Medical expert of the article
New publications
Enlargement of lymph nodes of the lung roots and mediastinum
Last reviewed: 04.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
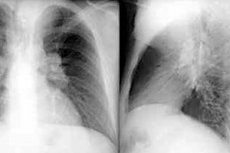
Among the general symptoms of a fairly wide range of diseases, an increase in lymph nodes in the lungs is noted - pulmonary, hilar bronchopulmonary, peribronchial or paratracheal. Since the lymph nodes are an integral part of the body's immune system, their increase, detected by radiography, CT or MRI of the lungs, is one of the clinical signs of pathologies of infectious or oncological origin.
Enlarged lymph nodes can be called lymphadenopathy, hyperplasia, and even enlarged lymph node syndrome (in AIDS patients), but in any case, the pathology has the same code R59 in accordance with ICD-10, and subclass R includes symptoms and abnormalities that are detected in patients during a medical examination.
Epidemiology
To date, there are no exact statistics on cases of enlarged lymph nodes in the lungs, as well as lymphadenopathy in other locations. However, according to experts from the British Paediatric Association, the increase in palpable nodes (behind the ear, submandibular, cervical, etc.) in childhood associated with infections varies from 38-45%, and this is one of the most common clinical problems in pediatrics.
According to the American Society of Clinical Oncology, the degree of malignant enlargement of lymph nodes correlates with age, increasing from 17.5-20% in 18-35 year old patients to 60% among older patients. And in children, this is most often a consequence of leukemia, and in adolescents - Hodgkin's lymphoma.
Benign reactive lymphadenopathy accounts for an average of 30% of cases, while enlarged lymph nodes in non-neoplastic diseases account for 26%.
Causes lymph node enlargement in the lungs
The enlargement of localized in the lungs (intrapulmonary) nodes occurs in response to the main pathological process of the disease – thanks to their T and B lymphocytes, macrophages, dendrites, lymphatic follicles and other protective factors of the lymphoid tissue.
The main diseases associated with the causes of enlarged lymph nodes in the lungs include:
- pneumonia caused by staphylococci and beta-hemolytic streptococci, as well as pneumococcal pneumonia;
- pulmonary tuberculosis (caused by Mycobacterium tuberculosis);
- tuberculosis of the lymph nodes (in pulmonary and extrapulmonary forms of tuberculosis);
- pulmonary sarcoidosis;
- fibrotic pulmonary lesions in systemic lupus erythematosus or amyloidosis;
- acute or chronic forms of bronchopulmonary mycoses caused by airborne infection of the respiratory organs by the fungi Histoplasma capsulatum (histoplasmosis), the mold fungus Aspergillus fumigatus (aspergillosis), the yeast-like fungus Blastomyces dermatitidis (pulmonary blastomycosis);
- exogenous allergic alveolitis (allergic pneumonitis);
- chronic occupational pulmonary diseases – silicosis and pneumoconiosis;
- lymph node cancer – lymphogranulomatosis (Hodgkin's lymphoma), non-Hodgkin's lymphoma (lymphosarcoma);
- lung cancer (adenocarcinoma, carciosarcoma, paraganglioma, etc.);
- acute lymphoblastic leukemia (a form of leukemia associated with malignant damage to the hematopoietic cells of the bone marrow);
- metastases to the pulmonary lymph nodes from malignant tumors of the esophagus, mediastinum, thyroid gland, or mammary gland. See also - Metastases to the lymph nodes
Pulmonologists note that enlarged lymph nodes in the root of the lung are characteristic of many pathologies, since here - in the zone of demarcation of the middle and posterior mediastinum of the chest - are located not only the bronchopulmonary and paratracheal lymph nodes, but also the longest lymphatic duct (thoracic). Root nodes can be enlarged in pneumonia, tuberculous bronchoadenitis, sarcoidosis, allergic alveolitis, bronchioloalveolar tumor of the lung, metastases of breast cancer, etc. Read also the publication - Causes of enlarged lymph nodes
As you understand, the presence of the listed diseases is the main risk factor for enlarged lymph nodes, which is included in the list of their symptoms.
Pathogenesis
The mechanisms of occurrence and development – pathogenesis of enlarged lymph node – are partially determined by the functions of lymph nodes, which, with the help of macrophages of their sinuses and stroma, cleanse the lymphatic fluid from infection-associated antigens, toxins and products of cellular metabolism. For more details, see the article Hyperplasia of lymph nodes.
Depending on the cause of the disease and the mechanism of action on the lymphoid tissue, there are different types of this pathology: infectious, reactive and malignant. Thus, during an infection, phagocytes with captured antigens and cells that have died from inflammatory necrosis enter the nodes with the lymph flow and accumulate. For example, in tuberculosis patients, mycobacteria M. tuberculosis that have entered the lymph nodes are absorbed by macrophages with the formation of phagolysosomes, the formation of granulomas and the development of caseous necrosis of the lymphoid tissue.
Granulomatous changes in the lymph nodes (with displacement of lymphoid tissue by fibrous tissue) are also observed in sarcoidosis, the etiology of which is still unknown to medicine (although autoimmune and genetic causes of its occurrence are not excluded).
In cases of reactive enlargement of the lymph nodes in the lungs, the dominant pathological process is the increased proliferation of their follicles, which is provoked by autoimmune diseases - when the body's immune system produces antigens against healthy cells, as occurs, in particular, in systemic lupus erythematosus.
When lymph nodes in the lungs increase in a malignant nature, lymphomas with abnormal cell proliferation are formed. And in metastases, lymphoproliferative disorders are caused by the infiltration of healthy tissues by atypical (cancerous) cells and their proliferation, which leads to pathological morphological changes.
 [ 14 ]
[ 14 ]
Symptoms lymph node enlargement in the lungs
As clinicians emphasize, an increase in lymph nodes in the lungs is a consequence of the development of diseases, and information regarding the size of intrapulmonary lymph nodes (diameter > 2 cm) can only be obtained by visualizing them.
So the symptoms of enlarged lymph nodes in the lungs are not distinguished from the clinical picture of the underlying diseases. Although when examining the lymph nodes in the lungs, not only their size, location and quantity are recorded, but also the presence of an inflammatory process, granuloma, necrosis (caseous or in the form of an abscess), pulmonary infiltrates, etc.
A tumor of an intrapulmonary lymph node can cause swelling of adjacent tissues or obstruction of lymphatic vessels, which leads to the appearance of respiratory symptoms: persistent dry cough, stridor (wheezing), shortness of breath.
Symptoms of calcified lymph nodes, such as those seen in histoplasmosis or tuberculosis, may also include coughing when the enlarged node protrudes into the trachea.
And large granulomatous hypertrophied lymph nodes can be accompanied not only by breathing problems, but also by painful sensations.
Complications and consequences
In most cases, the consequences and complications are related to the course of the underlying disease. And complications of enlarged lymph nodes in the lungs include the formation of an abscess or phlegmon, the formation of fistulas, and the development of septicemia.
Enlargement of the lymph nodes in the mediastinal region can lead to bronchial or tracheal obstruction, esophageal stricture, and impaired blood flow in the superior vena cava.
Pulmonary infiltrate in the lymph nodes of sarcoidosis can lead to scarring and irreversible pulmonary fibrosis, severe pulmonary dysfunction, and heart failure.
In case of tuberculous lesions of the intrathoracic lymph nodes with caseous contents, their rupture and infection can spread to other structures of the mediastinum are possible.
With malignant enlargement of intrapulmonary lymph nodes, metabolic complications arise: increased levels of uric acid in the blood, electrolyte imbalance, and functional renal failure.
Diagnostics lymph node enlargement in the lungs
Diagnosis of enlarged lymph nodes in the lungs is, first of all, instrumental diagnostics using radiography, ultrasound, computed tomography (CT), magnetic resonance imaging (MRI), positron emission tomography (PET).
Based on the results, a biopsy of the hyperplastic node (endoscopic, bronchoscopic or excisional) and immunohistochemical examination of the obtained tissue sample may be required. The biopsy results are especially important if there is a suspicion of a malignant tumor of the lymph node, and there are serious doubts about the diagnosis of the disease in which the pathological change in the lymph node was detected. Blood tests are also necessary: general and biochemical, for antibodies, for immune status and tumor markers. Skin tests are done for tuberculosis and sarcoidosis.
What do need to examine?
How to examine?
Differential diagnosis
Differential diagnosis based on the results of histology of the biopsy is necessary to determine the benign (or malignant) nature of lymph node hyperplasia – in order to establish the correct diagnosis.
Who to contact?
Treatment lymph node enlargement in the lungs
Considering that hyperplastic intrapulmonary lymph nodes appear in various pathologies, the main therapeutic efforts are aimed at these diseases, and separate treatment of enlarged lymph nodes in the lungs is simply impossible.
When the underlying cause is a bacterial infection, antibiotics are used; in bronchopulmonary mycoses, doctors prescribe systemic antifungal drugs. To reduce inflammation, drugs from the steroid hormone group (corticosteroids) or NSAIDs (non-steroidal anti-inflammatory drugs) can be used. In all cases, it is recommended to take vitamins A and E.
And when enlarged lymph nodes cause tissue degeneration and abscess formation, surgery may be required.
In cases of malignant enlargement of the lymph nodes in the lungs, treatment may include radiation, drug therapy with chemotherapy drugs, and surgery - anatomical segmentectomy or resection of the entire node (lymphadenectomy).
Prevention
Enlargement of the lymph nodes in the lungs is a common clinical manifestation and diagnostic sign, and its prevention, that is, a set of specific measures, has not been developed. Doctors advise to promptly seek medical help in case of prolonged deterioration of health, which can prevent the development of serious diseases.

