort to X-rays with the introduction of a contrast agent - arthrography of the joints.
Read also – X-ray diagnostics of osteoarthritis of the hip joints (coxarthrosis).
To assess the severity of orthopedic pathology, to determine the nature of the disorders of the hip joint structures, an X-ray is required for hip dislocation (the exit of the femoral head from the acetabulum), as well as an X-ray of congenital hip dislocation - hip dysplasia in children. An X-ray of the joint in the frontal plane allows you to visualize the defect, make all the necessary measurements and, based on these data, choose the most adequate tactics for its correction.
It should be borne in mind that during the first three to four months of life, X-rays of the child's legs are prohibited, and if necessary, an ultrasound of the hip joints of newborns is performed.
More complete information in the material – Diagnosis of congenital hip dislocation.
X-ray of soft tissues of the leg
Targeted X-ray of the soft tissues of the leg, i.e. muscles, is uninformative, since X-rays cannot be reflected by soft tissues, and they are not visible on X-ray images. But in some diseases, for example, ossifying myositis, the presence of ossification areas is determined by the shadows along the fibers of muscle tissue. And in differential diagnostics using X-rays in patients with an autoimmune disease of connective tissue - systemic scleroderma - calcium salt deposits (calcifications) are found in the periarticular soft tissues.
In myopathies affecting the muscle tissue of the lower extremities, the imaging tools are ultrasound and MRI. For more information, see – Muscle examination.
X-ray of leg vessels
X-ray of the blood vessels of the legs with contrast is used in the diagnosis of diabetic or atherosclerotic angiopathy, venous insufficiency or deep vein thrombophlebitis of the lower extremities.
All details in the material – Angiography
Currently, phlebography (X-ray of veins for varicose veins) is being replaced by a more modern, safe and maximally informative duplex scanning or ultrasound of the veins of the lower extremities.
An X-ray of the lymphatic vessels is also done with a contrast agent - lymphography.
Contraindications to the procedure
The list of contraindications to X-rays of the legs is short. These include severe mental illnesses, the presence of metal plates or rods installed in the lower extremities, bleeding, and the patient's unconscious state.
X-rays of the legs are also contraindicated during pregnancy. [ 3 ] For medical reasons, X-rays of the legs are allowed during breastfeeding. [ 4 ]
Complications after the procedure
If X-rays are not taken too often (the standard is once every six months), then there are no negative consequences after the procedure associated with ionizing radiation.
Possible complications after the procedure include exceeding the radiation dose (0.001 mSv per X-ray), as well as unjustifiably frequent use of X-rays, which can slow down bone growth, and damage DNA in children under 12. For this reason, it is better not to perform X-rays until the age of 14 unless absolutely necessary. [ 5 ]
In arthrography of joints, angiography and X-ray of lymphatic vessels, there may be side effects of contrast agents.

