Medical expert of the article
New publications
Thymoma in adults and children
Last reviewed: 12.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Among the rather rare neoplasms, specialists distinguish thymoma, which is a tumor of the epithelial tissue of the thymus, one of the main lymphoid-glandular organs of the immune system.
Epidemiology
Among all cancers, the proportion of thymus tumors is less than 1%. The incidence of thymoma is estimated by the WHO at 0.15 cases per 100,000 people. And, for example, in China, the overall incidence of malignant thymoma is 6.3 cases per 100,000 people. [ 1 ]
Thymoma of the anterior mediastinum, which accounts for 90% of all tumors of the thymus gland, accounts for 20% of tumors in this location - in the upper part of the chest, under the sternum.
In other cases (no more than 4%) the tumor can occur in other areas, and this is a mediastinal thymoma.
Causes thymomas
The biology and classification of thymus-related neoplasms are complex medical issues, and the exact causes of thymic thymoma are still unknown. This tumor is found equally in men and women, and thymoma is more often found in mature adults.
But a tumor of the thymus gland in young people, as well as thymoma in children, is rare. Although the thymus (thymus gland) is most active in childhood, since the developing immune system requires a large number of T-lymphocytes, which are produced by this gland.
The thymus gland, reaching its largest size during puberty, gradually involutes (decreases in size) in adults, and its functional activity is minimal.
More information in the material - Physiology of the thymus gland (thymus)
Risk factors
Hereditary or environmental risk factors predisposing to the development of thymoma have not been identified either. And today, age and ethnicity are considered risk factors confirmed by clinical statistics.
The risk of this type of neoplasm increases with age: thymomas are more often observed in adults aged 40-50 years, as well as after 70 years.
According to American oncologists, in the United States this tumor is most common among Asians, African Americans, and Pacific Islanders; thymoma is least common among whites and Hispanics. [ 2 ]
Pathogenesis
Like the causes, the pathogenesis of thymoma remains a mystery, but researchers have not lost hope of solving it and are considering various versions, including UV irradiation and radiation.
The thymus produces T-lymphocytes, ensures their migration to peripheral lymphoid organs, and induces the production of antibodies by B-lymphocytes. In addition, this lymphoid-glandular organ secretes hormones that regulate the differentiation of lymphocytes and complex interactions of T-cells in the thymus and tissues of other organs.
Thymoma is an epithelial tumor and grows slowly - with the proliferation of normal or modified medullary epithelial cells (similar to normal ones). Experts note that the epithelial cells that make up a malignant thymoma may not have typical signs of malignancy, which determines the cytological characteristics of this tumor. And its malignant behavior, observed in 30-40% of cases, consists of invasion into surrounding organs and structures.
Analysis of the relationship between thymoma and other diseases has shown that almost all of them are autoimmune in nature, which may indicate impaired tolerance of immunocompetent cells and the formation of a persistent autoimmune reaction (cellular autoreactivity). The most common associated condition (in a third of patients) is myasthenia with thymoma. Myasthenia gravis is associated with the presence of autoantibodies to acetylcholine receptors of neuromuscular synapses or to the enzyme muscle tyrosine kinase.
A correlation has also been established between tumors of this type and such simultaneously occurring autoimmune diseases as: polymyositis and dermatomyositis, systemic lupus erythematosus, erythrocyte aplasia (in half of patients), hypogammaglobulinemia (in 10% of patients), bullous dermatoses (pemphigus), pernicious or megaloblastic anemia (Addison's disease), nonspecific ulcerative colitis, Cushing's disease, scleroderma, diffuse toxic goiter, Hashimoto's thyroiditis, nonspecific aortoarteritis (Takayasu's syndrome), Sjogren's syndrome, hyperparathyroidism (excess parathyroid hormone), Simmonds' disease (panhypopituitarism), Good's syndrome (combined B- and T-cell immunodeficiency).
Symptoms thymomas
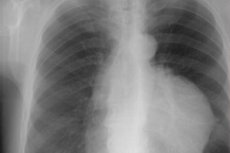
In 30-50% of cases, there are no symptoms of tumor growth in the epithelial tissue of the thymus, and, as radiologists note, a thymoma is accidentally discovered on a chest X-ray (or CT scan) during an examination carried out for another reason.
If the tumor manifests itself, the first signs are felt in the form of discomfort and pressure in the chest and retrosternal space, which may be accompanied by shortness of breath, persistent cough, chest pain of an unspecified nature and other signs of superior vena cava syndrome.
Patients with myasthenia gravis with thymoma complain of fatigue and weakness (for example, difficulty raising their arm to comb their hair), double vision (diplopia), difficulty swallowing (dysphagia), and drooping of the upper eyelids (ptosis). [ 3 ], [ 4 ]
Stages
The growth of thymoma and the degree of its invasiveness are determined by stages:
I – the tumor is completely encapsulated and does not grow into the fatty tissue of the mediastinum;
IIA – presence of tumor cells outside the capsule – microscopic penetration through the capsule into the surrounding adipose tissue;
IIB – macroscopic invasion through the capsule;
III – macroscopic invasion of adjacent organs;
IVA – there are pleural or pericardial metastases;
IVB – the presence of lymphatic or hematogenous metastases in extrathoracic areas.
Forms
The behavior of these tumors is unpredictable, and most of them are capable of developing into cancer and spreading beyond the gland. So thymomas can be benign or malignant; malignant (or invasive) thymoma is a tumor that behaves aggressively. Most Western experts classify thymoma as a malignant neoplasia. [ 5 ]
Having combined and systematized previously existing classifications of thymus tumors, WHO experts divided all types of thymomas depending on their histological type.
Type A is a medullary thymoma consisting of neoplastic epithelial cells of the thymus (without nuclear atypia); in most cases, the tumor is encapsulated and oval in shape.
Type AB is a mixed thymoma, which has a mixture of spindle and round epithelial cells or lymphocytic and epithelial components.
Type B1 is a cortical thymoma, consisting of cells similar to the epithelial cells of the gland and its cortex, as well as areas similar to the medulla of the thymus.
Type B2 is a cortical thymoma, the newly formed tissue of which has swollen epithelial reticular cells with vesicular nuclei and arrays of T cells and B cell follicles. Tumor cells can accumulate near the vessels of the thymus.
Type B3 – epithelial or squamoid thymoma; consists of lamellar growing polygonal epithelial cells with or without atypia, as well as non-neoplastic lymphocytes. It is considered a well-differentiated thymic carcinoma.
Type C – thymic carcinoma with histological atypia of cells.
When a thymoma behaves aggressively and invasively, it is sometimes called malignant.
Complications and consequences
The consequences and complications of thymoma are due to the ability of these neoplasms to grow into nearby organs, which leads to disruption of their functions.
Metastases are usually limited to the lymph nodes, pleura, pericardium, or diaphragm, and extrathoracic (outside the chest) metastasis – to bones, skeletal muscles, liver, abdominal wall – is rare.
In the presence of thymoma, patients have an almost fourfold increased risk of developing cancer, and secondary malignant neoplasms can be found in the lungs, thyroid gland, and lymph nodes.
In addition, thymoma – even after complete resection – can recur. As clinical practice shows, thymoma recurrences occur in 10-30% of cases 10 years after removal.
Diagnostics thymomas
In addition to anamnesis and examination, thymoma diagnostics includes a whole range of examinations. The tests prescribed are aimed at identifying associated diseases and the presence of paraneoplastic syndrome, as well as determining the possible spread of the tumor. This is a general and complete clinical blood test, an analysis for antibodies, the level of thyroid hormones and parathyroid hormone, ACTH, etc. [ 6 ]
Instrumental diagnostics involves visualization by mandatory chest X-ray (in direct and lateral projection), ultrasound and computed tomography. It may also be necessary to conduct thoracic MRI or PET (positron emission tomography).
On an X-ray, a thymoma appears as an oval, evenly or slightly wavy outlined shadow – a lobular density of soft tissue, slightly shifted to the side relative to the middle of the chest.
On CT, thymoma appears as a large accumulation of neoplastic tissue in the mediastinal region.
Using fine-needle aspiration biopsy (under CT control), a tumor tissue sample is obtained for histological examination. Although the ability to most accurately determine the type of neoplasm is only possible with postoperative histology - after its removal: due to the histological heterogeneity of thymomas, which complicates their classification into a specific type.
Differential diagnosis
Differential diagnosis should take into account the possibility of the patient having: thymomegaly, thymic hyperplasia, thymolipoma, lymphoma, nodular form of retrosternal goiter, pericardial cyst or tuberculosis of the intrathoracic lymph nodes.
Who to contact?
Treatment thymomas
As a rule, treatment of stage I epithelial thymic tumor begins with surgery to remove the thymoma (by complete median sternotomy) with simultaneous resection of the thymus – thymectomy. [ 7 ]
Surgical treatment of stage II tumors also involves complete removal of the thymus with possible adjuvant radiation therapy (for high-risk tumors).
At stages IIIA-IIIB and IVA, the following are combined: surgery (including removal of metastases in the pleural cavity or lungs) – before or after a course of chemotherapy or radiation. Perfusion chemotherapy, targeted and radiation therapy can be used in cases where tumor removal does not produce the expected effect, or the tumor is particularly invasive. [ 8 ]
Chemotherapy uses Doxorubicin, Cisplatin, Vincristine, Sunitinib, Cyclophosphamide and other anti-cancer drugs. Chemotherapy is given to all inoperable patients. [ 9 ], [ 10 ], [ 11 ]
Treatment of stage IVB thymoma is carried out according to an individual plan, since general recommendations have not been developed.
Forecast
Thymomas grow slowly, and the chances of a successful cure are much higher when the tumor is detected in the early stages.
It is clear that for stage III-IV thymomas, compared to stage I-II tumors, the prognosis is less favorable. According to statistics from the American Cancer Society, if the five-year survival rate for stage I is estimated at 100%, for stage II – at 90%, then for stage III thymomas it is 74%, and for stage IV – less than 25%.

