Medical expert of the article
New publications
Preparations
New and best broad-spectrum antibiotics: names of tablets, ointments, drops, suspensions
Last reviewed: 04.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Diseases caused by bacterial infections have existed for as long as humanity itself. But here's the problem: their number is growing every year, and bacteria are evolving, learning to camouflage themselves and survive in adverse conditions. An empirical approach to treating infectious pathologies involves prescribing an antimicrobial agent immediately during the appointment, without waiting for the results of the analysis for the pathogen. In such conditions, it is very difficult to choose an effective drug, because many antibiotics act only on a certain group of bacteria. And here, broad-spectrum antibiotics come to the rescue, effective against a large number of pathogens and used to treat various infectious pathologies of different organs and systems of the human body.
Doctors often have to deal with not one, but several pathogens that have settled in the body of a particular person. Antibacterial agents with a wide spectrum of antimicrobial activity help out in this situation, limiting the number of drugs prescribed to the patient.
Indications broad-spectrum antibiotics
Broad-spectrum antibiotics are rightfully considered universal drugs, since no matter what infection is hidden in the body, they will definitely deal a devastating blow to it. They are used for various pathologies of human organs and systems, the cause of which was a bacterial infection of one or more types.
Broad-spectrum antibiotics for infection may be prescribed in the following cases:
- If it is not possible to quickly determine the pathogen, and treatment is prescribed empirically. That is, based on the patient's complaints, a preliminary diagnosis is established and an antimicrobial drug is prescribed, which should contain the infection until the true pathogen is identified.
By the way, this is a common practice in most medical institutions, especially when it comes to outpatient treatment. Even if they have well-equipped laboratories.
This approach to antibiotic therapy can be justified if we are talking about severe infections characterized by a rapid progression and spread of the process to other organs, and about pathologies that are widespread, the causative agents of which are well known.
- If the bacteria causing the disease are resistant to narrow-spectrum antibiotics.
- In case of detection of a non-standard superinfection, which is characterized by the presence of several types of bacterial pathogens at once.
- To prevent the development of infectious pathologies after surgical operations or cleaning of wound surfaces.
The decision to prescribe a particular drug from a certain group of broad-spectrum antibiotics is made by the doctor independently, based on the situation and the effectiveness of previously prescribed treatment.
Broad-spectrum antibiotics for various diseases
A surprising feature of broad-spectrum antibiotics is that there is no need to invent many such drugs to treat various diseases. The same antibiotic can be used to treat the respiratory system and in the treatment of urogenital infections. Indications for use are noted in the instructions for the drugs, and medical specialists have the opportunity to familiarize themselves with them and use this information in their work.
Let us consider the use of different groups of active antibiotics in the treatment of the most popular pathologies.
Broad-spectrum antibiotics for genitourinary infections. STIs and UTIs are the most common diagnoses in the practice of a urologist. Their treatment cannot be done without the use of effective antibiotics, which ideally should completely destroy the pathogens without causing much harm to the human body.
Medicines for the treatment of the genitourinary system must be excreted by the kidneys and be effective against any bacteria that can cause these pathologies. The use of several medicines is a blow primarily to the gastrointestinal tract (when taken orally), liver and kidneys. Broad-spectrum antibiotics help to avoid this, because with the right selection of medicines, you can get by with just one drug.
Urogenital infections can be caused by various types of bacteria, but the most common are streptococci, staphylococci and E. coli, and in hospital infections - ureaplasma and chlamydia. They should be the target of the prescribed antibiotic.
Several groups of drugs meet this requirement:
- Beta-lactams
- Penicillins (in particular aminopenicillins and combination broad-spectrum antibiotics of the penicillin series, which are protected from the destructive action of beta-lactamases by including inhibitors of this enzyme in the drug).
- Cephalosporins of the 3rd and 4th generations with an extended spectrum of action. The 3rd generation of drugs are effective in pyelonephritis, and the 4th generation are indispensable in complex resistant infections.
- Aminoglycosides. They are also used for urinary tract pathologies, but due to the negative impact on the kidneys, their use is justified only in a hospital setting.
- Macrolides are used only in connection with such a pathology as non-gonococcal urethritis when atypical microflora is detected (for example, chlamydia).
- The same can be said about tetracyclines.
- Carbapenems. They are often the drugs of choice for pyelonephritis (usually imipenem or its analogues are prescribed).
- Fluoroquinolones are indicative of their ability to accumulate in tissues, including the genitourinary organs (bladder, kidneys, prostate gland, etc.). And due to their ability to suppress most strains of bacteria resistant to other antibiotics, they have found quite wide application in urology.
In particular, for cystitis, one of the most common pathologies of the genitourinary system, the following broad-spectrum antibiotics are applicable:
- New generation penicillin drugs, effective against various pathogens (E. coli, anaerobic microbes, Trichomonas, chlamydia, mycoplasma, ureaplasma, etc.), including protected penicillins (Augmentin, Amoxiclav, etc.).
- Cephalosporin antibiotics resistant to resistant strains of bacterial infection (Ceftriaxone, Cefotaxime in the form of injections, Cefuraxime for oral administration, etc.).
- Macrolides (Azithromycin and its analogues for oral administration). The experience of their use in the treatment of urogenital infections in women with penicillin intolerance is indicative, since macrolides have less toxicity.
- Fluoroquinolones (Ciprofloxacin, Nolitsin, etc.). Their advantage is the low frequency of administration and effectiveness against strains that are insensitive to beta-lactams and macrolides. The drugs show a good effect in the treatment of acute cystitis caused by Pseudomonas aeruginosa.
- Additionally, broad-spectrum drugs such as Monural, Levomycetin, Furadonin and other medications may be prescribed at the discretion of the doctor.
When we talk about cystitis, we mean an inflammatory process in the bladder, but inflammation of the kidneys (nephritis) is also considered a pathology no less rarely. Despite the fact that the concept of nephritis is collective and implies several types of kidney pathologies, the most popular of which is pyelonephritis, approaches to the treatment of these diseases in terms of the use of antibiotics have many common points of contact.
Antibiotics for kidney inflammation are used mainly with a broad spectrum of action, since this pathology is known to have a huge number of pathogens that can act both alone (representatives of one group) and collectively (representatives of several groups and strains of bacteria).
When prescribing effective drugs, representatives of the penicillin series (Amoxicillin, Amoxiclav, etc.) come to the forefront, effective in combating enterococci and E. coli. Such drugs can even be prescribed for the treatment of pyelonephritis during pregnancy.
As an option, in the case of uncomplicated nephritis, macrolides (Sumamed, Vilprofen, etc.) can be prescribed, which are effective in the case of both gram-negative and gram-positive pathogens.
Cephalosporins (Ciprolet, Cephalexin, Supraks, etc.) are prescribed when there is a high probability of developing purulent inflammation. In severe cases of the disease and the development of complications, preference is given to aminoglycosides (Gentamicin, Netilmicin, etc.), and in case of severe pain - fluoroquinolones (Levofloxacin, Nolitsin, etc.).
Treatment of inflammatory kidney pathologies is always complex and multicomponent. Antibiotics can be prescribed both orally and by injection, which is often practiced in severe forms of kidney diseases.
Many diseases of the reproductive system have the unpleasant property of being transmitted during sex. Thus, it becomes a problem for both sexes. Such infectious diseases should be treated only with effective antibiotics, and the sooner the better. Therefore, if the pathogen cannot be immediately identified in sexually transmitted diseases (STDs), preference is given to broad-spectrum antibiotics.
Sexually transmitted diseases requiring antibiotics can be different (syphilis, gonorrhea, urogenital chlamydia, Reiter's disease with an unidentified pathogen, venereal lymphogranulomatosis and granuloma), and the approach to their treatment with antibiotics can also differ.
In case of syphilis, preference is given to antibiotics of the penicillin series, which in this case are considered more effective. It is also better to start treatment of gonorrhea with these antibiotics, but in case of intolerance, they can be replaced with other broad-spectrum antibiotics without a doubt.
For urogenital chlamydia and Reiter's disease, mainly tetracycline series AMPs (Tetracycline and Doxycycline), macrolides (Erythromycin, Azithromycin, etc.) and fluoroquinolones (usually Ciprofloxacin) are used.
In case of venereal lymphogranulomatosis, mainly tetracycline drugs (Doxycycline, Metacycline, etc.) are used, and in case of granuloma – penicillin drugs. In the latter case, drugs of other groups are sometimes prescribed (usually in case of penicillin intolerance), for example, Levomycetin, Erythromycin, Tetracycline, etc.
Among sexually transmitted infections, balanoposthitis should be noted. And although this pathology is commonly considered to be purely male, since it consists of inflammation of the head and some part of the male penis, it can be transmitted sexually to women as well.
Broad-spectrum antibiotics for balanoposthitis are prescribed only in the advanced stage of the disease and only when it is not possible to accurately determine the pathogen or there are several of them. In gangrenous, purulent-ulcerative and phlegmonous forms of pathology, antibiotics are used mainly in injection form. In case of a fungal pathogen, AMP are not used.
Another common health pathology that makes itself felt in the autumn-winter period is a cold. Of course, there is no such diagnosis; usually we are talking about respiratory diseases, which are listed in the medical record as ARI or ARVI. In the latter case, the pathogen is a virus that is treated not with AMP, but with antiviral immunomodulatory agents.
Broad-spectrum antibiotics for colds are prescribed only if the weakening of the immune system under the influence of the virus provokes the awakening of bacterial infections in the body 3-5 days after the appearance of the first symptoms of the disease. In this case, it is necessary to treat complications of the cold, such as bronchitis, tracheitis, pneumonia, etc.
ARI, in turn, if treatment is ineffective, can easily develop into tonsillitis, which is also treated with antimicrobial drugs.
In case of bacterial angina, the broad-spectrum antibiotic that the doctor will prescribe first will be from the penicillin series, which is effective against most pathogens of this pathology. The most popular drugs of this type are Amoxil, Flemoxin, Ampicillin, Augmentin, etc.
If the patient is allergic to penicillins, they can be replaced with macrolides (Erythromycin, Clarithromycin, Azithromycin, etc.). In case of complicated pathology, cephalosporin antibiotics (Ceftriaxone, Cephabol, etc.) will be preferable.
Let's briefly consider which antibiotics are appropriate to use for the treatment of bronchitis and pneumonia. For bronchitis with a large number of various pathogens, doctors prefer to prescribe broad-spectrum antibiotics of the following groups:
- Aminopenicillins (Amoxicillin, Augmentin, Amoxiclav, etc.).
- Macrolides (Azithromycin, Sumamed, Macropen, etc.).
- Fluoroquinolones (Ofloxacin, Levofloxacin, etc.) are prescribed in the absence of problems with the gastrointestinal tract.
- Cephalosporins (Ceftriaxone, Cefazolin, etc.) resistant to strains that destroy penicillins.
For pneumonia, doctors prescribe the same groups of broad-spectrum antibiotics, but preference is given to:
- macrolides (“Azithromycin”, “Clarithromycin”, “Spiramycin, etc.)
- fluoroquinolones (“Levofloxacin”, “Ciprofloxacin”, etc.).
The prescription of a broad-spectrum AMP in this case is due to the long wait for the results of tests to determine the pathogen. But pneumonia is accompanied by a strong increase in temperature and other severe symptoms, the rapid relief of which depends only on the effectiveness of the antibiotic.
Another common complication of acute respiratory infections and tonsillitis is otitis (inflammation of the middle ear). The disease is painful and it is not always possible to identify the pathogen, so doctors prefer to use broad-spectrum antibiotics in their prescriptions for otitis. These are usually penicillin (Amoxicillin, Augmentin, etc.) and cephalosporin (Cefroxime, Ceftriaxone, etc.) drugs, which can be prescribed either orally or by injection. In addition, an alcohol solution of Levomycetin is often prescribed, which is used for ear drops.
Broad-spectrum antibiotics are also used to treat some gastrointestinal pathologies. Let's start with the fact that intestinal infections are quite common, occurring both among adult patients and among children. Their pathogens enter the body through unwashed hands, food, and water. Unpleasant symptoms of intestinal infections are the result of poisoning the body with a toxin (enterotoxin) secreted by bacteria.
Dysentery, salmonellosis, cholera, escherichiosis, giardiasis, typhoid fever, food poisoning with staphylococcus - all these infectious pathologies are treated with antibiotics. More than 40 types of pathogenic microorganisms can be the causative agents of these pathologies, the detection of which takes time, during which the toxic infection can spread, causing various complications. This is why the drugs of choice for intestinal infections are antibiotics that are active against many bacteria.
A broad-spectrum intestinal antibiotic is designed to prevent the development of the disease and intoxication of the body, completely destroying any pathogen causing the pathological process in the intestine.
The new generation cephalosporins (Claforan, Cefabol, Rocesim, etc.) and fluoroquinolones (Ciprofloxacin, Normax, Ciprolet, etc.) cope best with this task. Moreover, the drugs are used both in tablet form and as injections.
Aminoglycosides are used for intestinal infections after diagnosis has been clarified. The same can be said about penicillin (Ampicillin) and tetracycline (Doxal, Tetradox, etc.) antibiotics.
Another broad-spectrum drug from the group of antiprotozoal antibiotics, Metronidazole, is used to treat giardiasis.
Everyone knows that such common gastrointestinal pathologies as gastritis and stomach ulcers are very often caused by the bacterium Helicobacter pylori. To treat such pathologies of a bacterial nature, despite the fact that the pathogen is known, the same broad-spectrum antibiotics are used.
Broad-spectrum gastric antibiotics are the same "Amoxicillin", "Clarithromycin", "Metronidazole", "Erythromycin" and others, which are used in various treatment regimens to eradicate bacterial infections. Sometimes 2 antibiotics are used simultaneously, and in other cases, a three-component regimen is preferred.
Prostate diseases are the scourge of the male population of the planet. At the same time, 1/3 of patients have prostatitis of bacterial origin, requiring special antibacterial treatment.
For bacterial prostatitis, doctors can use any broad-spectrum antibiotics that can quickly deal with any infection.
Let's list them in descending order of frequency of use for a given pathology:
- Fluoroquinolones (Ofloxacin, Ciprofloxacin, etc.)
- New generation tetracyclines (Doxycycline, etc.)
- Penicillins, starting from the 3rd generation (Amoxicillin, Amoxiclav, etc.)
- New generation cephalosporins (Ceftriaxone, Cefuroxime, etc.)
- Macrolides (Azithromycin, Vilprafen, Josamycin, etc.).
Broad-spectrum antibiotics are also used in gynecology. They are a universal medicine for any inflammatory process that has arisen in the internal genital organs of a woman. At the same time, they are often prescribed even before receiving the results of smears on the microflora.
The most common drugs prescribed by gynecologists are Ampicillin, Erythromycin, Streptomycin and other drugs from different groups of antibiotics that are active against numerous types of bacterial infections. In severe pathologies, preference is given to Amoxiclav and cephalosporins. Sometimes, combination drugs with a wide spectrum of action are prescribed, such as Ginekit (azithromycin + secnidazole + fluconazole), which are capable of defeating both bacterial and fungal infections.
Broad-spectrum antibiotics have also gained great popularity in the fight against infectious agents in some skin diseases (pemphigus neonatorum, lupus erythematosus, erysipelas, lichen ruber, scleroderma, etc.). In this case, penicillins remain the advantage. The drugs of choice in most cases are: "Oxacillin", "Ampicillin", "Ampiox".
Also, in skin diseases, AMP is widely used in the form of ointments. Antibiotic-containing ointments allow the pathogen to be affected from the outside, which reduces toxic effects for the patient's body (Tetracycline, Erythromycin, syntomycin and many other ointments containing antibiotics).
Broad-spectrum antibiotics are also used for skin pathologies associated with thermal or mechanical damage (wounds and burns). Treatment of small wounds usually does not require the use of serious AMPs, but with the appearance of pus in the wound, the use of antibiotics becomes mandatory.
In the first days of treatment of purulent wounds, broad-spectrum antibiotics (penicillins, cephalosporins and other types of AMP) are mainly prescribed. The drugs are used both in tablets and injections, and in the form of solutions for treating wounds. In the second stage of treatment, the use of antibacterial gels and ointments is also indicated.
In burns, the goal of antibiotic therapy is to prevent and prevent the spread of purulent infection, which is typical for such wounds. The necrotic tissue at the site of a severe burn becomes a breeding ground for various microorganisms. In case of minor burns, antibiotics are usually not used.
To suppress microbial invasion in 3B and 4th degree burns, broad-spectrum antibiotics are used (protected and semi-synthetic penicillins, 3rd generation cephalosporins, aminoglycosides and fluoroquinolones). If the process affects bone structures, Lincomycin is prescribed. Systemic drugs are most often administered intramuscularly or intravenously. Local antibacterial therapy is selected depending on the nature of the wound process.
Surgical intervention also involves violating the integrity of the skin and underlying tissues. Despite the fact that operations are carried out strictly under aseptic conditions, it is not always possible to avoid the risk of developing postoperative purulent complications. Broad-spectrum antibiotics are used to prevent and treat such complications after surgery.
The drugs used in the postoperative period are selected by the doctor individually. In first place are cephalosporins (Ceftriaxone, Cefazolin, etc.) and aminoglycosides (Amikacin, etc.). Then come protected penicillins (for example, Amoxiclav) and carbapenems (Maropenem, etc.).
Broad-spectrum antibiotics have also found their application in dentistry. Bacteria in the oral cavity can penetrate into the tissues of the jaw area through wounds on the mucous membrane and damage to the tooth enamel. Such inflammatory processes (especially acute ones) occurring in the head area are considered very dangerous and require immediate treatment, including antibiotic therapy. In this case, the pathogen is not always detected. This means that broad-spectrum antibiotics remain the drugs of choice: protected penicillins (most often "Augmentin") and fluoroquinolones ("Pefloxacin" and its analogues, "Cifran", etc.). Macrolides (for example, "Summamed") and "Lincomycin" are also used.
Release form
Broad-spectrum antibiotics produced by the pharmaceutical industry may differ not only in their names and scope of application, but also in their release forms. There are drugs that are intended only for oral administration or only for injection administration, while others have several different release forms, which makes it possible to use them in different situations.
Tablets are considered one of the most common forms of drug release. Broad-spectrum antibiotics in tablets are also used much more often than other drug forms. In addition, many of them can be easily purchased at a pharmacy without a prescription.
The most popular penicillin drugs, which are effective in various infectious pathologies of the respiratory, genitourinary and other body systems, are necessarily available in tablet form (as an option, capsules or granules) for oral administration. It is especially convenient if the treatment is carried out on an outpatient basis, since it does not require additional costs and skills of use. This largely determines the wider use of tablets compared to injection solutions.
The most popular penicillins in tablets: Ampicillin, Amoxicillin, Amoxil, Flemoxin, Augmentin, Amoxiclav, Ecobol, Trifamox.
The list of tablet preparations for cephalosporins of the 3rd generation and higher, which are often prescribed instead of penicillins in case of intolerance to the latter, is very small. The active ingredients of these preparations can be cefixime (Cefixime, Suprax, Ceforal Solutab, etc.) or ceftibuten (Cedex, etc.).
Macrolides, which are well tolerated and have the ability to inhibit the proliferation of bacterial infections, have a fairly large list of drugs in tablets: Azithromycin, Summamed, Azitsid, Ecomed, Clarithromycin, Klabax, Erythromycin, Macropen, Rulid, etc.
There are also tablets of the most powerful group of antibacterial drugs - fluoroquinolones, intended for the treatment of severe infectious pathologies of the respiratory, genitourinary, digestive and other systems. The most popular fluoroquinolone is ofloxacin, which in tablet form can be called: "Ofloxacin", "Zanocin", "Oflo", "Tarivid" and others.
No less popular are tablets based on ciprofloxacin (Ciprofloxacin, Ciprolet, Tsifran, etc.).
The most powerful representative of fluoroquinolones is moxifloxacin. It can be found in tablet form under the names "Moxifloxacin", "Avelox", etc.
Despite the fact that many tablets from the AMP series can be purchased at a pharmacy without any restrictions, they can only be used as prescribed by the attending physician and in the dosage prescribed by him.
The number of tablets in a package of AP may vary, as well as the course of treatment with such drugs. Recently, so-called broad-spectrum antibiotics for 3 days have become popular. The package of such AMP usually contains 3 (sometimes 6) tablets or capsules, which are designed for a 3-day course of therapy. The dosage of such drugs is slightly higher than those designed for 5-14 days. And the positive effect is achieved due to the shock dose of the antibiotic.
Oral antibiotics can also be produced in the form of a suspension or granules for its preparation. Broad-spectrum antibiotics in suspension are most often used to treat small children for whom tablet forms are simply not suitable. Suspension is also used if a person has certain difficulties swallowing tablets.
The second popular form of broad-spectrum antibiotics is an injection solution. Some antibiotics can be found on sale in the form of ampoules with a ready-made injection solution, while others are available as a powder for preparing a solution, which is then dissolved in a liquid medium (saline, anesthetics, etc.).
The method of application of such drugs may also differ. Broad-spectrum antibiotics in ampoules are used for parenteral administration of the drug: for intravenous or intramuscular injections, as well as for use in droppers.
Broad-spectrum antibiotics in injections are usually used to treat inpatients with moderate to severe illness. However, in some cases (for example, in gastrointestinal pathologies, when drug irritation causes additional trauma to the gastric mucosa), the ampoule form of the drug can also be prescribed for outpatient treatment. In this case, injections are given by health workers in the physical therapy rooms of medical institutions or by a nurse visiting the home.
If the drug is sold not in liquid form, but in powder or suspension for the preparation of an injection or infusion solution, then in addition to the syringe, you will need to buy a solvent prescribed by the doctor along with the antibiotic. For infusion administration of the drug, you will need a system (dropper).
Antibiotics in injections act faster and are somewhat more effective than oral forms. Their use is indicated for severe pathologies that require urgent measures. Relief occurs already in the first days of taking the drug.
Broad-spectrum antibiotics in ampoules with a ready-made solution or a medicinal substance for its preparation are available for almost all groups of drugs. Among the popular tetracycline drugs, Tetracycline and Doxycycline can be used in the form of injections. Most cephalosporins are available in the form of powder for the preparation of solutions for parenteral administration (Ceftriaxone, Cefazolin, etc.). Carbapenems are available only in the form of injection solutions.
This form of release is available for penicillins (Penicillin, Ampilillin, Trifamox, Ampisid, Timentin, Tizatsin, etc.) and fluoroquinolones (Levofloxacin).
Very often, antibiotic injections are painful, so for intramuscular administration, the powdered drugs are diluted with a lidocaine solution.
Ointments with a broad-spectrum antibiotic are not used as often as the above forms. However, in some cases, their use significantly increases the effectiveness of antibiotic therapy.
Their use is relevant for infectious pathologies of the visual organs, external otitis, infectious skin diseases, healing of wounds and burns, etc. In these cases, the use of systemic drugs does not always allow achieving good results, while the ointment makes it possible to act directly on the bacterial pathogen located on the surface of the body. In addition, in addition to the antibiotic, other components that have a positive effect on the wound can be added to the ointment.
For skin diseases, ointments such as Baneocin, Fastin, Fusiderm, Levosin, Terramycin Ointment, and Sintomycin have become very popular. The ointment with the antibiotic Sanguiritrin is used in both dermatology and dentistry. The ointment Dalacin is used in gynecology for inflammatory diseases caused by some bacterial pathogens.
Tetracycline and erythromycin ointments are effective in treating infectious eye diseases, as well as pustules on the skin and mucous membranes. They are commonly considered to be broad-spectrum eye antibiotics. Although ointments are not the only and preferred form of antibiotics for eye diseases. And doctors often prefer eye drops with a broad-spectrum antibiotic, which are more convenient to use.
Eye drops with antibiotics contain AMP of certain groups. These are aminoglycosides, fluoroquinolones and chloramphenicol (drops "Torbex", "Tsipromed", "Levomycetin", etc.).
Broad-spectrum antibiotics can also be produced in the form of rectal or vaginal suppositories. Most often, such drugs are used in gynecology to treat inflammation immediately after its detection, while a smear analysis for microflora is being carried out. Often, this form of the drug is prescribed in parallel with taking antibacterial tablets. The suppositories dissolve under the influence of body heat and release the active substance, which can act directly at the site of infection.
Pharmacodynamics
Broad-spectrum antibiotics of different groups may have different effects on pathogenic microorganisms. The action of some is aimed at destroying the cellular structure of bacteria (bactericidal), while others are aimed at inhibiting (slowing down) the synthesis of protein and nucleic acids (bacteriostatic).
Bactericidal broad-spectrum antibiotics inhibit the biosynthesis of the cell wall of pathogenic bacteria, thereby destroying them. Bacteria cannot develop further and die. Such action is especially rapid in relation to bacteria capable of active reproduction (and microorganisms reproduce by cell division). The absence of a wall in "newborn" bacteria contributes to the fact that they quickly lose the substances necessary for life, and die from exhaustion. It takes a little more time to destroy adult bacteria in this way. The disadvantage of drugs with bactericidal action is their relatively high toxicity to the body (especially at the time of death of a large number of bacteria) and low selectivity of action (not only pathogenic, but also useful microorganisms die).
Bacteriostatic broad-spectrum antibiotics affect microorganisms differently. By inhibiting the production of protein, which is involved in almost all processes in a living organism, and nucleic acids, which are carriers of important genetic information, they thereby suppress the ability of bacteria to reproduce and preserve species characteristics. In this case, microorganisms do not die, but go into an inactive stage. If the human immune system is functioning well, such bacteria are no longer able to cause the development of the disease, so the symptoms of the disease disappear. Unfortunately, with a weak immune system, the effect of drugs with a bacteriostatic effect will not be enough. But their toxic effect on the human body is less than that of bactericidal drugs.
Penicillin antibiotics of a broad spectrum of action are famous for their noticeable bactericidal action on most gram-positive and gram-negative bacteria (staphylococci, streptococci, diphtheria pathogens, anaerobes, striptochetes, etc.). They have found wide application in the treatment of infectious diseases of the respiratory organs (pneumonia, bronchitis, etc.) and ENT organs (otitis, sinusitis, etc.), infections of the abdominal organs (peritonitis), genitourinary system (pyelonephritis, cystitis, etc.). They are used for purulent surgical infections and to prevent complications after surgical interventions.
The most widely used are semi-synthetic (they are more resistant to the effects of the acidic environment of the stomach and can be used orally) and protected penicillins (combined drugs that are resistant to the effects of beta-lactamase enzymes that destroy them, produced by bacteria for protection).
The disadvantage of penicillin-type AMPs is the high probability of developing allergic reactions of varying severity, including life-threatening ones. However, these drugs are considered the least toxic of all known AMPs.
Broad-spectrum cephalosporin antibiotics also have a strong bactericidal effect. They are characterized by good resistance to beta-lactamases and do not require the inclusion of additional components. The disadvantage of these antibiotics is that most of these effective drugs are not absorbed in the gastrointestinal tract, which means they can only be used parenterally (in the form of injections and droppers). Nevertheless, these AMPs have found wide application in the treatment of infectious pathologies of the respiratory and genitourinary systems. They are used in the treatment of sexually transmitted diseases, ENT infections, to combat pathogens of peritonitis, endocarditis, as well as diseases of the joints and bones.
Broad-spectrum antibiotics from aminoglycosides and fluoroquinolones are also classified as AMPs with bactericidal action, but they are prescribed much less frequently. Aminoglycosides are useful in the fight against anaerobic bacteria and Pseudomonas aeruginosa, but are rarely used due to their high neurotoxicity, and fluoroquinolones with their powerful antibacterial action are preferred mainly for severe purulent infections.
Some drugs from the aminoglycoside group can also have a bacteriostatic effect.
Broad-spectrum antibiotics from the macrolide group, like tetracyclines, are classified as AMPs with bacteriostatic action. They are used to treat infectious diseases of the skin, respiratory organs, and joints. It is indicative to take them in severe diseases (for example, pneumonia) in combination with bactericidal antibiotics. This dual effect of AMPs enhances the therapeutic effect. At the same time, the toxic effect on the body does not increase, since macrolides are considered to be among the least toxic drugs. In addition, they very rarely cause allergic reactions.
When talking about the bactericidal and bacteriostatic action of AMP, it is necessary to understand that the same drug, depending on the pathogen and the dosage used, can have either one or the other effect. Thus, penicillins, at a low dosage or when used to combat enterococci, have a bacteriostatic rather than bactericidal effect.
Dosing and administration
We have figured out what broad-spectrum antibiotics are and how they work in various infectious pathologies. Now it's time to get to know the most prominent representatives of various ASHSD groups.
List of broad spectrum antibiotics
Let's start with the popular broad-spectrum antibiotics of the penicillin series.
 [ 17 ], [ 18 ], [ 19 ], [ 20 ]
[ 17 ], [ 18 ], [ 19 ], [ 20 ]
Amoxicillin
The drug belongs to the class of semi-synthetic antibiotics of the penicillin series of a broad spectrum of action of the 3rd generation. It is used to treat many infectious pathologies of ENT organs, skin, biliary tract, bacterial diseases of the respiratory, genitourinary and musculoskeletal systems. It is used in combination with other AMPs and for the treatment of inflammatory pathologies of the gastrointestinal tract caused by bacterial infection (the infamous Helicobacter pylori).
The active substance is amoxicillin.
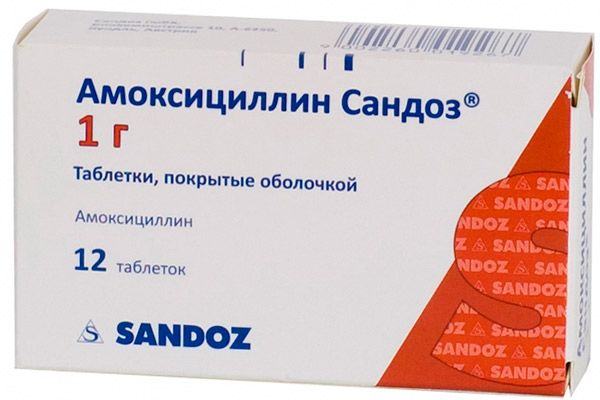
Pharmacodynamics
Like other penicillins, Amoxicillin has a pronounced bactericidal effect, destroying the cell membrane of bacteria. It has such an effect on gram-positive (streptococci, staphylococci, clostridia, most corynebacteria, eubacteria, causative agents of anthrax and erysipelas) and gram-negative aerobic bacteria. However, the drug remains ineffective against strains capable of producing penicillase (also known as beta-lactamase), so in some cases (for example, osteomyelitis) it is used together with clavulanic acid, which protects Amoxicillin from destruction.
Pharmacokinetics
The drug is considered acid-resistant, so it is taken orally. At the same time, it is quickly absorbed in the intestines and distributed throughout the tissues and fluids of the body, including the brain and cerebrospinal fluid. After 1-2 hours, the maximum concentration of AMP can be observed in the blood plasma. With normal kidney function, the half-life of the drug will be from 1 to 1.5 hours, otherwise the process can drag on for up to 7-20 hours.
The drug is excreted from the body mainly through the kidneys (about 60%), some of it is removed in its original form with bile.
Use during pregnancy
Amoxicillin is approved for use during pregnancy, since the toxic effects of penicillins are weak. However, doctors prefer to resort to antibiotics only if the disease threatens the life of the expectant mother.
The ability of the antibiotic to penetrate into fluids, including breast milk, requires that the baby be switched to formula milk for the duration of treatment with the drug.
Contraindications for use
Since penicillins are generally relatively safe, there are very few contraindications to the use of the drug. It is not prescribed for hypersensitivity to the components of the drug, intolerance to penicillins and cephalosporins, as well as for infectious pathologies such as mononucleosis and lymphocytic leukemia.
Side effects
First of all, Amoxicillin is famous for the possibility of developing allergic reactions of varying severity, ranging from rashes and itching on the skin and ending with anaphylactic shock and Quincke's edema.
The drug passes along the gastrointestinal tract, so it can cause unpleasant reactions from the digestive system. Most often, this is nausea and diarrhea. Colitis and thrush can occasionally develop.
The liver may react to the drug by increasing liver enzymes. In rare cases, hepatitis or jaundice may develop.
The drug rarely causes headaches and insomnia, as well as changes in the composition of urine (the appearance of salt crystals) and blood.
Method of administration and dosage
The drug can be found on sale in the form of tablets, capsules and granules for making a suspension. It can be taken regardless of food intake at intervals of 8 hours (in case of kidney pathologies - 12 hours). A single dose, depending on age, ranges from 125 to 500 mg (for children under 2 years old - 20 mg per kg).
Overdose
Overdose may occur when the permissible doses of the drug are exceeded, but it is usually accompanied only by the appearance of more pronounced side effects. Therapy consists of gastric lavage and taking sorbents; in severe cases, hemodialysis is used.
Interactions with other drugs
Amoxicillin has a negative effect on the effectiveness of oral contraceptives.
It is not advisable to take the drug simultaneously with probenecid, allopurinol, anticoagulants, antacids, and antibiotics with bacteriostatic action.
Storage conditions
It is recommended to store the drug at room temperature in a dry and dark place. Keep out of reach of children.
Best before date
The shelf life of the drug in any form is 3 years. The suspension prepared from granules can be stored for no more than 2 weeks.
 [ 21 ], [ 22 ], [ 23 ], [ 24 ], [ 25 ], [ 26 ]
[ 21 ], [ 22 ], [ 23 ], [ 24 ], [ 25 ], [ 26 ]
Amoxiclav
A combined drug of the penicillin series of the new generation. A representative of protected penicillins. Contains 2 active substances: the antibiotic amoxicillin and the penicillase inhibitor clavulanic acid, which has a slight antimicrobial effect.
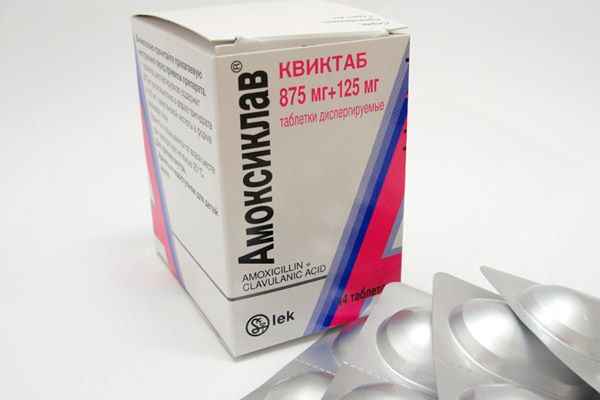
Pharmacodynamics
The drug has a pronounced bactericidal effect. It is effective against most gram-positive and gram-negative bacteria, including strains resistant to unprotected beta-lactams.
Pharmacokinetics
Both active substances are quickly absorbed and penetrate into all body environments. Their maximum concentration is observed an hour after administration. The half-life ranges from 60 to 80 minutes.
Amoxicillin is excreted unchanged, and clavulanic acid is metabolized in the liver. The latter is excreted by the kidneys, like amoxicillin. However, a small portion of its metabolites can be found in feces and exhaled air.
Use during pregnancy
For vital indications, use during pregnancy is permitted. When breastfeeding, it should be taken into account that both components of the drug can penetrate into breast milk.
Contraindications for use
The drug is not used in cases of liver dysfunction, especially associated with the intake of any of the active substances, which is noted in the anamnesis. Amoxiclav is also not prescribed in cases of hypersensitivity to the components of the drug, as well as if reactions of intolerance to beta-lactams have been noted in the past. Infectious mononucleosis and lymphocytic leukemia are also contraindications for this drug.
Side effects
The side effects of the drug are identical to those observed during the intake of Amoxicillin. No more than 5% of patients suffer from them. The most common symptoms are nausea, diarrhea, various allergic reactions, vaginal candidiasis (thrush).
Method of administration and dosage
I take the drug in tablet form regardless of food intake. The tablets are dissolved in water or chewed, washed down with water in the amount of ½ glass.
Usually, a single dose of the drug is 1 tablet. The interval between doses is 8 or 12 hours, depending on the tablet weight (325 or 625 mg) and the severity of the pathology. Children under 12 years of age are given the drug in the form of a suspension (10 mg per kg per dose).
Overdose
In case of drug overdose, there are no life-threatening symptoms. Usually, everything is limited to abdominal pain, diarrhea, vomiting, dizziness, sleep disorders.
Therapy: gastric lavage plus sorbents or hemodialysis (blood purification).
Interactions with other drugs
It is not advisable to take the drug simultaneously with anticoagulants, diuretics, NSAIDs, allopurinol, phenylbutazone, methotrexate, disulfiram, probenecid due to the development of side effects.
Concomitant use with antacids, glucosamine, laxatives, rifampicin, sulfonamides and bacteriostatic antibiotics reduces the effectiveness of the drug. It itself reduces the effectiveness of contraceptives.
Storage conditions
The drug should be stored at room temperature, away from moisture and light. Keep out of reach of children.
Best before date
The shelf life of the drug, subject to the above requirements, will be 2 years.
As for the drug "Augmentin", it is a complete analogue of "Amoxiclav" with the same indications and method of administration.
Now let's move on to an equally popular group of broad-spectrum antibiotics – cephalosporins.
 [ 27 ], [ 28 ], [ 29 ], [ 30 ], [ 31 ], [ 32 ], [ 33 ], [ 34 ]
[ 27 ], [ 28 ], [ 29 ], [ 30 ], [ 31 ], [ 32 ], [ 33 ], [ 34 ]
Ceftriaxone
Among the 3rd generation cephalosporin antibiotics, it is a big favorite among therapists and pulmonologists, especially when it comes to severe pathologies prone to complications. This is a drug with a pronounced bactericidal effect, the active substance of which is sodium ceftriaxone.
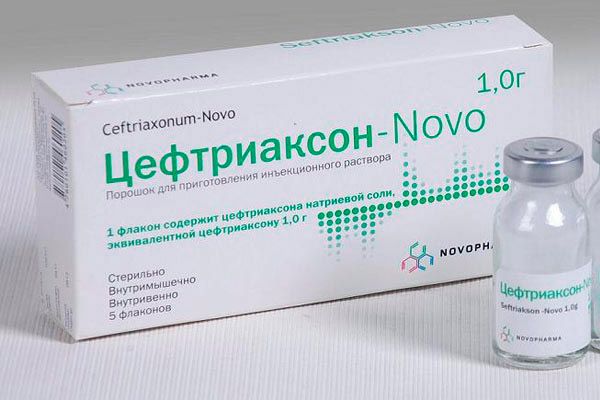
The antibiotic is active against a huge list of pathogenic microorganisms, including many hemolytic streptococci, which are considered the most dangerous pathogens. Most strains that produce enzymes against penicillins and cephalosporins remain sensitive to it.
In this regard, the drug is indicated for many pathologies of the abdominal organs, infections affecting the musculoskeletal, genitourinary and respiratory systems. It is used to treat sepsis and meningitis, infectious pathologies in weakened patients, and to prevent infections before and after operations.
Pharmacokinetics
The pharmacokinetic properties of the drug are highly dependent on the administered dose. Only the half-life period remains constant (8 hours). The maximum concentration of the drug in the blood after intramuscular administration is observed after 2-3 hours.
Ceftriaxone penetrates well into various environments of the body and maintains a concentration sufficient to destroy most bacteria for 24 hours. It is metabolized in the intestines to form inactive substances and is excreted in equal quantities with urine and bile.
Use during pregnancy
The drug is used in cases where there is a real threat to the life of the expectant mother. Breastfeeding should be stopped during treatment with the drug. Such restrictions are due to the fact that ceftriaxone can pass through the placental barrier and penetrate into breast milk.
Contraindications for use
The drug is not prescribed for severe liver and kidney pathologies with dysfunctions, gastrointestinal pathologies affecting the intestines, especially if they are associated with taking AMP, in case of hypersensitivity to cephalosporins. In pediatrics, it is not used to treat newborns diagnosed with hyperbilirubinemia, in gynecology - in the first trimester of pregnancy.
Side effects
The incidence of adverse effects during drug administration does not exceed 2%. The most common are nausea, vomiting, diarrhea, stomatitis, reversible changes in blood composition, and skin allergic reactions.
Less common: headache, fainting, fever, severe allergic reactions, candidiasis. Inflammation at the injection site may occasionally occur; pain during intramuscular administration is relieved with lidocaine administered in the same syringe with ceftriaxone.
Method of administration and dosage
It is considered mandatory to conduct a test for tolerance to ceftriaxone and lidocaine.
The drug can be administered intramuscularly and intravenously (injections and infusions). For intramuscular administration, the drug is diluted in a 1% solution of lidocaine, for intravenous administration: in the case of injections, water for injections is used, for droppers - one of the solutions (saline, glucose solutions, levulose, dextran in glucose, water for injections).
The usual dosage for patients over 12 years of age is 1 or 2 g of ceftriaxone powder (1 or 2 vials). For children, the drug is administered at a rate of 20-80 mg per kg of weight, taking into account the patient's age.
Overdose
In case of drug overdose, neurotoxic effects and increased side effects, including seizures and confusion, are observed. Treatment is carried out in a hospital setting.
Interactions with other drugs
Antagonism between ceftriaxone and chloramphenicol has been experimentally noted. Physical incompatibility is also observed with aminoglycosides, so in combination therapy the drugs are administered separately.
The drug is not mixed with solutions containing calcium (Hartmann's, Ringer's, etc.). Simultaneous administration of ceftriaxone with vancomycin, fluconazole or amsacrine is not recommended.
Storage conditions
The vials with the preparation should be stored at room temperature, protected from light and moisture. The prepared solution can be stored for 6 hours, and at a temperature of about 5 o C it retains its properties for 24 hours. Keep away from children.
Best before date
The shelf life of the antibiotic powder is 2 years.
 [ 35 ], [ 36 ], [ 37 ], [ 38 ], [ 39 ], [ 40 ]
[ 35 ], [ 36 ], [ 37 ], [ 38 ], [ 39 ], [ 40 ]
Cefotaxime
One of the 3rd generation cephalosporins, showing, like others, a good bactericidal effect. The active substance is cefotaxime.
It is used for the same pathologies as the previous drug, has found wide application in the therapy of infectious diseases of the nervous system, in case of blood poisoning (septicemia) by bacterial elements. It is intended only for parenteral administration.
Active against many, but not all, bacterial pathogens.
Pharmacokinetics
The maximum concentration of cefutaxime in the blood is observed after half an hour, and the bactericidal effect lasts 12 hours. The half-life varies from 1 to 1.5 hours.
It has good penetrating ability. During the process of metabolization it forms an active metabolite, which is excreted with bile. The main part of the drug in its original form is excreted with urine.
Use during pregnancy
The drug is prohibited for use during pregnancy (at any stage) and breastfeeding.
Contraindications for use
Do not prescribe in case of hypersensitivity to cephalosporins and during pregnancy. In case of intolerance to lidocaine, the drug should not be administered intramuscularly. Do not give intramuscular injections to children under 2 and a half years old.
Side effects
The drug can cause both mild skin reactions (redness and itching) and severe allergic reactions (Quincke's edema, bronchospasm, and in some cases, anaphylactic shock).
Some patients report pain in the epigastrium, stool disorders, and dyspeptic symptoms. Minor changes in liver and kidney function, as well as in blood laboratory parameters, are noted. Sometimes patients complain of fever, inflammation at the injection site (phlebitis), and deterioration of the condition due to the development of superinfection (repeated infection with a modified bacterial infection).
Method of administration and dosage
After testing for sensitivity to cefotaxime and lidocaine, the drug is prescribed at a dosage of 1 g (1 vial of powder) every 12 hours. In severe infectious lesions, the drug is administered at 2 g every 6-8 hours. The dosage for newborns and premature babies is 50-100 mg per kg of weight. The dosage is also calculated for children over 1 month old. Babies under 1 month are prescribed 75-150 mg/kg per day.
For intravenous injections, the drug is diluted in water for injection; for drip administration (within an hour) – in saline solution.
Overdose
Overdose of the drug may cause damage to brain structures (encephalopathy), which is considered reversible with appropriate professional treatment.
Interactions with other drugs
It is not advisable to use the drug simultaneously with other types of antibiotics (in the same syringe). Aminoglycosides and diuretics can increase the toxic effect of the antibiotic on the kidneys, so combination therapy should be carried out with monitoring of the organ's condition.
Storage conditions
Store at a temperature not exceeding 25 ° C in a dry, darkened room. The prepared solution can be stored at room temperature for up to 6 hours, at a temperature from 2 to 8 ° C – no more than 12 hours.
Best before date
The drug can be stored in its original packaging for up to 2 years.
 [ 41 ], [ 42 ], [ 43 ], [ 44 ], [ 45 ], [ 46 ], [ 47 ]
[ 41 ], [ 42 ], [ 43 ], [ 44 ], [ 45 ], [ 46 ], [ 47 ]
Hepacef
This drug also belongs to the 3rd generation cephalosporin antibiotics. It is intended for parenteral administration for the same indications as the 2 above-described drugs from the same group. The active substance is cefoperazone, which has a noticeable bactericidal effect.
Despite its high effectiveness against many significant pathogenic microorganisms, many bacteria producing beta-lactamase retain antibiotic resistance to it, i.e. they remain insensitive.
Pharmacokinetics
With a single administration of the drug, a high content of the active substance is already noted in the body's liquid media, such as blood, urine and bile. The half-life of the drug does not depend on the route of administration and is 2 hours. It is excreted with urine and bile, and its concentration remains higher in bile. It does not accumulate in the body. Repeated administration of cefoperazone is also allowed.
Use during pregnancy
The drug can be used during pregnancy, but it should not be used without special need. A small amount of cefoperazone gets into breast milk, and yet breastfeeding should be limited during treatment with Hepacef.
Contraindications for use
Other than intolerance to cephalosporin antibiotics, the drug has no other contraindications for use.
Side effects
Skin and allergic reactions to the drug are rare and are mainly associated with hypersensitivity to cephalosporins and penicillins.
Symptoms such as nausea, vomiting, decreased stool frequency, jaundice, arrhythmia, increased blood pressure (in rare cases, cardiogenic shock and cardiac arrest), increased sensitivity of teeth and gums, anxiety, etc. may also be observed. Superinfection may develop.
Method of administration and dosage
After performing a skin test for cefoperazone and lidocaine, the drug can be administered either intravenously or intramuscularly.
The usual adult daily dosage ranges from 2 to 4, which corresponds to 2-4 vials of the drug. The maximum dose is 8 g. The drug should be administered every 12 hours, evenly distributing the daily dose.
In some cases, the drug was administered in large doses (up to 16 g per day) at intervals of 8 hours, which did not have a negative effect on the patient's body.
The daily dose for a child, starting from the neonatal period, is 50-200 mg per kg of weight. Maximum 12 g per day.
When administered intramuscularly, the drug is diluted with lidocaine; when administered intravenously, it is diluted with water for injection, saline solution, glucose solution, Ringer's solution, and other solutions containing the above-mentioned liquids.
Overdose
The drug does not have acute toxic effects. It is possible that side effects may increase, seizures and other neurological reactions may occur due to the drug entering the cerebrospinal fluid. In severe cases (for example, renal failure), treatment may be carried out by hemodialysis.
Interactions with other drugs
The drug should not be administered simultaneously with aminoglycosides.
During treatment with the drug, you should limit the consumption of alcoholic beverages and solutions.
Storage conditions
It is recommended to store the drug in its original packaging at low positive temperatures (up to 8 o C) in a dark, dry place.
Best before date
The drug retains its properties for 2 years from the date of manufacture.
Antibiotics from the fluoroquinolone group help doctors with severe infectious pathologies.
 [ 48 ], [ 49 ], [ 50 ], [ 51 ], [ 52 ], [ 53 ]
[ 48 ], [ 49 ], [ 50 ], [ 51 ], [ 52 ], [ 53 ]
Ciprofloxacin
A popular budget antibiotic from the fluoroquinolone group, which is available in the form of tablets, solutions and ointments. It has a bactericidal effect on many anaerobes, chlamydia, and mycoplasma.
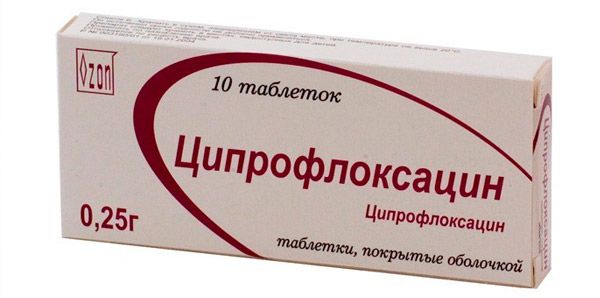
It has a wide range of indications for use: infections of the respiratory system, middle ear, eyes, urinary and reproductive systems, abdominal organs. It is also used in the treatment of infectious pathologies of the skin and musculoskeletal system, as well as for prophylactic purposes in patients with weakened immunity.
In pediatrics, it is used to treat complicated diseases if there is a real risk to the patient’s life that exceeds the risk of developing joint pathologies during treatment with the drug.
Pharmacokinetics
When taken orally, the drug is quickly absorbed into the blood in the initial section of the intestine and penetrates into various tissues, fluids and cells of the body. The maximum concentration of the drug in the blood plasma is observed after 1-2 hours.
Partially metabolized with the release of low-activity metabolites with antimicrobial action. The drug is excreted mainly by the kidneys and intestines.
Use during pregnancy
The drug is not used at any stage of pregnancy due to the risk of damage to cartilage tissue in newborns. For the same reason, breastfeeding should be avoided during the period of therapy with the drug, since ciprofloxacin freely penetrates into breast milk.
Contraindications for use
The drug is not used to treat pregnant and lactating women. Oral forms of the drug are not used in people with glucose-6-phosphate dehydrogenase deficiency and in patients under 18 years of age.
Therapy with the drug is prohibited for patients with hypersensitivity to ciprofloxacin and other fluoroquinolones.
Side effects
Usually the drug is well tolerated by patients. Only in isolated cases can various gastrointestinal disorders be observed, including bleeding in the stomach and intestines, headaches, sleep disorders, tinnitus and other unpleasant symptoms. Rare cases of arrhythmia and hypertension are noted. Allergic reactions also occur very rarely.
May provoke the development of candidiasis and dysbacteriosis.
Method of administration and dosage
Orally and intravenously (jet or drip) the drug is used 2 times a day. In the first case, a single dose is from 250 to 750 mg, in the second - from 200 to 400 mg. The course of treatment is from 7 to 28 days.
Local treatment of the eye with drops: drip 1-2 drops into each eye every 1-4 hours. Suitable for adults and children from 1 year old.
Overdose
Symptoms of drug overdose when taken orally indicate an increase in its toxic effect: headache and dizziness, tremors in the limbs, weakness, convulsions, hallucinations, etc. In large doses, it leads to kidney dysfunction.
Treatment: gastric lavage, taking antacids and emetics, drinking plenty of fluids (acidified liquid).
Interactions with other drugs
Beta-lactam antibiotics, aminoglycosides, vancomycin, clindomycin and metronidazole enhance the effect of the drug.
It is not recommended to take ciprofloxacin simultaneously with sucralfate, bismuth preparations, antacids, vitamin-mineral supplements, caffeine, cyclosporine, oral anticoagulants, tizanidine, aminophylline and theophylline.
Storage conditions
It is recommended to store the drug at room temperature (up to 25 o C). Keep out of reach of children.
Best before date
The shelf life of the drug should not exceed 3 years.
Ciprolet is another popular drug from the fluoroquinolone group, which belongs to the category of broad-spectrum antibiotics. This drug is an inexpensive analogue of the drug Ciprofloxacin with the same active ingredient. It has similar indications for use and release forms to the above-mentioned drug.
The popularity of the next group of antibiotics – macrolides – is due to the low toxicity of these drugs and their relative hypoallergenicity. Unlike the above groups of AMP, they have the property of inhibiting the reproduction of bacterial infection, but do not destroy bacteria completely.
 [ 54 ], [ 55 ], [ 56 ], [ 57 ]
[ 54 ], [ 55 ], [ 56 ], [ 57 ]
Sumamed
A broad-spectrum antibiotic that is a favorite among doctors and belongs to the macrolide group. It can be found on sale in tablets and capsules. But there are also forms of the drug in the form of powder for the preparation of oral suspension and lyophilisate for the preparation of injection solutions. The active substance is azithromycin. It has a bacteriostatic effect.
The drug is active against most anaerobic bacteria, chlamydia, mycoplasma, etc. It is used primarily to treat respiratory and ENT infections, as well as infectious pathologies of the skin and muscle tissue, STIs, and gastrointestinal diseases caused by Helicobacter pylori.
Pharmacokinetics
The maximum concentration of the active substance in the blood is observed 2-3 hours after its administration. In tissues, the drug content is tens of times higher than in liquids. It is excreted from the body over a long period of time. The half-life can be from 2 to 4 days.
It is excreted mainly in bile and a little in urine.
Use during pregnancy
According to animal studies, azithromycin does not have a negative effect on the fetus. However, when treating people, the drug should be used only in extreme cases due to the lack of information regarding the human body.
The concentration of azithromycin in breast milk is not clinically significant. However, the decision to breastfeed during therapy with the drug should be carefully considered.
Contraindications for use
The drug is not prescribed in case of hypersensitivity to azithromycin and other macrolides, including ketolides, as well as in case of renal or hepatic insufficiency.
Side effects
Adverse reactions during drug intake are observed in only 1% of patients. These may include dyspeptic phenomena, bowel disorders, loss of appetite, development of gastritis. Sometimes allergic reactions are observed, including angioedema. It may cause kidney inflammation or thrush. Sometimes taking the drug is accompanied by heart pain, headaches, drowsiness, sleep disorders.
Method of administration and dosage
Tablets, capsules and suspension should be taken once every 24 hours. The last two forms are taken either an hour before meals or 2 hours after meals. There is no need to chew the tablets.
A single adult dose of the drug is 500 mg or 1 g, depending on the pathology. The therapeutic course is 3-5 days. The dosage for a child is calculated based on the age and weight of the small patient. Children under 3 years of age are given the drug in the form of a suspension.
The use of lyofisilate involves a 2-stage process of preparing a medicinal solution. First, the drug is diluted with water for injection and shaken, then saline, dextrose solution or Ringer's solution is added. The drug is administered only intravenously as a slow infusion (3 hours). The daily dose is usually 500 mg.
Overdose
Overdose of the drug manifests itself in the form of side effects of the drug. Treatment is symptomatic.
Interactions with other drugs
Should not be used simultaneously with ergot preparations due to the development of strong toxic effects.
Lincosamines and antacids can weaken the effect of the drug, while tetracyclines and chloramphenicol can enhance it.
It is undesirable to take the drug simultaneously with such drugs as heparin, warfarin, ergotamine and its derivatives, cycloseryl, methylprednisolone, felodipine. Indirect anticoagulants and agents undergoing microsomal oxidation increase the toxicity of azithromycin.
Storage conditions
The drug should be stored in a dry room with a temperature of 15-25 degrees. Keep out of reach of children.
Best before date
The shelf life of capsules and tablets is 3 years, powder for oral administration and lyophilisate – 2 years. The suspension prepared from the powder is stored for no more than 5 days.
Broad-spectrum antibiotics for children
Studying the description of various broad-spectrum antibiotics, it is easy to notice that not all of them are used to treat children. The danger of developing toxic effects and allergic reactions makes doctors and parents of the baby think a thousand times before offering the child this or that antibiotic.
It is clear that if possible, it would be better to refuse taking such strong drugs. However, this is not always possible. And then you have to choose from the whole variety of AMP those that will help the baby cope with the disease without causing much harm to his body.
Such relatively safe drugs can be found in almost any group of antibiotics. For small children, there are suspension forms of drugs.
The use of drugs with a broad spectrum of antimicrobial activity in pediatrics is practiced in cases where it is not possible to quickly identify the causative agent of the disease, while the disease is actively gaining momentum and poses an obvious danger to the child.
The choice of an effective antibiotic is based on the following principle: the drug must exhibit sufficient activity against the suspected pathogen in minimally effective doses and be available in a form appropriate to the child's age. The frequency of administration of such antibiotics should not exceed 4 times a day (for newborns - 2 times a day).
The instructions for the drug should also include instructions on how to calculate the effective dose of the drug for a child of the appropriate age and weight.
The following drugs meet these requirements:
- Penicillin group - amoxicillin, ampicillin, oxacillin and some drugs based on them: Augmentin, Flemoxin, Amoxil, Amoxiclav, etc.
- Cephalosporin group - ceftriaxone, cefuroxime, cefazolin, cefamandole, ceftibuten, cefepime, cefoperazone and some drugs based on them: Zinnat, Cedex, Vinex, Supraks, Azaran, etc.
- Aminoglycosides based on streptomycin and gentamicin
- Carbapenems – Imipenem and Moropenem
- Macrolides – Clarithromycin, Klacid, Sumamed, Macropen, etc.
You can learn about the possibilities of using the drug in childhood from the instructions attached to any medicine. However, this is not a reason to prescribe antimicrobial drugs to your child on your own or change the doctor's prescriptions at your own discretion.
Frequent tonsillitis, bronchitis, pneumonia, otitis, various colds in childhood have long ceased to surprise either doctors or parents. And taking antibiotics for these diseases is not uncommon, since children do not yet have a sense of self-preservation, and they continue to actively move and communicate even during illness, which causes various complications and the addition of other types of infection.
It is important to understand that the mild course of the above-mentioned pathologies does not require taking antibiotics of either a broad or narrow spectrum of action. They are prescribed when the disease progresses to a more severe stage, for example, with purulent tonsillitis. In viral infections, antibiotics are prescribed only if a bacterial infection joins them, which manifests itself in the form of various serious complications of ARVI. In the allergic form of bronchitis, the use of AMP is inappropriate.
Doctors' prescriptions for different pathologies of the respiratory and ENT organs may also differ.
For example, in case of angina, doctors prefer drugs from the macrolide group (Sumamed or Klacid), which are given to children in the form of a suspension. Treatment of complicated purulent angina is carried out mainly with Ceftriaxone (most often in the form of intramuscular injections). Of the cephalosporins for oral administration, Zinnat suspension can be used.
In case of bronchitis, the drugs of choice are often penicillins (Flemoxin, Amoxil, etc.) and cephalosporins for oral administration (Suprax, Cedex). In complicated pathologies, Ceftriaxone is again used.
In case of complications of acute respiratory viral infections and acute respiratory infections, protected penicillins (usually Augmentin or Amoxiclav) and macrolides (Sumamed, Macropen, etc.) are indicated.
Usually antibiotics intended for children have a pleasant taste (often raspberry or orange), so there are no special problems with taking them. But be that as it may, before offering the medicine to the child, you need to find out from what age it can be taken and what side effects can be encountered during therapy with the drug.
Taking penicillins and cephalosporins can cause allergic reactions in a child. In this case, antihistamines Suprastin or Tavegil will help.
Many broad-spectrum antibiotics can lead to the development of dysbacteriosis and vaginal candidiasis in girls. Safe medications such as probiotics will help improve digestion and normalize the body's microflora: Linex, Hilak forte, Probifor, Atsilakt, etc. These same measures will help maintain and even strengthen the baby's immunity.
The best broad-spectrum antibiotic
Having learned about a disease, each of us wants to receive the best treatment using the most effective drugs in order to get rid of it forever in a short time. In the case of infectious diseases, everything seems extremely simple: it is worth dealing with the bacterial pathogen, and the disease will be defeated. But only antimicrobial drugs can destroy pathogenic microorganisms, among which broad-spectrum antibiotics are deservedly popular.
Unfortunately, despite the development of new technologies in pharmaceuticals, scientists have not yet invented a universal medicine capable of fighting absolutely all types of bacterial infections. And this is impossible, since new unstudied microorganisms are constantly appearing in the world, mutations occur, resulting in the formation of new strains of already known bacteria, which even new generation drugs cannot cope with.
In connection with the above, the concept of "the best broad-spectrum antibiotic" should be considered only in the concept of a certain pathology. It is not for nothing that experienced doctors, in most cases giving preference to protected penicillins and cephalosporins with their high activity against a huge number of pathogens, choose other antibiotics for pneumonia and other severe pathologies: macrolides and fluoroquinolones.
It would seem, what's the difference if all these drugs have a broad spectrum of action? But there is a difference. Some AMPs are more effective against aerobic bacteria, which means they make sense to use for the treatment of respiratory diseases. Others are able to cope with Pseudomonas aeruginosa, which means their use will be more useful in the treatment of purulent wounds and abscesses. It turns out that there is no point in treating the same bronchitis with a drug that is effective in combating anaerobes (bacteria that do not need oxygen for life and development) and Pseudomonas aeruginosa.
The best drug will always be the one that is targeted against a specific pathogen. In this regard, drugs with a narrow spectrum of action even win. However, only if the pathogen is precisely identified.
If there is no possibility to quickly identify the pathogen, a broad-spectrum drug should be prescribed taking into account all possible pathogens. Thus, in case of infectious lesions of the respiratory organs, the drugs of choice are "Augmentin", "Amoxicillin", "Ceftriaxone", "Sumamed", because these drugs cover virtually the entire spectrum of possible pathogens of respiratory infections.
The same requirement must be observed when antibiotic therapy is prescribed for preventive purposes. There is no point in fighting bacteria that simply cannot exist in a specific pathology.
But that's not all. An effective broad-spectrum antibiotic should not only treat well, but also not harm the person it treats. A good antibiotic is one that is prescribed thoughtfully, after a final diagnosis has been made and corresponds to it, and also has the fewest side effects and is easy to use. So, for small children, Augmentin in tablet form cannot be called the best antibiotic, but the suspension will definitely help the baby fight the disease without causing discomfort.
When prescribing drugs, it is necessary to take into account contraindications for use, because if, having a therapeutic effect on one organ, an antibiotic at the same time cripples another, it cannot be called the best. For example, if a patient is intolerant to penicillins, then, despite their high effectiveness in certain pathologies, the drugs will have to be replaced with drugs of another group, so as not to harm the patient, because severe allergic reactions can even end in death.
Which antibiotic is better: cheap or expensive?
Having studied the therapist's prescription and the state of their financial affairs, many come to the conclusion that doctors deliberately do not prescribe cheap and inexpensive broad-spectrum antibiotics, giving preference to more expensive ones. There is a widespread opinion that in this way they help out pharmacies.
For example, why prescribe the expensive "Augmentin" if there is a cheaper analogue "Amoxicillin"? In fact, the active substance of the drugs is the same, which means that, in theory, they should have the same effect. But everything is not so simple. "Amoxicillin" is a semi-synthetic penicillin, while the more modern "Augmentin" is already a protected penicillin with a wider spectrum of action and resistance to penicillinase produced by some strains of bacteria.
In principle, treatment can be started with Amoxicillin, but where is the guarantee that the bacterial pathogen will not be resistant to it, which means that after the course has not brought relief from the symptoms of the disease, you will have to buy the more expensive Augmentin or another equally cheap drug. So where is the savings?
True, there are drugs that are completely identical in both the active substance and the pharmacological action, and the difference in price is caused by the difference in the composition of auxiliary components and the policy of the manufacturers. For example, Amoxicillin and Flemoxin, Sumamed and Azithromycin, Rulid and Roxithromycin. Usually, a cheap analogue is an older drug, and its name often coincides with the active substance.
Such drugs are interchangeable, but the final decision on the possibility of one drug over another should be thought out and discussed with the attending physician. Doctors are also people, therefore, having understood the patient's situation, they will always be able to advise cheaper, but quite effective analogues. And this will be better than choosing a drug yourself.
It is clear that the price of expensive broad-spectrum antibiotics, in addition to the cost of components and work, also includes advertising costs. By the way, these costs often become the main part of the announced price. However, the inclusion of more expensive auxiliary components in the composition of the drug also pursues its own goals. It is believed that expensive oral agents have a more gentle effect on the gastrointestinal mucosa and are less toxic. Coated tablets and capsules deliver the active substance to the intestines, where it is absorbed into the blood, and are not sprayed in the stomach, it is subject to destruction by gastric acid. Alas, inexpensive drugs do not always have such forms of release.
As a rule, Russian broad-spectrum antibiotics and domestic AMPs are much cheaper than imported ones. The quality and effectiveness of the drugs may be the same, but the price will differ significantly. This is understandable, because the price of foreign drugs, in addition to transportation and registration (which, by the way, is much more expensive than in the case of domestic ones), also includes a considerable customs fee. Take, for example, the cheap Russian "Clarithromycin" and "Klacid" made in Italy, which is approximately 5 times more expensive than its analogue.
It is impossible to say that Russian analogues of well-known antibiotics are worse than foreign ones. In this case, competition is not based on product quality, but on price and popularity of the manufacturer. And here, each product has its own buyer. Some do not trust domestic manufacturers, so they buy an imported analogue, although not cheap. And others are guided by price.
On the other hand, sometimes there is no choice. For example, the drug from the fluoroquinolone group "Gatifloxacin" and drugs based on gatifloxacin can be called Indian broad-spectrum antibiotics, since most of them are produced in India. And there are quite a lot of such drugs among broad-spectrum antibiotics. It is impossible to say for sure whether this is good or bad. After all, drugs from India are famous for their good quality and relatively low price.
Or here is the situation with the French broad-spectrum antibiotic "Rovamycin". According to reviews, the drug copes well with its task, but its cost (almost 200 UAH for 10 tablets) will seem quite high to many. The drug has domestic analogues "Rovacid" (Kyiv) and "Starket" (Kharkov and Boryspil), as well as a Russian analogue "Spiramycin". These drugs are much cheaper than "Rovamycin", but unlike the French drug, they are not so easy to find in pharmacies.
Safe broad-spectrum antibiotics
Every time you buy antibiotics prescribed by a doctor, you think about the harm that drugs that kill other living organisms can cause to your body. And if you also take into account the wide spectrum of activity of new generation antibiotics, then willy-nilly the thought arises about how safe they are for humans.
Manufacturers of drugs and doctors claim that in the absence of contraindications and in the prescribed dosage, AMPs should not harm human health. But this statement is true in most cases with a short course of treatment.
Of all the types of broad-spectrum antibiotics, the safest are penicillin-type antibiotics and macrolides. These are the drugs that pediatricians most often prescribe to children.
The greatest danger of penicillins is considered to be the development of dyspeptic phenomena and allergic reactions. Macrolides are generally considered the least toxic drugs with rare and mild side effects. As for cephalosporins, short-term treatment with drugs of this group (for example, "Ceftriaxone") is prescribed even to small children, which means that these drugs can also be classified as relatively safe.
The safety of drugs can be judged by the frequency of their prescription for therapy of children and pregnant women. The drugs of choice in this regard were and remain penicillins in the absence of allergic reactions.
If there is intolerance to penicillins, they are replaced by cephalosporins and macrolides. The safest macrolides during pregnancy are erythromycin-based drugs, in second place are such active substances as clarithromycin, azithromycin, josamycin and roxithromycin.
When treating tuberculosis in pregnant women, tetracyclines are acceptable. The drug of choice in this case is Rifampicin.
The danger of antibiotics usually lies in their incorrect use. Many broad-spectrum antibiotics are sold without a prescription. These are mainly drugs most often used in the treatment of respiratory diseases. Some people think that if a drug can be bought without a prescription, it means that it is generally safe and there is no need to follow the instructions. This is fundamentally wrong. With this approach to antibiotic therapy, even the safest drug can cause harm to health.
Natural broad-spectrum antibiotic
People have known for a long time that there are products and plants in nature that can destroy pathogenic bacteria. This fact is even confirmed by the history of the appearance of the first antibiotic - penicillin, the prototype of which was mold.
Many herbs and plants are natural antibiotics. Among the herbs, the following are famous for their pronounced bactericidal and bacteriostatic action: yarrow, wormwood, wild rosemary, tansy, plantain, motherwort. Chamomile, calendula, celandine, eucalyptus, eleutherococcus, sage, as well as Kalanchoe and aloe also have antimicrobial properties. All these plants are active against several groups of bacteria, and collections of such herbs can be considered a full-fledged broad-spectrum AMP.
Antibacterial properties are also characteristic of many plants that we are used to seeing on our table. These are garlic, ginger, onion, horseradish, pomegranate, cranberry, lingonberry. And cranberry is not only an antibiotic, but also an irreplaceable vitamin and mineral complex.
However, the most powerful natural broad-spectrum antibiotics are considered to be bee products such as honey and propolis.
Honey itself is effective against white and golden staphylococcus, proteus, enterobacteria, and E. coli. But when mixed with decoctions and herbal juices that have antibacterial properties, it becomes a notorious killer of pathogenic microorganisms.
But neither herbs, nor plants, nor honey can compare in strength with propolis, which is deservedly considered the strongest antimicrobial drug. Propolis is used both in its natural form (chewed), and in the form of ointments and infusions. Propolis tincture can even be bought at a pharmacy, because its medicinal properties are not rejected by traditional medicine.
Propolis is used to treat various infectious pathologies of the oral cavity and ENT organs. As a therapeutic and preventive agent, it has proven itself well in the treatment of wounds, burns, frostbite (in the form of ointments and infusions). Propolis also effectively fights fungal infections.
Mountain resin – mumiyo – acts similarly to propolis. Altai mumiyo is especially popular among fans of traditional medicine, who buy the product online. However, it can also be bought in pharmacies, both in its natural form and in capsules for oral administration.
Which broad-spectrum antibiotic to choose (natural or synthetic) is, of course, up to the patient to decide. In doing so, one must always be guided by the principle of "do no harm!" And following this principle will be much easier if the patient consults with the attending physician about taking any antibacterial agent, rather than making the decision on his own.
Attention!
To simplify the perception of information, this instruction for use of the drug "New and best broad-spectrum antibiotics: names of tablets, ointments, drops, suspensions" translated and presented in a special form on the basis of the official instructions for medical use of the drug. Before use read the annotation that came directly to medicines.
Description provided for informational purposes and is not a guide to self-healing. The need for this drug, the purpose of the treatment regimen, methods and dose of the drug is determined solely by the attending physician. Self-medication is dangerous for your health.

