Medical expert of the article
New publications
Bone exostosis
Last reviewed: 29.06.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
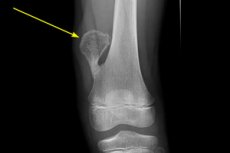
Bone exostosis (from the Greek exo, "something outside or beyond" and the suffix-osis, which in medicine means a pathologic condition or process) is defined as a benign outgrowth of bone tissue extending outward or over an existing bone.
Epidemiology
Among bone neoplasms, exostoses account for approximately 4-4.5% of cases.
The most common of the benign bone tumors, bone cartilage exostoses or osteochondromas, occur in 3% of the population, and in 75% of cases they are solitary masses.
Multiple osteochondromas occur in hereditary multiple exostoses, the frequency of which does not exceed one case per 50,000 people. [1]
According to various studies, the prevalence of buccal exostoses ranges from 0.09% to nearly 19%, and 5% of bone and cartilage exostoses involve the pelvic bones. [2]
Causes of the exostosis of bone
Exostosis is also called bone spur and osteoma of bone. But while an exostosis affecting any bone is a non-tumor bone outgrowth of dense lamellar bone, the periosteal layers of which usually have no trabeculae (supporting beams) or medullary spaces, then osteoma is a benign bone tumor of predominantly craniofacial localization (primarily in the paranasal sinuses), and the bone tissue forming it may be lamellar and spongy - with vascular channels and inclusions of bone marrow and fat.
Common causes of exostosis include trauma, chronic bone irritation, or a disorder of bone development (traceable to a family history of congenital imperfect bone formation). Idiopathic exostosis is not uncommon, where the exact etiology is unknown.
For example, exostosis of the external auditory canal is thought to result from irritation of its bony walls by cold water and wind; exostoses form in the medial part of the external auditory canal - at the suture lines of the tympanic, temporal, and mastoid bones of the bony canal. [3], [4]
Exostosis of the jaw bone is called buccal bone exostosis and often occurs in early adolescence after damage to the gums and the underlying bony structures (also due to malocclusions of the teeth). [5] By the way, exostosis of the gingival bone is impossible, as the gums are the mucous membrane of the alveolar process of the upper and alveolar part of the lower jaw, and its own lamina consists of loose connective tissue. The most common exostoses of the jaws are torus mandibularis - nodular protrusions of the dense cortical layer of bone on the surface of the mandible adjacent to the tongue (near the premolars and molars), as well as exostosis along the midline of the hard palate - torus palatinus. [6]
Subnail exostosis, which most commonly affects the big toe, index and middle finger, is associated with trauma or chronic infection of the nail bed.
When a bone outgrowth is covered by cartilage, it is a bone and cartilage exostosis called an osteochondroma, which can be on the long bones of the lower leg-tibia exostosis (os tibia) and fibula exostosis (os fibula); on the scapula (scapula) and on the pelvic bones, sciatic bone exostosis (os ischii).
Causes of bone exostosis in children
Exostosis of bone in a child and osteochondromas - benign skeletal tumors in children - can be either solitary bone overgrowth or multiple (on multiple bones).
For example, bone exostosis often occurs in the healing of a fracture with partial or complete detachment of a bone fragment at the site of muscle tendon attachment, which orthopedists explain by congenital weakness of the apophyses (bone outgrowths to which muscles are attached).
The etiology of benign bone growths is also seen in reactive bone formation - hyperplastic periosteal reaction, in which the formation of new bone occurs in response to damage or other stimuli surrounding the bone periosteum (periosteum), which has an internal osteogenic (bone-forming) layer.
Osteochondroma, i.e. Bone and cartilage exostosis of the epiphysis (enlarged end section) of the femur and tibia, as well as exostosis of the talus of the tarsal bone is formed in hereditary Trevor's disease (hemimelic epiphyseal dysplasia or tarsoepiphyseal aclasia). [7]
Among the causes noted and such systemic pathologies as: hereditary pseudohypoparathyroidism (genetically determined resistance of target organs or to parathyroid hormone), infantile cortical hyperostosis (Caffey's disease); Gardner's syndrome; Albright hereditary osteodystrophy; systemic ossifying periostosis (Marie-Bemberger syndrome); progressive ossifying myositis (Münheimer's disease), etc.
Multiple bone exostoses (multiple exostosis syndrome, diaphyseal aklasia or hereditary multiple osteochondromas) is an autosomal dominant inherited disorder usually diagnosed in children aged 3-5 years. [8] The area most commonly affected is the knees, and there is also bone overgrowth on the long bones of the upper extremities: exostosis of the humerus (os humerus), exostosis of the radius (os radius), and exostosis of the ulna (os ulna). Less common localizations include the shoulder blades, hands, ribs, vertebrae, and pelvis. [9]
Exostoses in children and adolescents stop growing after the epiphyseal plates (lamina epiphysialis) mature.
Risk factors
Factors that increase the risk of exostoses include: trauma; constant physical overload on certain skeletal segments; heredity and sporadic genetic mutations leading to congenital anomalies and systemic skeletal diseases; secondary hyperparathyroidism (which develops due to low vitamin D levels); degenerative-dystrophic joint changes, arthritis and osteoarthritis; foot deformity in diabetes; and posture disorders.
Pathogenesis
Explaining the pathogenesis of bone exostosis, experts note that the overgrowth of bone tissue refers it to hyperostosis, which has different mechanisms of formation.
One of the mechanisms of exostosis formation, proposed by Rudolf Virchow, is associated with the displacement of hyaline cartilage of the epiphyseal plate (cartilaginous growth plate), which causes lateral bone growth from the metaphysis - adjacent to the epiphyseal plate of tubular bones.
Another pathogenetic mechanism may be based on the dysfunction of the main cells of bone tissue - osteocytes, which are not capable of mitotic division, but actively participate in the metabolism of bone matrix because they are mechanosensory cells. Various mechanical forces acting on bone can stimulate osteocytes, resulting in changes in the flow of intercellular fluid and deformation of the bone intercellular substance (bone matrix), which forms the majority of bone mass.
Osteocytes produce the protein sclerostin (encoded by the SOST gene), which suppresses bone formation and the transmission of intracellular signals between bone-forming osteoblasts and osteoclasts responsible for bone resorption, which is crucial for the continuous process of bone remodeling.
In addition, sclerostin counteracts the activity of bone morphogenetic protein BMP3 - osteogenin, which belongs to transforming growth factors-beta (TGF-beta); it induces osteogenic differentiation and exhibits bone-forming activity. If the synthesis of these proteins and their physiological ratio are disturbed, the regulation of bone formation is also disturbed.
In multiple exostoses syndrome, pathogenesis is caused by mutations in EXT1 and EXT2 genes encoding glycosyltransferase proteins required for the biosynthesis of heparan sulfate (a glycoprotein of the extracellular matrix of all tissues). It was found that complete absence or accumulation of heparansulfate, as well as chain shortening in its structure, disrupts the processes of differentiation and proliferation of epiphyseal plate chondrocytes and proper bone growth. [10]
Symptoms of the exostosis of bone
Exostoses can occur in any bone and are either asymptomatic (and detected incidentally on radiologic examination) or - when the bony overgrowth puts pressure on peripheral nerves and blood vessels - cause chronic pain of varying intensity.
Depending on their shape, size and location, exostoses lead to restricted movement and functional impairment. For example, hearing loss can be observed with an exostosis of the ear canal. Buccal exostosis in the form of torus mandibularis, a series of smooth bony nodules along the facial alveolar part of the mandible, causes symptoms such as difficulty in chewing, swallowing, and articulation; superficial ulceration of the adjacent mucosa may occur.
Exostosis of the frontal bone of the skull (os frontale) is defined as osteoma of the frontal sinus, which can manifest as pain and pressure in the frontal sinuses; with compression on the ocular part of the bone forming the upper wall of the eye sockets, there is protrusion of the eyeballs, decreased vision, and problems with eyelid mobility. [11]
Exostosis of the occipital bone (os occipitale) at the occipital foramen is usually noticed incidentally on radiography, although it may become symptomatic with complaints of painful swelling of the bone at the back of the neck causing pain (especially in the supine position).
A calcaneal exostosis (os calcaneum) is heel spur or Haglund's deformity, a bony cartilaginous growth on the back of the heel, also called a retrocalcaneal exostosis. The main symptoms are a "bump on the heel" and pain in the heel when walking and at rest. [12] See also - causes of heel spurs
Pain, tingling in the upper part of the foot and toes are symptoms that can be caused by metatarsal wedge exostosis - metatarsal exostosis (osis metatarsus), which forms on the upper part of the foot above the arch. Exostosis of the metatarsal head may be manifested by pain in the metatarsophalangeal joint when walking (with its intensification when the weight of the body is transferred to the forefoot), a feeling of stiffness of this joint in the morning; interfinger neuralgia may develop and a callus may form over the bony prominence.
Exostosis of the talus bone, one of the tarsal bones that forms the bottom of the ankle joint, is called an ankle bone spur, which can compress the surrounding soft tissues of the ankle, causing swelling and soreness at the front of the ankle joint, as well as pain when the foot is dorsally flexed.
Tibial exostosis is most often localized in the proximal tibia; and peroneal exostosis of the tibia is also formed, mainly close to the knee joint. In both cases, nearby nerve endings may be compressed, causing pain, compression neuropathies with numbness and paresthesias; there is muscle dystonia, movement disorders, and curvature of the lower leg bones.
Femoral osteochondroma or cartilaginous exostosis of the femur (os femoris), which occurs in the distal diaphysis of the femur and extends into the metaphyseal region, can cause pain in the knee along the midline of the joint. Pain of varying intensity is also caused by the indentation of the exostosis into the thigh muscles and their deformation. When a bony outgrowth is formed in the area of the trochanter minor, there is a narrowing of the sciatic-femoral space and swelling of the quadriceps femoris muscle, and pain is felt in the hip joint. [13]
Exostosis of the metacarpal bones (osis metacarpi) of the hand is a well-defined bony malformation with a wide base, protruding into the soft tissues and well palpable. Typical complaints are pain, curvature of the fingers, numbness and limited mobility.
Isolated bone and cartilage exostosis of the iliac bone (os ilium) of the pelvis may manifest with soft tissue swelling and discomfort in the lumbar region.
Pubic exostosis or exostosis of the brow bone (os pubis), a painless bone mass or increasing painful lump in the groin area, can cause urethral compression with problems urinating (and, in men, discomfort during intercourse).
In the vast majority of patients, clinical symptoms of hereditary multiple bone exostosis (which is most often localized in the peri-epiphyseal regions of long bones) manifest by the time they reach adolescence and include: constant pain or numbness due to nerve compression; impaired circulation; varying limb lengths; tendon and muscle damage; angular deformities of the upper and lower extremities; and limited range of motion in the joints articulating the affected bones. [14]
Complications and consequences
Complications of exostosis of the external auditory canal include obstruction causing recurrent otitis externa with pain or tinnitus, as well as conductive hearing loss.
Exostosis of the jaw bone can increase bleeding gums when brushing teeth and creates a threat to periodontal health due to difficulty with oral hygiene.
In addition to reactive myositis, the formation of adventitious bursae with the development of bursitis, a negative consequence of osteochondroma, a bone and cartilage exostosis of the proximal tibia that protrudes into the hamstring fossa, is thrombosis of the hamstring artery and acute ischemia of the lower limb.
If exostosis of the metatarsal head or talus is present, anterior impingement syndrome of the ankle joint develops.
The consequences of multiple exostosis syndrome include mild growth retardation, limb asymmetry, curvature and shortening of one or both bones of the forearm, wrist joint deformity (Madelung's deformity), valgus deformity of the knee or ankle joint.
It should be kept in mind that an increase in the size of an exostosis occurring after skeletal maturation should lead one to assume its malignant transformation. Malignization of an existing osteochondroma into secondary periprosthetic osteo- or chondrosarcoma is the most dangerous complication of multiple bone exostosis, affecting about 4% of patients.
Diagnostics of the exostosis of bone
Diagnosis of exostoses is made based on patient examination and bone examination, which is used for:
- Bone x-rays;
- Bone scintigraphy;
- Bone ultrasound;
- Magnetic resonance imaging (MRI) of bone structures (including joints).
Methods of visualizing bone overgrowth vary depending on its location, for example, panoramic radiographs of the maxillofacial region are used in dentistry and otoscopy is used in otolaryngology.
Differential diagnosis
Differential diagnosis includes: simple or aneurysmal bone cyst, eosinophilic granuloma of bone, chronic ostitis, osteomyelitis, deforming osteodystrophy, benign osteoid osteoma of various localizations, periosteal chondroma, progressive ossifying fibrodysplasia, osteosarcoma, and osteoblastoma.
Osteophytes - bony growths secondary to osteoarthritis on the edges of joints - should also be differentiated.
Who to contact?
Treatment of the exostosis of bone
The etiology and symptomatology of bone exostoses determine the tactics of their treatment. In case of asymptomatic bone and cartilaginous growths, no therapy is performed.
Conservative treatment for Haglund's deformity (exostosis of the heel bone) includes: wearing lower-heeled shoes, wearing open-back shoes, using orthopedic insoles in shoes, physical therapy (including massage and ultrasound therapy), taking non-steroidal anti-inflammatory drugs (NSAIDs) and other painkillers. External remedies can also relieve pain, such as Diclofenac or Nimesulide joint pain relieving ointments.
Sometimes this bone growth is removed. For more information, see. - remedies and treatments for heel spurs
For occipital bone exostosis, soft pillows and anesthesia may be effective; however, in patients whose symptoms do not respond to medication and physical therapy, surgical excision of the bony outgrowth results in improvement.
In case of stenosis of the external auditory canal by bony outgrowths formed in it, their removal - osteotomy - is indicated.
It should be understood that drug therapy, including corticosteroid injections, cannot "dissolve" the exostosis or "separate" it from the bone.
Treatment for hereditary multiple exostosis involves surgical removal of the bone malformations that cause pain, discomfort and restricted movement. It is also performed to restore joint mobility, improve circulation or for cosmetic purposes.
In case of lesions in the distal tibia, fibula and radius, surgical excision of osteochondroma should be performed to prevent deformity of the corresponding joints. And to correct displacement of the bones of the lower limbs and wrists, a surgical intervention such as hemiepiphysiodesis can be performed.
Prevention
In many cases, bone exostosis cannot be prevented, so the general recommendations for preventing this pathology include protecting the ear canals from cold water (when practicing water sports), wearing comfortable shoes, correcting an improper bite, developing correct posture, and maintaining a healthy weight and fitness.
Forecast
Prognosis also depends on the cause of bone and cartilage exostoses. For example, even after surgical removal of an exostosis, local recurrence of osteochondroma is noted in almost 12% of cases, requiring repeated operations performed to eliminate complaints associated with bone exostoses.

