Medical expert of the article
New publications
Adamantinoma of the upper and lower jaw
Last reviewed: 04.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
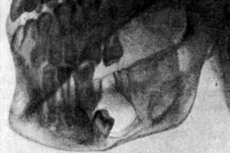
A very rare disease, adamantinoma, is a malignant formation of the bone system. The specificity of adamantinoma is that this tumor arises from cellular enamel structures. The disease is currently still at the stage of study, since its etiology still has many controversial and unclear points.
Epidemiology
Adamantinoma is considered a very rare malignant tumor (locally malignant in 0.15%). According to statistics, the frequency of detection of adamantinoma ranges from 0.3 to 0.48% of all registered oncological bone pathologies.
Adamantinoma mainly affects men aged 50-60. However, there have been cases where the disease was detected in women aged 25-35, and even in newborns.
The predominant localization of adamantinoma is the lower jaw area (in 90% of patients). However, in some cases, the pathology was recorded in the tibia.
Causes adamantinomas
The reasons for the tumor's appearance remain a mystery to scientists today. There is still no clear answer. There are only assumptions that certain authors of scientific papers tend to make.
Some experts believe that adamantinoma is a consequence of abnormal development of the tooth germ. Other scientists insist that the origin of adamantinoma is associated with the epithelial structures of the mucous tissues of the oral cavity. The third group of specialists is sure that the tumor originates from the odontogenic islands of Malassez - elements of the epithelium.
In addition, there is a fourth version - the appearance of adamantinoma from the epithelial layer of follicular cystic formations.
Since the causes of the tumor are unknown, many risk factors are also questioned. Previously, it was assumed that the disease could be caused by tissue trauma or damage due to some third-party pathologies.
Pathogenesis
Previously, the disease was identified with endothelioma, and only since 1913 the pathology was described as an independent disease (at that time, it was a primary adamantinoma of the tibia). At that time, doctors assumed the theoretical origin of the tumor from the embryonic epithelial tissue of the dentin germ. This version existed for quite a long time - until scientists pointed out the possible histogenesis of the neoplasm.
In the 1930s, adamantinoma was classified as a primary epithelial tumor. However, this did not put an end to the pathogenesis of the disease. Already 10-20 years later, specialists described cases where adamantinoma appeared in bones against the background of fibrous dysplasia. As a result, theories of the tumor's origin began to diverge even more diametrically: they suggested vascular etiology, a type of angioblastoma, etc.
At the moment, the pathogenetic mechanism has not been fully clarified. Most experts have decided that it is most logical to classify adamantinomas as varieties of endothelioma, since these tumors have a similar structure. By conducting careful electron microscopy, scientists have indicated a complex cellular structure of the neoplasm, and its histology is variable, which adds problems in describing the tumor.
Symptoms adamantinomas
The development of adamantinoma is usually slow, gradual, and painless.
The first signs may be expressed in the appearance of edema or slight swelling. However, as practice shows, several years (and even several decades) may pass between the onset of edema and seeking medical help.
In isolated cases, adamantinoma develops rapidly, violently, accompanied by pronounced local and general symptoms, with the spread of metastases through the blood and lymph.
If adamantinoma develops in the lower jaw area, then over time facial deformation is observed, the patient begins to experience difficulties with speech, swallowing, chewing, and painful sensations appear. If the tumor reaches large sizes, then bleeding, ulceration of the mucous membrane, and the appearance of pathological fractures of the jaw bones are possible.
Adamantinoma of the lower jaw is most often localized in the area of the angle or branch. In most cases, it resembles a cyst, but does not have a clearly defined capsule. If such "cysts" are located multiple times, they merge, transforming into large formations. Usually, this is a gray tumor, elastic, pliable. The cavities of the neoplasm contain yellowish contents (sometimes of colloidal consistency). The bone tissue surrounding the adamantinoma is distinguished by its thinness. The tumor can grow deep, leading to deformation of the facial bones.
Adamantinoma of the tibia develops with the formation of a significant diffuse destructive focus. In some cases, a fusion of several spherical foci is observed, sometimes pathological violations of the integrity of the bone are detected. The appearance of primary destructive changes in the cortical layer of the long bone, followed by its destruction and damage to the bone marrow cavity and diaphysis is considered typical.
Adamantinoma of the upper jaw is extremely rare - only in isolated cases. If the upper jaw is affected, the patient may experience difficulties with nasal breathing. Sometimes there are visual disturbances in the form of double vision, increased lacrimation. The sensitivity of the skin in the upper half of the face may be impaired. Some patients note the appearance of aching pain, like a regular toothache. Deformation of the face with maxillary localization is not observed.
Stages
According to the structural type, two types of adamantinoma are distinguished: solid and polycystic. In fact, these types do not belong to independent forms, but occur one after another.
The solid type of adamantinoma is the initial stage of the neoplasm, which develops at a more accelerated rate, unlike the polycystic variant. Solid adamantinoma is a nodular formation of varying density, with a grayish or reddish tint, with or without a capsule.
Polycystic adamantinoma is a combination of several cystic formations containing light or brown discharge. Microscopically, one can detect the presence of typical branched epithelial strands or inclusions with layers of connective tissue, with blood and lymphatic vessels. In the central part of the complex epithelium, there are star-shaped cellular structures.
The described stages have much in common with the structural changes of the growing enamel dental organ.
There is also another histological classification of adamantinoma:
- granular cell tumor;
- basal cell tumor;
- acanthomatous (keratin) tumor;
- pleomorphic tumor (with the presence of epithelial strands);
- follicular tumor.
Complications and consequences
Adamantinoma is often complicated by inflammatory diseases that lead to the formation of ulcers and fistulas with serous or purulent discharge that enter the oral cavity. Trauma and mechanical damage to the neoplasm can provoke the development of a purulent inflammatory process or purulent osteomyelitis of the nearby bone tissue. Bone melting and destructive osteolysis processes, which are a consequence of infiltration, can cause the appearance of a pathological bone fracture.
Locally malignant adamantinoma can transform into a full-fledged malignant process, with the spread of metastases by lymphogenous and hematogenous routes. This happens in approximately 4.5% of cases: most often, such a complication affects patients who did not receive the necessary treatment in a timely manner.
Diagnostics adamantinomas
Adamantinoma in the jaw is detected during an examination of the oral cavity by a dentist. The diagnosis is based on the results of the examination, questioning the patient, and the presence of characteristic complaints.
Instrumental diagnostics involves the use of radiography, which is carried out in different projections: panoramic, intracavitary, lateral and axial projections. The resulting images allow us to assess the size and stage of the painful focus, as well as the condition of the damaged bone.
The main typical radiological signs of adamantinoma are:
- the presence of a solid tumor, which has the appearance of small dark nodules divided by bone membranes;
- the presence of a cystic tumor, with areas of destruction or with affected areas divided by bone membranes;
- swelling or bay-shaped mandibular deformity;
- sclerosis and thinning of the mandibular bones;
- destructive changes in the alveolar process, deformation and disruption of the placement of dental roots (not in all cases);
- destructive processes in the angular region of the lower jaw, up to the coronoid process.
The affected area may be small in size or spread over large areas of tissue: the doctor will definitely notice this during the examination.
An important component of the diagnostic process for adamantinoma is the confirmation or exclusion of the oncological nature of the disease. To do this, the doctor will puncture the neoplasm. Subsequently, cytology tests are performed on the collected fluid. In the case of a benign process, the analysis will indicate the presence of fibrin, blood cells, cholesterol, lipid-granular and stellate cells.
Differential diagnosis
Differential diagnostics of adamantinoma is carried out with inflammatory dental cysts, carcinoma and cyst of the salivary glands, osteoblastoclastoma and other tumor formations.
Who to contact?
Treatment adamantinomas
Adamantinoma can only be completely cured by surgery. If the disease is accompanied by purulent processes, then antibacterial treatment with oral cavity sanitation is prescribed beforehand.
Surgical treatment for adamantinoma may vary - it depends on the size of the neoplasm and the extent to which the process has spread to nearby tissues. If the pathology was detected at an early stage of development, then removal can be carried out without changing the integrity of the jaw - such treatment is more acceptable, since it allows to preserve its functionality to one degree or another. During surgical intervention after enucleation of the tumor, the cavity walls are washed with a phenol solution. This allows for necrosis processes in the remaining epithelial tissues, which serves as a preventive measure for the recurrence of adamantinoma.
If the neoplasm has grown to a significant size, the surgeon removes it, partially affecting the integrity of the jaw bone. When removing a large area of bone tissue, bone plastic surgery using orthopedic structures is possible.
Treatment of adamantinoma after surgery involves taking antibiotics, physiotherapy and dietary nutrition with the exclusion of coarse and dense foods.
The speed of recovery of the body in the postoperative period depends on both regular compliance with the doctor's orders and adherence to the general rules of rehabilitation.
For 24 hours after the operation, the patient must be provided with complete rest and bed rest. Rest and good sleep will help the body recover faster. Cold compresses can be used to relieve postoperative swelling and pain. They are applied for about 15 minutes.
If the surgery was performed on the jaw bones, then the patient will be prescribed a diet for some time, with the use of only pureed and liquid food. If the adamantinoma was removed from other bones, then the rehabilitation scheme is prescribed by the doctor on an individual basis, taking into account the patient's condition and his motor abilities.
Medicines
The medications to be taken after surgery to remove adamantinoma and in what quantities should be determined only by the attending physician. Most often, the physician may recommend taking vitamin complexes (vitamins A, E and C are especially important). The simplest and most accessible medications in this category are ascorbic acid pills, Aevit capsules, Undevit and Hexavit pills. Any disease, including adamantinoma, occurs with a decrease in the body's defenses. If measures are taken in a timely manner and the immune system is strengthened, it is possible not only to prevent the development of complications, but also to prevent a relapse of the neoplasm. The physician's treatment prescriptions during the rehabilitation period must necessarily include vitamins - to support the body and strengthen its internal protective reserves.
Antibiotics and sulfonamides are used to prevent infection and to eliminate signs of inflammation in damaged tissues. Among such drugs, the most popular are Ciprofloxacin, Ampicillin, Etazol, Sulfazin.
Additionally, the doctor may prescribe medications that improve blood circulation: Nicotinic acid, Trental, Pentoxifylline.
Nonsteroidal anti-inflammatory drugs will help relieve pain and stabilize body temperature. The most popular drugs in this category are Diclofenac, Ibuprofen, Acetylsalicylic acid.
Method of administration and dosage |
Side effects |
Special instructions |
|
Ciprofloxacin |
Prescribed orally at 0.125-0.5 g twice a day for 1-2 weeks. |
Rarely – allergy, change in taste, abdominal pain, diarrhea. |
The tablets should not be taken with alkaline mineral water. |
Sulfazin |
Take 1-2 g daily until the patient’s condition normalizes. |
Sometimes – nausea, vomiting, hematuria. |
The drug is not recommended during pregnancy. |
Pentoxifylline |
Take orally, 2 tablets (0.2 g) three times a day after meals, without chewing. Duration of treatment is 2-3 weeks. |
Headache, sleep disturbance, pain in the heart area, dyspepsia. |
The drug is contraindicated during pregnancy and for the treatment of children under 12 years of age. |
Ibuprofen |
Prescribed in tablets of 200 mg up to 4 times a day, preferably for no more than five days. |
Abdominal pain, ringing in the ears, dizziness, sleep disturbances, allergies. |
The drug is used in short courses, with monitoring of the state of the digestive system. |
Physiotherapy treatment
Physiotherapeutic methods are an important addition to conservative treatment of adamantinoma in the postoperative period. Physiotherapeutic procedures will help reduce the intensity of inflammation, relieve pain and prevent the development of infection in the wound.
As a rule, doctors recommend paying attention to the following types of treatment:
- ultraviolet irradiation of the mucous membrane using a short or integral radiation spectrum, starting with 2 biodoses, gradually increasing to 5-6 biodoses (per course - up to 6 sessions);
- ten-minute fluctuation in the amount of five to six sessions;
- SMV therapy from 5 to 7 minutes per procedure;
- electrophoresis with anesthetics (for pain), for example, with trimecaine;
- magnetic therapy with a pulsating magnetic field in a pulse mode (1:1 or 1:2), for 25-30 minutes, in the amount of 12-16 procedures.
Folk remedies
As an addition to standard medications for adamantinoma, the doctor may recommend tonic and pain-relieving recipes of traditional medicine. For example, such:
- For tibial adamantinoma, use a compress with a medicine based on white acacia: mix acacia flowers with table salt in a 10:1 ratio, leave for at least three hours and apply as a compress to the affected area. Do not apply such a compress if the skin is damaged - has cracks, scratches, cuts.
- With adamantinoma, horse chestnut tincture will help alleviate the condition. The plant flowers are poured with vodka in a 1:1 ratio and kept in a dark place for 20 days. The tincture is taken orally, 5 ml three times a day before meals, for a month.
- To recover after surgery to remove adamantinoma, use the following drink: mix 50 ml of fresh St. John's wort juice with 200 ml of milk and drink in the morning on an empty stomach.
- In the postoperative period, it is useful to drink compote from sour apples - for example, from "Antonovka". To prepare it, three medium apples are cut into slices, filled with water, brought to a boil, removed from the heat and covered with a lid. After three hours, the drink can be drunk, preferably on an empty stomach.
Herbal treatment
In the treatment of jaw adamantinoma, rinsing the mouth is considered an important procedure that helps to get rid of possible infection, reduce pain, and prevent and warn of inflammation. The use of herbal decoctions and infusions successfully complements the traditional treatment prescribed by the doctor.
To alleviate the condition with adamantinoma, such plants as sage, chamomile, calendula, thyme, hyssop, horsetail, eucalyptus leaves, thyme, yarrow have a good effect. To prepare a medicinal infusion, two tablespoons of herbal raw materials are poured with 200 ml of boiling water, allowed to brew and filtered. The resulting infusion is used to rinse the mouth - the more often the better.
Sage has excellent anti-inflammatory and antiseptic properties. To prepare the medicine, boil 1 tbsp of the plant for 20 minutes in 200 ml of boiling water. The decoction is used for rinsing.
To increase the effectiveness of the remedy suggested above, you can add a little crushed rhizome of the scaly-sided plant to it.
Rinsing should be done at least 10 times a day. Infusions should be prepared every day so that they are fresh. The rinse liquid should not be hot: the optimal temperature is about 36-37°C.
Homeopathy
Homeopathic medicines are prescribed on an individual basis, taking into account the patient’s characteristics and the stage of the disease.
After surgical removal of adamantinoma, the patient's condition usually improves after taking Arnica or Hypericum.
Quinine is recommended for postoperative bleeding.
In the presence of an inflammatory process, Mercury solubilis, Nux Vomica, Phosphorus, and Lachesis can help.
As a rule, drugs are prescribed in low dilutions, taking into account that the lower the dilution, the more often the drug is taken.
The preparations are taken before meals, approximately half an hour before. In addition, you cannot brush your teeth or chew gum immediately before and after taking homeopathic remedies.
Prevention
There are no specific methods for preventing adamantinoma, so it is very difficult to prevent the pathology in advance. It is recommended to consult a dentist periodically, at least once every six months, for a preventive examination. You should also visit a doctor at the first signs of oral diseases.
If possible, mechanical damage to bones, bruises, and impacts should be avoided. When installing dentures, it is necessary to select high-quality materials, and the installation itself should be entrusted only to an experienced specialist.
Forecast
The prognosis for adamantinoma is positive in most cases, but only if the neoplasm is detected and removed in a timely manner.
However, it should be taken into account that adamantinoma has a significant tendency to recur, so the patient is subject to medical observation after surgery.


 [
[