Medical expert of the article
New publications
What do vascular asterisks look like on the face, body and legs?
Last reviewed: 04.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
It is accepted that a person is adorned with clear skin without any flaws. It is unlikely that a cute mole on the cheek can spoil the aesthetic appearance. But scars, large birthmarks, acne, pockmarks, telangiectasias have never been considered attractive. Among all of the above, of particular interest are anomalies called by an unusual word - telangiectasias. This is the name of vascular defects or reddish stars, nets, branches, dots of small vessels that can appear in both sick and healthy people. Many know from their own experience what spider veins look like on the body, but have no idea how to deal with this scourge. And others do not even know what we are talking about. But forewarned is forearmed, so we will try to give useful information to both.
A little bit about spider veins
Vascular asterisks, capillary networks or spiders are neoplasms consisting of dilated small-caliber vessels. These include:
- Capillaries are tiny vessels with a diameter of about 5-10 microns, in which the exchange of gases (oxygen and carbon dioxide) and the replacement of arterial blood with venous blood occur.
- Venules are small vessels with a diameter of 12-28 microns, which are a continuation of the capillaries and ensure the outflow of venous blood with a large amount of carbon dioxide from them.
- Arterioles are small blood vessels that supply arterial, oxygen-rich blood to the capillaries. In the vascular networks, they are usually represented by their terminal segments, i.e. those areas that are adjacent to the capillaries and have the smallest diameter.
Most often, the walls of venules and capillaries are subject to stretching. Arterial vessels have an elastic and durable three-layer membrane, designed for high pressure of blood coming from the heart. Only a disorder of the trophic function and metabolism can disrupt the properties of the elastic muscular membrane. Venules, which provide blood flow to the heart under lower pressure, are not designed for heavy loads. Their walls are less durable and elastic, easily stretched and unable to fully restore their shape.
Capillaries, whose walls are permeable and consist of only one layer, change their shape quite easily under excessive loads and compression. At high blood pressure, they are prone to ruptures and hemorrhages. [ 1 ]
The change in the shape of the vessel can be both local and extensive. But with the naked eye we see only the areas of expansion that are closer to the surface of the skin. As the vessel wall expands, it becomes thinner and the contents of the vessels, i.e. blood, are visible through it.
Our body and skin are permeated with many intertwined small vessels. If there is only one dilated area in the superficial layers of the skin, we can see a point or stripe of a darker color than the surrounding skin. Depending on how close it is to the epidermis, its color will also change (from brownish to brown, red or purple).
If the elasticity of the walls of several small vessels is impaired in a local area, we see a vascular network resembling a spider in different shades of red.
The appearance of spider veins depends not only on the number and location of the affected vessels, but also on their type. In arterial vessels, the blood is scarlet, and such telangiectasias will be red. In venules, the blood is the darkest, so neoplasms from them will be dark red, burgundy and purple. Capillaries are very thin vessels, so regardless of the composition of the blood in them and its oxygen saturation, expansions are visible as red defects with a slight variation in shades.
Despite the beautiful popular name, vascular anomalies are not considered welcome guests on the skin. And not only because of their unaesthetic appearance. These unusual anomalies have an ambiguous origin and it is very difficult, and sometimes impossible, to determine the reason for their appearance.
In some cases, spider veins can be considered a symptom of a disease. The appearance of venous nodules and spider veins associated with impaired microcirculation in the veins and impaired tissue trophism is observed with varicose veins. In acute and chronic liver diseases (cirrhosis, hepatitis), the appearance of vascular anomalies resembling spiders in shape is associated with impaired functioning of the organ and hormonal disorders. The fact is that in addition to removing toxins, the liver has other responsibilities. So, it actively participates in the metabolism of many hormones, including estrogen. The liver removes excess vasoactive substances (adrenaline, bradykinin, etc.) from the body, causing vasodilation.
Disruption of metabolic processes of female and male hormones (estrogens and testosterone), as well as hormonal substances that affect blood vessels, is precisely the reason for the appearance of vascular networks in liver diseases.
If we are talking about chronic diseases, vascular elements will be present on the body constantly. And those defects that are associated with temporary disorders (hormonal disruptions in acute liver pathologies) usually disappear after health is normalized. [ 2 ]
Due to hormonal imbalance, vascular formations can occur during pregnancy and menopause. Their appearance is also facilitated by the use of hormonal contraceptives. Non-hormonal causes of temporary red spots and meshes on the body are considered to be skin injuries. If the cause of telangiectasias can be eradicated and tissue trophism is not impaired, the neoplasms usually disappear on their own.
Symptoms vascular asterisks
We have already said that the appearance of spider veins can have different causes. Some of them are pathological. And since the eye can only determine the nature of the vessel, but not the reason for its expansion, the appearance of telangiectasias should be considered as a signal of possible ill health.
Spider veins are often the first signs of liver disease, occurring in an acute form. This organ is poorly supplied with nerve fibers, so pain in it is not always felt and not immediately (usually at the stage of cancer, with an abscess or syphilitic lesion). Liver diseases are most often judged by their external manifestations: the appearance of spider veins, yellowing of the skin and palms, changes in the color of urine and feces. [ 3 ]
In chronic cardiovascular and liver diseases, neoplasms from small vessels are constantly present, but the severity of the anomaly depends on the period of the disease (exacerbation or remission) and the duration of its course.
Telangiectasias can have different shapes and sizes:
- Linear form. New growths in the form of stripes from red to purple shade depending on the type of vessels. Most often, spider veins with localization on the legs, distinguished by darker shades, have this form. These are dilated areas of small veins.
- Point vascular asterisks are also the result of a local lesion (expansion or rupture of the wall with point hemorrhage) of one small vessel: a capillary, vein or arteriole. The color of the neoplasm depends on the type of vessel and the duration of its damage.
- Vascular spiders. They have a red nodule in the center, rising above the skin surface and formed as a result of a rupture of the wall of one or several closely located vessels. From which thin capillary rays extend in different directions. They are usually light red in various shades.
- Vascular trees. In this case, the subcutaneous pattern resembles a tree branch with multiple thin branches. Its color depends on the type of vessels.
- Capillary mesh. A type of spider veins made from interlacing dilated capillaries without damaging their walls.
Taking into account how spider veins look, what color they are and where they are located, you can suspect specific diseases. The accuracy of such diagnostics is, of course, not high, but it allows you to think about your health and visit a doctor once again.
Couperose
Cosmetologists call couperose an anomaly of small vessels localized in the facial area, where they become visible to the naked eye. In this case, it is not the appearance of the spider veins (shape, color, size) that is taken into account, but their localization. In dermatology, spider veins, wherever they appear, are called telangiectasias.
Spider veins on the face and neck are especially common in people with thin, sensitive skin, especially if it is exposed to aggressive environmental factors (active sun, wind, frost). Many people, coming home from the cold, notice tree-like spider veins on their cheeks.
Facial skin is usually more delicate than most of the rest of the human body, and it is also more exposed to negative external influences than other areas. You can protect yourself from negative factors of the outside world only with the help of special creams. But even their use does not always help to avoid the appearance of unwanted "decorations". Fortunately, such neoplasms disappear quite quickly when the body adapts to the surrounding temperature.
The skin on our face around the eyes is especially thin. It is easily injured, and any minor injury can lead to the appearance of a vascular network under the eyes or on the eyelids. Women have more delicate skin, the beauty of which they maintain with various cosmetics. Some of these products can cause allergies, in which an increased amount of histamine is released into the blood - a hormone-like substance that can dilate blood vessels. This causes lacrimation, allergic rhinitis, local dilation of blood vessels and hyperemic areas with visible capillary network.
Spider veins on the eyelids can appear as a result of eyelid trauma when rubbing the eyes or applying cosmetics (eyeliner, mascara), an allergic reaction or exposure to aggressive environmental factors.
Vascular asterisks on the lips are most often the result of trauma or infection. They can appear near herpetic eruptions, in the corners of the lips with angular cheilitis. Telangiectasias above the upper lip are often the result of the removal of the antennae. Pulling out the hair follicle can be accompanied by a rupture of the capillaries that feed it. Disruption of microcirculation at the site of the rupture leads to the formation of red dots and small capillary spiders. [ 4 ]
Telangiectasias in the forehead, cheeks and chin are often the consequences of fighting acne. At the site of the squeezed pimple, as a result of pressure on small vessels located in the upper and deeper layers of the skin, as well as rupture of their membranes, red dots, irregular spots, linear and branched patterns of different shades of red remain. In this case, not only mechanical but also chemical effects (allergy to creams and lotions, use of alcohol-containing compounds for disinfection and cauterization) can lead to vasodilation.
Spider veins on the nose can appear both under the influence of negative environmental factors and after mechanical damage to the vessels. The latter is possible not only when removing pimples in various ways, but also as a result of a runny nose (as a result of constant friction of the fingers against the skin of the wings of the nose, the latter turn red and red veins appear on them).
Spider veins on arms and legs
The thickness of the skin on different parts of the body varies from person to person. If you compare the hands of different people of the same sex, you can see that some have a clearly visible vascular pattern (those with thin skin and a small fat layer), while others seem to have none at all. Under the influence of cold, wind, solar radiation, and thermal factors, such pictures of red trees can become brighter, which is a normal reaction of the vessels.
The vessels on the arms also swell when carrying heavy objects, straining the arms, or squeezing the limb. In this case, even large vessels are usually visible, and small spider-like formations appear only in places where capillaries are broken. That is, how spider veins on the limbs look depends on the processes occurring at the site of their appearance. This applies to both cancer and legs.
Spider veins on the hands can appear both on their upper part (usually on the forearm and wrist) and in the area of the hand (its back and palms). And this is exactly the point that is worth dwelling on in more detail. The appearance of persistent redness of the palms and vascular pattern on them is considered one of the signs of various liver diseases, accompanied by dysfunction of the organ. "Liver" palms can be seen in patients with cirrhosis of the liver, hepatitis, abscess and liver cancer.
Telangiectasias on the back of the hand usually occur as a result of trauma (mechanical, thermal or chemical), causing local vasodilation or disruption of blood microcirculation. They are also possible in the palms, but in this case there is no symmetry (in liver diseases, both palms turn red, the pattern of vessels appears in approximately the same places on both hands).
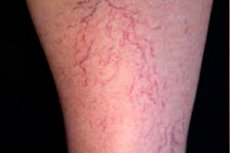
Spider veins appear even more frequently on the legs (usually on the thighs and shins, and in rare cases on the feet). The skin on the feet is usually rougher and thicker, so the vessels are not visible through it. Vessels dilated as a result of a blow, injury or thermal burn can only be seen in those who carefully look after the skin of their legs, regularly exfoliating and removing hardened skin. However, sometimes unprofessionally done exfoliation is precisely what causes skin injury and the reaction of the vessels to it. [ 5 ]
Spider veins on the thighs and shins often appear in those whose work requires them to stand for a long time, as well as those with sedentary jobs. In the latter case, the risk of getting such a "decoration" is higher for those who like to sit with their legs crossed, because it is in this position of the limbs that blood circulation in the vessels is disrupted, the pressure in them increases, which causes an increase in diameter.
Regular disruption of venous outflow due to microcirculation and metabolic disorders eventually leads to the development of vascular pathologies, the most common of which is varicose veins. With this pathology, persistent swelling of the veins appears on the shins and thighs with the appearance of nodules on the skin and a linear or branched dark red with a bluish tint pattern.
If the appearance of vascular images is caused by overexertion of the legs, carrying heavy objects, walking in high heels, they soon disappear, as soon as the legs rest. But if such violence is repeated regularly, after some time the venules lose their ability to recover, they stretch (more in length), and bend under the skin, which is why they become clearly visible against the skin.
Spider veins on the thighs sometimes have different shapes, sizes and shades. A similar picture is often observed with excess weight and obesity, when the risk of varicose veins increases. In overweight people, not only venous but also arterial vessels experience increased stress, so telangiectasias can have a different shade. The fat layer does not interfere with contemplating the pattern, because we see only those vessels that are closely adjacent to the outer layer of the skin (epidermis), and the subcutaneous tissue is located much lower.
Telangiectasias may appear on the thighs of women suffering from cellulite. In this case, they can also be expected in other places covered with "orange peel" (on the buttocks, fat deposits in the abdominal area, upper arms, etc.).
Spider veins on the body
We have already said that telangiectasias can appear on different parts of the human body. And even on those that are usually covered by clothing and rarely injured. They can occur anywhere where there is a violation of blood microcirculation or stretching of blood vessels, appear with thermal exposure to the skin or injuries, in places where metabolic processes are disrupted.
The appearance of spider veins on the chest and shoulders, as the most unprotected parts of the body, is usually seasonal. They are most visible in people with fair skin under the influence of the sun. Their tan is almost a continuous capillary network, the result of a slight skin burn. It is clear that few people take such an event seriously or with concern. And even more severe burns, when a bright capillary network reminds of itself for several days, rarely stop those who want to have tanned skin. And this is despite the fact that almost all media say that solar radiation is one of the important factors in the development of skin cancer. [ 6 ]
But the appearance of individual "spiders" near the mammary glands should definitely not be treated carelessly. At the same time, the fact of how the vascular stars look is of decisive importance. The vascular network can be seen on full breasts, during feeding the child, when the skin and vessels under it are stretched. But the appearance of local small spider-shaped telangiectasias on the skin should be alarming. It is precisely such long-lasting defects that should be alarming, because if there was no injury, then what else could have caused the disruption of blood flow and vasodilation?
However, during pregnancy, menopause, after abortions, when vascular changes are caused by hormonal changes, and also as a result of using hormonal contraceptives, spider veins can appear on different parts of the body without indicating any pathology.
Spider veins on the upper body can appear in both women and men with fair skin. The latter like to walk around with an open torso in sunny weather, and at the site of sunburn you can see redness with a visible vascular network.
Spider veins on the back can be the result of sunburn or squeezing acne in the appropriate location, or a symptom of liver dysfunction. With dysfunction of this organ and bile ducts, a rash of small spider veins is often observed in the face and back. The skin on the back is not particularly delicate, so telangiectasias do not appear here without reason.
The same can be said about spider veins on the abdomen. In liver pathologies, they can be quite large and branched, the color of the translucent vessels is bluish. A similar picture is observed in case of venous outflow disturbance as a result of decreased ability and speed of blood flow through the diseased liver in such pathologies as liver cancer or cirrhosis. Hepatic spider veins of this localization are compared to the head of a jellyfish, since they cover the swollen abdomen of the patient, creating the impression that it, like the cap of a jellyfish, is translucent through and through.
The appearance of small stars, linear or sinuous stripes, red dots on the stomach, sides and buttocks can be a sign of cellulite or compression of blood vessels in the waist and pelvic area by a belt, elastic band, rough seams on clothing. In the second case, telangiectasias quickly disappear if the cause that causes them is removed.
Spider veins in the genital and perineal areas indicate a disruption of venous blood flow in the pelvic area, which may be the result of sedentary work or wearing underwear that is too tight with rough seams. [ 7 ]
Telangiectasia during pregnancy
Not only special medications used in cardiology (vasodilators), but also some biologically active substances have the ability to dilate blood vessels. It is this property of histamine and other hormone-like substances that underlies the action of many such drugs. The fact that the level of production of some vasoactive hormones increases during pregnancy explains the high frequency of spider veins in expectant mothers.
Female and male sex hormones can cause an increase in the lumen of small vessels. When they are normal, there is nothing to be afraid of. But in women, the level of estrogen jumps during pregnancy, because it is necessary for the normal development of the placenta and the fetus in it. This is an elementary explanation for the appearance of telangiectasias in pregnant women.
Regardless of how spider veins look during pregnancy, the reason for their appearance during hormonal changes is the same for all women. Or rather, it is a stable complex of non-pathological reasons. Changes in hormone levels, weight gain, and therefore stress on the legs and heart, stretching of tissues in the abdominal area with each month of pregnancy.
On the abdomen, the increased visibility of blood vessels can be explained by the stretching of the skin on it as the child grows (stretched skin is thinner and more transparent). At the same time, the veins are also stretched (mainly in length) due to their plasticity.
Temporary spider veins on the legs may appear after long walks due to the increased load on the legs. But a forced or unjustified sedentary lifestyle of the expectant mother can cause venous congestion in the pelvic area, and telangiectasias will become chronic.
If the body of the expectant mother does not have metabolic disorders that change the properties of muscle and connective tissue, then after childbirth the abdomen is restored and as this happens, the vascular asterisks disappear. But even if they do not disappear for a long time, the cause is not necessarily pathological.
A possible reason is the use of hormonal contraceptives, the action of which is based on the correction of hormonal levels. And although we are no longer talking about high levels of estrogen, it is important to understand that any fluctuations in hormonal levels will affect the condition of the body and, in particular, the characteristics of the vascular walls. For example, during menopause, women's estrogen levels are significantly reduced, but the risk of spider veins increases (and not only due to varicose veins). The fact is that natural estrogens not only correlate with the diameter of blood vessels, but also help improve the elasticity of their walls. With a decrease in estrogen levels, blood vessels become flabby, stretch easily and are worse at restoring their shape, which is what we observe during menopause. [ 8 ]
But why do some pregnant women have visible vascular defects, while others do not? Again, it's all about the properties of the skin (some people have thin and delicate skin, so even small vessels are visible through it) and hereditary predisposition. The restructuring of the expectant mother's body acts as a trigger for a genetically determined process.
Spider veins in a child
A child's body, as is known, has many differences from an adult's. A newborn baby spent a long time in the mother's womb, and the conditions of its existence did not require the organization of a serious system of protection and adaptation. The newborn's body is little reminiscent of a protective shell. Thin, easily vulnerable and very sensitive to changes in the environment, it seems to glow through and through.
Very often, a bluish pattern of small veins in the eyelids, forehead and cheeks is visible in small children, whose skin is more delicate than that of adults. Such patterns are especially visible after walks in the fresh air on sunny, windy or frosty days.
The tendency to develop vascular patterns is most pronounced in premature, weakened and sickly children, who already have a decent list of various pathologies of internal organs at birth. But even in healthy children born on time, you can see the vascular pattern shining through the thin skin of the face.
Spider veins on the face of a newborn are a common occurrence. Pediatricians are calm about it, recommending only to protect the child's face from the sun and wind, so as not to complicate the situation. With age, the vessels become less noticeable.
If telangiectasias appeared at a later age, it is necessary to pay attention to the preceding events and behavior of neoplasms. The appearance of single vascular networks can be the result of an accidental skin injury. If a "tree" appeared on the cheeks or forehead of a child, the cause may be a temperature drop when leaving the bath or overheating of the child. The appearance of a pattern after walks is completely normal.
If spider veins disappear quickly, there is nothing to worry about. But those that persist for a long time are worth paying attention to. They can be the result of a genetic predisposition (especially if the parents also had a similar reaction of the vascular system), which can manifest itself at different ages, or indicate some health problems. You should not, referring to the young age, exclude liver disease and circulatory disorders in a child. [ 9 ]
The same liver cirrhosis has a genetic predisposition, so it kills not only those who abuse alcohol (sometimes diagnosed in boys over 7 years old). Hepatitis affects people of different ages, but in chronic cases in children it often develops into liver cirrhosis. In addition, in some cases (even if they are extremely rare), the appearance of a vascular network may indicate the development of malignant processes in the body.
What do spider veins look like in a child? Usually, these are not point formations. More common are dendritic telangiectasias, which are visible constantly from birth or appear later, becoming more pronounced when the skin is exposed to heat or cold.
The appearance of multiple spider-like, point and linear vascular anomalies requires examination of the child, because here there is a persistent violation of blood microcirculation, which negatively affects the functioning of the cardiovascular system as a whole. This situation requires examination of the child and identification of the cause of the appearance of multiple telangiectasias. In some cases, it can be caused by hereditary reasons (congenital weakness of blood vessels or features of the child's skin), but other pathologies related to the functioning of internal organs cannot be ruled out. [ 10 ]
Pathological telangiectasia can be distinguished from genetically determined telangiectasia using a plate made of transparent material (plastic or glass). It is placed on the spider vein and pressed lightly. If the neoplasm has changed color to a lighter color (merged with the skin), most likely, this is a hereditary feature of the body. However, just in case, it is better to play it safe and show the child to a specialist, because by diagnosing your child without sufficient knowledge and skills, we thereby take responsibility for the consequences, whatever they may be.
Complications and consequences
Spider veins are new growths of small vessels that show through the skin, thereby affecting its appearance. If we put aside the aesthetic side of the issue, then regardless of the reasons causing the swelling of the vessels and their increased visibility, such defects are not considered dangerous. It is not surprising that the fight against them is most often carried out in cosmetology rooms, and not in hospitals.
In some cases, you can see that the spider veins have disappeared on their own, in others they have to be removed (again, for the sake of cosmetic effect). But it is very important to understand that in cases where telangiectasia is a symptom of a disease, removing the symptom does not solve the problem. This is not a treatment method, which means that the disease will continue to progress, leaving more and more traces on the skin. On the Internet, you can find many reviews where people complain that removing spider veins gave only a temporary result. Defects appear again in the same or another place. [ 11 ]
However, given how unsightly spider veins look, people are increasingly inclined to believe that such defects need to be dealt with. There is no particular need to remove such defects, but if their presence causes mental problems: lack of confidence, decreased self-esteem, depression, etc., such a fight becomes a necessity.
Removing spider veins is a completely safe procedure, but there is a risk of skin infection at the site of the wound. In addition, it is very important to choose the right time for the procedure. Bright summer sun is not the best option for recovery after it, especially if the spider veins were removed with a laser. Moreover, sun exposure of the body after laser exposure significantly increases the risk of cancer.
After the procedure for removing telangiectasia, patients are often frightened when they see that the skin in the place where the spider vein was has turned red or dark spots have appeared on it, resembling bruises. This is a normal phenomenon associated with the cauterizing effect of the laser and small hemorrhages under the skin at the site of damage to the walls of thin vessels. Redness usually disappears within a couple of days. In case of infection, severe swelling, soreness at the site of the former telangiectasia, foci of suppuration may appear, the skin becomes locally warmer. The spread of infection may be indicated by a general increase in temperature. Hematomas disappear within 1-2 weeks.
Quite often, after fruitless attempts to get rid of the vascular network or if it is large, the owners of such "decoration" try to disguise it. A tattoo is considered as one of the interesting and fashionable options for disguising defects. But is it possible to make a tattoo on spider veins?
In principle, vascular defects located under the skin are not included in the list of contraindications to tattooing, as is varicose veins. There is only a mention of skin diseases, but telangiectasias are not included in them, although they are brought to dermatologists, who can recommend a consultation with a phlebologist if varicose veins are suspected. [ 12 ]
Moreover, today the removal of spider veins by laser is widely used, i.e. cauterization of telangiectasias, which in essence is not much different from applying a classic tattoo. Perhaps the sanitary conditions can be a bit of a debate, but even here you can always choose a professional who will not have any problems.
Besides, today tattoo is a common decoration, which is available even to children, because it can be done painlessly and quite safely - with the help of henna of different shades. Another thing is that any tattoo again does not solve the problem of spider veins in diseases. And a drawing on the face (if we are talking about rosacea ) is unlikely to be perceived positively in our society.
Whatever a person does in an attempt to get rid of an unaesthetic vascular defect, it is important to remember that health comes first. Failure to comply with hygiene requirements implies a high probability of wound infection, i.e. the development of a complication requiring specific treatment, which can also cause another skin defect (scars).
A very unpleasant consequence of ignoring the problem can be the progression of the existing disease. And this means that it is imperative to respond to the vascular signal and consult a doctor. If spider veins turn out to be the first sign of liver disease, varicose veins or hormonal disorders, this is a good chance to catch the disease at the very beginning, when it has not yet caused significant damage to health and the chances of its speedy recovery are high. [ 13 ]
Diagnostics vascular asterisks
Spider veins and spider veins, or scientifically telangiectasias, are considered by doctors as an external defect, for the detection of which no special tests or devices are required. In principle, people usually go to the doctor in connection with the detection of a swollen spider vein or isolated small veins. However, most often a person is concerned about the aesthetic side of the problem, and not health issues, so they do not always seek help from doctors, leaning towards removing the cosmetic defect in the conditions of cosmetology centers and clinics.
Whether such behavior is justified depends on the reason for the appearance of the vascular pattern. In some cases, the removal of neoplasms really does have a positive effect. And if the strange behavior of small vessels is not associated with a disease, there is nothing to worry about, this is a completely worthy solution to the problem. But if spider veins are a symptom of pathology, their removal does not lead to recovery. Moreover, it is simply impossible to get rid of defects completely in such conditions, new patterns will appear in the future, which once again indicates the need for complex treatment of the underlying disease and its manifestations.
But how can we understand what caused the change in the behavior of the vessels? Something can be told by how the spider veins look, where they are located, the prevalence of telangiectasias on the body, but only a specialist can determine the exact cause of their appearance. [ 14 ]
Since many patients treat spider veins as a harmless cosmetic defect, they seek advice from a dermatologist at best. If we are not talking about consistently swollen veins on the legs and a feeling of heaviness in them, then this option is not bad. After studying the patient's medical history and physical examination, the dermatologist can make a verdict on a possible hereditary predisposition, but can also recommend a consultation with a phlebologist (vascular surgeon).
The best option is to first contact your general practitioner or pediatrician if the vascular pattern is found on the child's body, and especially when it does not go away for a long time. And the general practitioner, having carefully examined the skin and familiarized himself with other symptoms, will already say which doctor is best to contact.
Regarding the tests, it can be said that they play a decisive role in this case, if we are talking about a study on hormones. After all, it is precisely the hormonal imbalance that often leads to a violation of the elasticity of the capillary and venous network. A clinical blood test, which a therapist can prescribe, is useful in terms of checking for coagulability and predisposition to the occurrence of blood clots. It will also be necessary in preparation for the procedure of removing neoplasms.
If vascular pathologies are suspected, and in particular varicose veins, instrumental diagnostics come to the rescue, which involves examining the venous vessels using ultrasound (Dopplerography). Such an examination is necessary to assess the blood flow in the vessels. [ 15 ]
Sometimes these diagnostic methods are sufficient to establish a diagnosis, in other cases the doctor may additionally prescribe an ultrasound examination of the abdominal organs, liver, kidneys, and a gynecological examination for women. In case of hormonal disorders not related to pregnancy, menopause, or the use of contraceptives, an endocrinologist consultation is necessary.
Differential diagnosis
Differential diagnostics for spider veins comes down to determining the reasons for their appearance. That is, the doctor needs to differentiate non-pathological spider veins and telangiectasias, which are a symptom of disease or hormonal disorders.
In childhood, strange moles of a bright red color, similar in appearance to spider veins, are sometimes found on the body and head of children. Both neoplasms are based on small vessels, but hemangiomas, as tumor formations, tend to increase in size, while spider veins are small in size and usually do not grow. As a benign tumor that is not prone to degeneration, hemangioma does not pose a particular danger and is treated with the same methods as telangiectasias.
Who to contact?
Prevention
Since spider veins, according to doctors, are quite safe neoplasms that can be safely removed without consequences for health, we can assume that the prognosis for their treatment is positive. But telangiectasias are not essentially a disease, but can only act as a symptom of certain disorders in the body. At the same time, the capillary network tends to recover after the damaged vessel is removed, so the procedure does not affect the processes of nutrition and respiration of tissues.
Small vessels, although they are an important component of the nutrition and gas exchange system in the body, do not play a decisive role in the circulatory system. There are a lot of them and the loss of a vessel is quickly compensated by the formation of others. But when exposed to factors that provoke the disease, new vessels can also become less elastic and flexible, so the removal of spider veins does not affect the prognosis of the underlying disease.
Regarding the prevention of spider veins, the opinions of doctors, cosmetologists and traditional medicine are somewhat different. Some cosmetologists and traditional medicine recommend strengthening blood vessels for preventive purposes in order to avoid their unjustified expansion, increase elasticity and resistance to stress. Other experts claim that there is logic in strengthening arteries and veins, which have a strong framework, but there is no point in strengthening the permeable capillary shell. And yet, both sides agree that in case of vein damage (varicose veins), strengthening blood vessels is useful and necessary. [ 16 ]
This can be done in various ways. With the help of cold foot baths, contrast showers (it causes alternate expansion and contraction of blood vessels, thereby training them), including in the diet foods rich in vitamins C, P, B5 (do not forget to pay attention to microelements: magnesium, manganese, zinc, calcium, etc.). Vitamin C is useful both as a stimulator of collagen synthesis and as a natural anticoagulant that prevents thrombus formation. Vitamin P reduces the fragility of the smallest vessels - capillaries, and pantothenic acid strengthens the vessels and prevents their damage.
Prevention of venous congestion can be considered physical exercise and an active lifestyle. If a person has to sit a lot, it is necessary to take active breaks during work (as they say, stretch your legs). When working standing, activity is also necessary, but you need to give your legs a rest by sitting on a chair and lifting them up a little, improving venous outflow.
Since people with excess weight are more prone to the development of varicose veins and the appearance of spider veins on the legs and body, then if you have it, there is a need to change your eating habits and control your body weight. Physical exercise and a low-calorie diet, but rich in vitamins and microelements, with a minimum salt content in dishes will also help here.
Massage of the legs and the whole body also helps improve blood circulation and tissue nutrition, strengthens blood vessels, but people who already have spider veins are not recommended to actively massage such areas. If the vascular pattern appears under the influence of cold or heat, do not wash with hot or too cold water (the best option is water at room temperature). Alcohol also helps to dilate blood vessels, so do not abuse it either internally or externally (for example, in lotions).
Hormonal imbalances have a negative effect not only on blood vessels, so it is worth seeing a doctor and adjusting your hormonal background, which will prevent the appearance of telangiectasias or help get rid of them. In the future, you need to carefully monitor the work of the endocrine and excretory systems, which will help avoid many problems, including spider veins. [ 17 ]
So, we have learned what spider veins look like and what diseases they can signal. It is high time to carefully examine your face, body, limbs and make sure that there are no such defects on them, and at the same time do everything so that they do not appear. Otherwise, there is a reason to think about whether everything in your body is functioning correctly or it is time to visit your doctor again and take care of your health.

