Medical expert of the article
New publications
Symptoms and types of astrocytoma of the brain
Last reviewed: 04.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
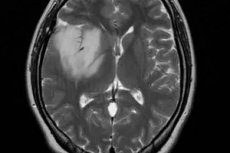
Astrocytoma of the brain is a tumor that is not visible to the naked eye. However, the growth of the tumor does not pass without a trace, because when squeezing nearby tissues and structures, their functioning is disrupted, the tumor destroys healthy tissues, and can affect the blood supply and nutrition of the brain. Such a development of events is typical for any tumor, regardless of its localization.
The growth and pressure of the tumor on the brain vessels provokes an increase in intracranial pressure, which gives symptoms of hypertensive-hydrocephalic syndrome. They may be accompanied by signs of intoxication of the body, which is more typical for the disintegration of malignant tumors in the late stages of cancer. In addition, the tumor has an irritating effect on sensitive neurons in the brain tissue.
All of the above will result in the appearance of a characteristic symptom complex. A person may experience all or individual symptoms:
- persistent headaches, which are most often of a nagging nature,
- symptoms from the digestive system in the form of loss of appetite, nausea, and sometimes vomiting,
- visual impairment (double vision, feeling that everything around is in a fog),
- unexplained weakness and rapid fatigue, characteristic of asthenic syndrome, body aches are possible,
- Often there are disturbances in coordination of movements (the functioning of the vestibular apparatus is impaired).
Some patients develop minor epileptic seizures even before the tumor is detected. Epileptic seizures in astrocytoma are not considered a specific symptom, because they are typical for any brain tumors. However, the reason for the occurrence of seizures without a history of epilepsy is quite understandable. The tumor irritates nerve cells, causing and maintaining the excitation process in them. It is focal abnormal excitation of several neurons that leads to epileptic seizures, often accompanied by convulsions, short-term loss of consciousness, salivation, which the person does not remember after a couple of minutes.
It can be assumed that the larger the tumor, the greater the number of neurons it can excite, and the more severe and pronounced the attack will be.
So far we have talked about brain astrocytoma as such, without focusing on the localization of the tumor. However, the location of the neoplasm also leaves its mark on the clinical picture of the disease. Depending on which part of the brain is affected (pressured) by the tumor, other symptoms appear, which can be considered the first signs of the tumor process of a specific localization. [ 1 ]
For example, the cerebellum is an organ responsible for the coordination of movements, regulation of body balance and muscle tone. It is divided into two hemispheres and a middle part (the vermis, which is considered to be a phylogenetically older formation than the cerebellar hemispheres, which appeared as a result of evolution).
Cerebellar astrocytoma is a tumor that forms in one of the sections of this part of the brain. It is the vermis that does most of the work when it comes to regulating tone, posture, balance, and associated movements that help maintain balance when walking. Cerebellar vermis astrocytoma disrupts the functioning of the organ, hence the prevalence of symptoms such as impaired standing and walking, characteristic of static-locomotor ataxia. [ 2 ], [ 3 ]
Astrocytoma formed in the frontal lobe of the brain is characterized by other symptoms. Moreover, the clinical picture will depend on the damaged side, taking into account which hemisphere of the brain is dominant in a person (left for right-handed people, right for left-handed people). In general, the frontal lobes are the part of the brain that is responsible for conscious actions and decision-making. They are a kind of command post.
In right-handed people, the right frontal lobe is responsible for controlling the execution of non-verbal actions based on the analysis and synthesis of information coming from receptors and other areas of the brain. It does not participate in the formation of speech, abstract thinking, or forecasting of actions. The development of a tumor in this part of the brain threatens the appearance of psychopathic symptoms. This can be either aggression or, conversely, apathy, indifference to the world around them, but in any case, the adequacy of a person's behavior and attitude to what surrounds them can often be questioned. Such people, as a rule, change their character, negative personality changes appear, control over their behavior is lost, which is noticed by others, but not the patient himself.
Localization of the tumor in the precentral gyrus area threatens muscle weakness of varying degrees, ranging from paresis of the limbs, when movements are limited, to paralysis, when movements are simply impossible. A right-sided tumor causes the described symptoms in the left leg or arm, a left-sided tumor in the right limbs.
Astrocytoma of the left frontal lobe (in right-handed people) is in most cases accompanied by speech disorders, logical thinking and memory for words and actions. The motor speech center (Broca's center) is located in this part of the brain. If the tumor presses on it, this is reflected in the characteristics of pronunciation: the rate of speech and articulation are disturbed (speech becomes unclear, blurred with some "clarifications" in the form of individual normally pronounced syllables). With severe damage to Broca's center, motor aphasia develops, which is characterized by difficulties in forming words and sentences. The patient is able to articulate individual sounds, but cannot combine movements to form speech, sometimes pronouncing words other than those he wanted to say. [ 4 ]
When the frontal lobes are affected, perception and thinking are impaired. Most often, such patients are in a state of causeless joy and bliss, called euphoria. Even after learning their diagnosis, they cannot think critically, so they do not realize the full seriousness of the pathology, and sometimes simply deny its existence. They become uninitiative, avoid situations of choice, refuse to make serious decisions. Often, there is a loss of formed skills (like dementia), which causes difficulties in performing familiar operations. New skills are formed with great difficulty. [ 5 ], [ 6 ]
If the astrocytoma is located on the border of the frontal and parietal regions or is displaced towards the back of the head, the usual symptoms are:
- disturbance of body sensitivity,
- forgetting the characteristics of objects without reinforcement by visual images (a person does not recognize an object by touch and does not orientate himself in the location of body parts with his eyes closed),
- failure to perceive complex logical and grammatical constructions concerning spatial relationships.
In addition to the disturbance of spatial sensations, patients may complain of a disturbance of voluntary (conscious) movements in the opposite hand (the inability to perform even habitual movements, for example, bringing a spoon to the mouth).
Left-sided location of parietal astrocytoma is fraught with speech, mental arithmetic, and writing disorders. If the astrocytoma is located at the junction of the occipital and parietal parts, reading disorders are likely due to the fact that the person does not recognize letters, which usually also entails writing disorders (alexia and agraphia). Combined writing, reading, and speech disorders occur when the tumor is located near the temporal part.
Astrocytoma of the thalamus is a pathology that debuts with headaches of a vascular or hypertensive nature and visual disturbances. The thalamus is a deep structure of the brain, consisting mainly of gray matter and represented by two optic tubercles (this explains visual disturbances with a tumor of this localization). This part of the brain acts as an intermediary in the transmission of sensory and motor information between the cerebrum, its cortex and peripheral parts (receptors, sensory organs), regulates the level of consciousness, biological rhythms, sleep and wakefulness processes, and is responsible for concentration.
A third of patients have various sensory disturbances (usually superficial, less often deep, occurring on the side opposite the lesion), half of the patients complain of movement disorders and movement coordination disorders, tremor [ 7 ], slowly progressive Parkinson's syndrome [ 8 ]. People with thalamic astrocytoma (more than 55% of patients) may have varying degrees of higher mental activity disorders (memory, attention, thinking, speech, dementia). Speech disorders occur in 20% of cases and are presented in the form of aphasia and tempo-rhythmic disorders, ataxia. The emotional background may also be disturbed, up to forced crying. In 13% of cases, muscle twitching or slowness of movement is observed. Half of the patients have paresis of one or both hands, and almost all have weakened facial muscles of the lower part of the face, which is especially noticeable during emotional reactions. [ 9 ], [ 10 ], [ 11 ] A case of weight loss in thalamic astrocytoma is described [ 12 ].
Decreased visual acuity is a symptom associated with increased intracranial pressure and is found in more than half of patients with thalamic tumors. When the posterior parts of this structure are affected, visual field narrowing is detected.
With astrocytoma of the temporal region, there is a change in auditory, visual, taste sensations, speech disorders, memory loss, problems with coordination of movements, the development of schizophrenia, psychosis, aggressive behavior [ 13 ]. All these symptoms do not necessarily have to appear in one person, because the tumor can be located higher or lower, bordering on other areas of the brain. In addition, which side of the brain was affected plays a role: left or right.
Thus, astrocytoma of the right temporal lobe is most often accompanied by hallucinations. They can be visual or auditory (visual hallucinations are also typical for damage to the occipital part, which is responsible for processing and perception of visual information), often combined with a disorder of taste perception (with damage to the anterior and lateral parts of the temporal lobe). Most often they occur on the eve of an epileptic seizure in the form of an aura. [ 14 ]
By the way, epileptic seizures with astrocytoma are most likely with tumors of the temporal, frontal and parietal lobes. In this case, they manifest themselves in all sorts of diversity: convulsions and head turns while maintaining or losing consciousness, freezing, lack of reaction to the environment in combination with repetitive movements of the lips or reproduction of sounds. In mild forms, there is an increase in heartbeat, nausea, skin sensitivity disorders in the form of tingling and "goosebumps", visual hallucinations in the form of a change in color, size or shape of an object, the appearance of flashes of light before the eyes.
When the hippocampus, located on the inner surface of the temporal region, is damaged, long-term memory suffers. Localization of the tumor on the left (in right-handed people) can affect verbal memory (the person recognizes objects, but cannot remember their names). Both oral and written speech suffer, which the person stops understanding. It is clear that the patient's own speech is a construction of unrelated words and sound combinations. [ 15 ]
Damage to the right temporal region negatively affects visual memory, recognition of intonation, previously familiar sounds and melodies, and facial expressions. Auditory hallucinations are characteristic of damage to the upper temporal lobes.
If we talk about persistent symptoms of astrocytoma, which occur regardless of the location of the tumor, then first of all it is necessary to note headache, which can be either constant aching (this indicates the progressive nature of the tumor), or occur in the form of attacks when changing body position (typical for early stages).
This symptom cannot be called specific, but observations show that a brain tumor can be suspected if the pain appears in the morning and weakens by the evening. With high blood pressure, headaches are usually accompanied by nausea, but if intracranial pressure increases (and this can be caused by a growing tumor that compresses blood vessels and disrupts the outflow of fluid from the brain), vomiting, frequent hiccups, and deterioration of thinking abilities, memory, and attention may also occur.
Another feature of headaches with astrocytoma of the brain is its widespread nature. The patient cannot clearly determine the localization of pain, it seems that the whole head hurts. As intracranial pressure increases, vision also deteriorates up to complete blindness. Most quickly, cerebral edema with all the ensuing consequences occurs with tumor processes in the frontal lobes.
Astrocytoma of the spine
So far we have talked about astrocytoma as one of the glial tumors of the brain. But the nervous tissue is not limited to the cranium, through the occipital foramen it penetrates into the spine. The continuation of the initial section of the brainstem (medulla oblongata) is a nerve fiber that extends inside the spinal column to the tailbone. This is the spinal cord, which also consists of neurons and connecting glial cells.
Spinal cord astrocytes are similar to those in the brain, and they, too, under the influence of some (not fully understood) reasons, can begin to divide intensively, forming a tumor. The same factors that can provoke tumors from glial cells in the brain are considered as possible causes of spinal cord astrocytoma.
But if brain tumors are characterized by increased intracranial pressure and headaches, then spinal cord astrocytoma may not manifest itself for a long time. The progression of the disease in the overwhelming majority of cases is slow. The first signs in the form of spinal pain do not always appear, but often (about 80%), and only 15% of patients experience a combined occurrence of back and head pain. Skin sensitivity disorders (paresthesia) also occur with the same frequency, which manifest themselves as spontaneous tingling, burning, or a sensation of crawling ants, and pelvic disorders due to a violation of their innervation. [ 16 ]
Symptoms of motor disorders, diagnosed as paresis and paralysis (weakening of muscle strength or inability to move a limb), appear at later stages, when the tumor becomes large and disrupts the conductivity of nerve fibers. Usually, the interval between the onset of back pain and motor disorders is at least 1 month. At later stages, some children also develop spinal column deformities. [ 17 ]
As for the localization of tumors, the majority of astrocytomas are found in the cervical region, less often they are localized in the thoracic and lumbar regions.
Spinal cord tumors can occur in early or late childhood, as well as in adult patients. However, their prevalence is lower than that of brain tumors (only about 3% of the total number of diagnosed astrocytomas and about 7-8% of all CNS tumors). [ 18 ]
In children, spinal cord astrocytomas occur more often than other tumors (about 83% of the total number); in adults, they are second only to ependymomas (a tumor of the ependymal cells of the ventricular system of the brain - ependymocytes). [ 19 ]
Types and degrees
A tumor of astrocytes is one of many variants of the tumor process in the central nervous system, and the concept of "brain astrocytoma" is very general. Firstly, neoplasms can have different localizations, which explains the dissimilarity of the clinical picture in the same pathology. Depending on the location of the tumor, the approach to its treatment may also differ.
Secondly, the tumors differ morphologically, i.e. they consist of different cells. Astrocytes of the white and gray matter have external differences, for example, the length of the processes, their number and location. Fibrous astrocytes with weakly branching processes are found in the white matter of the brain. Tumors of such cells are called fibrous astrocytomas. Protoplasmic astroglia of the gray matter are characterized by strong branching with the formation of a large number of glial membranes (the tumor is called protoplasmic astrocytoma). Some tumors can contain both fibrous and protoplasmic astrocytes (fibrillary protoplasmic astrocytoma). [ 20 ]
Thirdly, neoplasms from glial cells behave differently. The histological picture of different variants of astrocytoma shows that among them there are both benign (they are a minority) and malignant (60% of cases). Some of the tumors develop into cancer only in isolated cases, but they can no longer be classified as benign neoplasms.
There are various classifications of brain astrocytomas. Some of them are understandable only to people with medical education. For example, let's consider a classification based on the difference in cell structure, which distinguishes 2 groups of tumors:
- Group 1 (common or diffuse tumors), represented by 3 histological types of neoplasms:
- fibrillary astrocytoma - a formation without clear boundaries with slow growth, refers to the diffuse variant of astrocytomas, consisting of astrocytes of the white matter of the brain
- protoplasmic astrocytoma - a rare type of tumor that often affects the cerebral cortex; it consists of small astrocytes with a small number of glial fibers, it is characterized by degenerative processes, the formation of microcysts inside the tumor [ 21 ]
- gemistocytic or gemistocytic (mast cell) astrocytoma - poorly differentiated accumulation of astrocytes, consists of large angular cells
- Group 2 (special, distinct, nodal), represented by 3 types:
- pilocytic (hair-like, hair-like, piloid) astrocytoma - a non-malignant tumor of parallel fiber bundles, has clearly defined boundaries, is characterized by slow growth, and often contains cysts (cystic astrocytoma) [ 22 ]
- subependymal (granular) giant cell astrocytoma, subependymoma - a benign tumor, named so because of the giant size of its constituent cells and location, often settles near the membranes of the ventricles of the brain, can cause blockage of the interventricular openings and hydrocephalus [ 23 ]
- Microcystic cerebellar astrocytoma is a nodular formation with small cysts that is not prone to degeneration into cancer.
It should be noted that epileptic seizures are more characteristic of the second group of brain astrocytomas.
This classification gives an idea of the tumor structure, which is not very clear to the average person, but does not answer the burning question of how dangerous are different forms of diffuse tumors. With nodular tumors, everything is clear, they are not prone to degeneration into cancer, but are diagnosed much less often than diffuse ones.
Later, scientists made repeated attempts to classify astrocytomas by their degree of malignancy. The most accessible and convenient classification was developed by the WHO, taking into account the tendency of different types of astrocytomas to degenerate into a cancerous tumor.
This classification considers 4 types of glial tumors from astrocytes, which correspond to 4 degrees of malignancy:
- Group 1 of neoplasms - astrocytomas of the 1st degree of malignancy (grade 1). This group includes all types of special (benign) astrocytomas: pilocytic, subependymal, microcystic, pleomorphic xanthoastrocytoma, usually developing in childhood and adolescence.
- Group 2 of neoplasms – astrocytomas of 2 (low) degree of malignancy (grade 2 or low grade). This includes the usual (diffuse) astrocytomas discussed above. Such neoplasms can develop into cancer, but this happens rarely (usually with a genetic predisposition). They are more common in young people, since the age of detection of a fibrillary tumor rarely exceeds 30 years.
Next come tumors with a high degree of malignancy, which are prone to cell malignancy (high grade).
- Group 3 tumors – astrocytoma of the 3rd degree of malignancy (grade 3). A striking representative of this group of tumors is considered to be anaplastic astrocytoma – a rapidly growing neoplasm without defined contours, more often found among the male population aged 30-50.
- Group 4 glial tumors from astrocytes are the most malignant, highly aggressive neoplasms (grade 4) with almost lightning-fast growth, affecting the entire brain tissue, and the presence of necrotic foci is mandatory. A striking example is multiform glioblastoma (giant cell glioblastoma and gliosarcoma), diagnosed in men over 40 years of age and practically incurable due to an almost 100% tendency to relapse. Cases of the disease in women or at a younger age are possible, but occur less frequently.
Glioblastomas do not have a hereditary predisposition. Their occurrence is associated with highly oncogenic viruses (cytomegalovirus, herpes virus type 6, polyomavirus 40), alcohol consumption and exposure to ionizing radiation, although the effect of the latter has not been proven.
Later, new versions of the classification included new variants of already known types of astrocytoma, which nevertheless differ in the probability of degeneration into cancer. Thus, piloid astrocytoma is considered one of the safest benign types of brain tumors, and its variant, pilomyxoid astrocytoma, is a rather aggressive neoplasm with rapid growth, a tendency to relapse, and the possibility of metastasis. [ 24 ]
Pilomyxoid tumor has some similarities with piloid tumor in location (most often it is the area of the hypothalamus and optic chiasm) and the structure of its constituent cells, but it also has many differences, which allowed it to be distinguished as a separate type. The disease is diagnosed in young children (the average age of patients is 10-11 months). The tumor is assigned the 2nd degree of malignancy.

