Medical expert of the article
New publications
Psoriatic arthritis
Last reviewed: 04.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Psoriatic arthritis is a chronic inflammatory disease of the joints, spine and entheses associated with psoriasis. The disease belongs to the group of seronegative spondyloarthropathies. Screening of patients for the purpose of early diagnosis is carried out by a rheumatologist and/or dermatologist among patients with various forms of psoriasis, actively identifying characteristic clinical and radiological signs of damage to the joints and/or spine and/or entheses. In the absence of psoriasis, taking into account the presence of first- or second-degree relatives.
Epidemiology
Psoriatic arthritis is considered the second most common inflammatory joint disease after rheumatoid arthritis; it is diagnosed in 7-39% of patients with psoriasis.
Due to the clinical heterogeneity of psoriatic arthritis and the relatively low sensitivity of diagnostic criteria, it is quite difficult to accurately estimate the prevalence of this disease. The assessment is often complicated by the late development of typical signs of psoriasis in patients suffering from inflammatory joint disease.
According to various authors, the incidence of psoriatic arthritis is 3.6-6.0 per 100,000 population, and the prevalence is 0.05-1%.
Psoriatic arthritis develops at the age of 25-55 years. Men and women are equally often affected, with the exception of psoriatic spondylitis, which is twice as common in men. In 75% of patients, joint damage occurs on average 10 years (but not more than 20 years) after the first signs of psoriatic skin lesions appear. In 10-15%, psoriatic arthritis precedes the development of psoriasis, and in 11-15% it develops simultaneously with skin lesions. It should be noted that in most patients there is no correlation between the severity of psoriasis and the severity of the inflammatory process in the joints, except for cases of synchronous occurrence of two diseases.
Causes psoriatic arthritis
The causes of psoriatic arthritis are unknown.
The role of trauma, infection, and neuro-physical overload are discussed as environmental factors. 24.6% of patients noted trauma at the onset of the disease.
 [ 11 ]
[ 11 ]
Pathogenesis
It is believed that psoriatic arthritis occurs as a result of complex interactions between internal factors (genetic, immunological) and environmental factors.
Genetic factors
Many studies indicate a hereditary predisposition to the development of both psoriasis and psoriatic arthritis: more than 40% of patients with this disease have first-degree relatives suffering from psoriasis, and the number of cases of these diseases increases in families with identical or fraternal twins.
To date, seven PSORS genes responsible for the development of psoriasis have been identified, which are localized in the following chromosomal loci: 6p (gene PSORS1), 17q25 (gene PSORS2), 4q34 (gene PSORS3), lq (gene PSORS4), 3q21 (gene PSORS5), 19p13 (gene PSORS6), 1p (gene PSORS7).
The results of immunogenetic phenotyping of patients with psoriatic arthritis are contradictory. Population studies have found an increased frequency of detection of the genes of the major histocompatibility complex HLA: B13, B17, B27, B38, DR4 and DR7. In patients with psoriatic arthritis and with radiographic signs of sacroiliitis, HLAB27 is more often detected. In the polyarticular, erosive form of the disease - HLADR4.
It is also worth noting the non-HLA-associated genes included in the region of the major histocompatibility complex, in particular the gene encoding TNF-a. When studying the polymorphism of the TNF-a gene, a reliable link was found between the alleles of TNF-a-308, TNF-b+252 and erosive psoriatic arthritis. In the case of early disease, this fact has prognostic significance for the rapid development of destructive changes in the joints, and the carriage of TNF-a-238 in representatives of the Caucasian population is considered a risk factor for the development of the disease.
 [ 12 ], [ 13 ], [ 14 ], [ 15 ], [ 16 ]
[ 12 ], [ 13 ], [ 14 ], [ 15 ], [ 16 ]
Immunological factors
Psoriasis and psoriatic arthritis are considered diseases caused by disorders of T-cell immunity. The main role is given to TNF-a, a key proinflammatory cytokine that regulates inflammation processes using various mechanisms: gene expression, migration, differentiation, cell proliferation, apoptosis. It has been found that in psoriasis, keratocytes receive a signal for increased proliferation when T-lymphocytes release various cytokines, including TNF-a,
At the same time, high levels of TNF-a are found in the psoriatic plaques themselves. It is believed that TNF-a promotes the production of other inflammatory cytokines, such as IL-1, IL-6, IL-8, as well as granulocyte-macrophage colony-stimulating factor.
The following clinical manifestations are associated with a high concentration of TNF-a in the blood of patients with psoriatic arthritis:
- fever;
- enthesopathies;
- osteolysis;
- the appearance of destructive changes in the joints:
- ischemic necrosis.
In early psoriatic arthritis, IL-10, TNF-a and matrix metalloproteinases are detected in elevated concentrations in the cerebrospinal fluid. A direct correlation has been shown between the levels of TNF-a, matrix metalloproteinase type 1 and markers of cartilage degradation. Intensive infiltration of T- and B-lymphocytes, in particular CD8+ T-cells, was detected in synovial biopsy samples from patients. They are also detected at the sites of tendon attachment to bone at an early stage of inflammation. CD4 T-cells produce other cytokines: IL-2, interferon y, lymphotoxin a, which are detected in the cerebrospinal fluid and synovium of patients with this disease. Frequent sporadic cases of psoriasis in HIV infection are one of the proofs of the participation of CD8/CD4 cells in the pathogenesis of psoriatic arthritis.
Recently, the issue of the causes of increased bone tissue remodeling in psoriatic arthritis in the form of resorption of the terminal phalanges of the fingers, the formation of large eccentric joint erosions, and a characteristic "pencil in cup" deformation has been discussed. During bone tissue biopsy, a large number of multinucleated osteoclasts were found in the resorption zones. To transform osteoclast precursor cells into osteoclasts, two signaling molecules are required: the first is the macrophage colony-stimulating factor, which stimulates the formation of macrophage colonies, which are osteoclast precursors, and the second is the RANKL protein (receptor activator of NF-кВ ligand), which triggers the process of their differentiation into osteoclasts. The latter has a natural antagonist, osteoprotegerin, which blocks the physiological reactions of RANKL. It is assumed that the mechanism of osteoclastogenesis is controlled by the ratio between the activity of RANKL and osteoprotegerin. Normally, they should be in equilibrium; when the RANKL/osteoprotegerin ratio is disturbed in favor of RANKL, uncontrolled osteoclast formation occurs. In synovial biopsies of patients with psoriatic arthritis, an increase in the RANKL level and a decrease in the osteoprotegerin level were detected, and in the blood serum, an increase in the level of circulating CD14- monocytes, precursors of osteoclasts.
The mechanism of periostitis and ankylosis in psoriatic arthritis is not yet clear; the involvement of transforming growth factor b, vascular endothelial growth factor, and bone morphogenic protein is suggested. Increased expression of transforming growth factor b was found in the synovium of patients with psoriatic arthritis. In an experiment on animals, bone morphogenic protein (in particular, type 4), acting together with vascular endothelial growth factor, promoted bone tissue proliferation.
Symptoms psoriatic arthritis
The main clinical symptoms of psoriatic arthritis:
- psoriasis of the skin and/or nails;
- spinal cord injury;
- sacroiliac joint damage;
- enthesitis.
Psoriasis of the skin and nails
Psoriatic skin lesions can be limited or widespread; some patients experience psoriatic erythroderma.
The main localization of psoriatic plaques:
- scalp;
- area of the elbow and knee joints;
- navel area;
- axillary areas; o intergluteal fold.
One of the common manifestations of psoriasis, in addition to rashes on the skin of the trunk and scalp, is nail psoriasis, which can sometimes be the only manifestation of the disease.
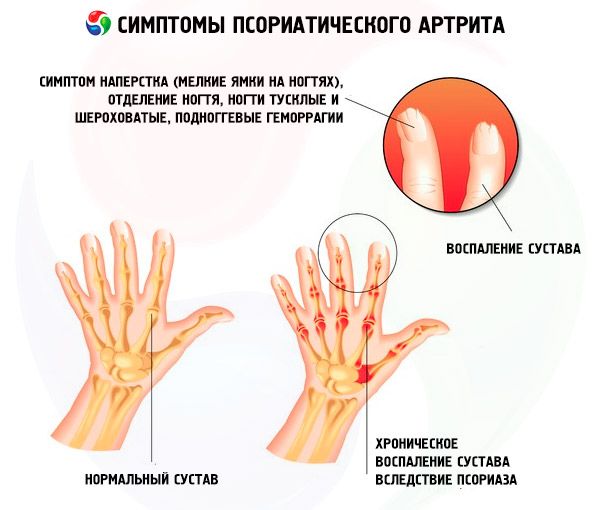
Clinical manifestations of nail psoriasis are varied. The most common are:
- thimble psoriasis;
- onycholysis:
- subungual hemorrhages, which are based on papillomatosis of the papillae with dilated terminal vessels (synonym subungual psoriatic erythema, "oil spots");
- subungual hyperkeratosis.
Peripheral psoriatic arthritis
The onset of the disease can be both acute and gradual. In most patients, the disease is not accompanied by morning stiffness, for a long time it can be limited and localized in one or several joints, such as:
- interphalangeal joints of the hands and feet, especially the distal ones;
- metacarpophalangeal;
- metatarsophalangeal;
- temporomandibular;
- wrist;
- ankle;
- elbow;
- knee.
Less often, psoriatic arthritis may debut with damage to the hip joints.
Often, new joints are involved asymmetrically, in the joints of the hands, randomly (chaotically). Characteristic signs of peripheral joint inflammation:
- involvement of the distal interphalangeal joints of the hands and feet with the formation of a "radish-shaped" deformity; o dactylitis;
- axial psoriatic arthritis with periarticular phenomena (simultaneous damage to three joints of one finger: metacarpophalangeal or metatarsophalangeal, proximal and distal interphalangeal joints with a peculiar cyanotic-purple coloration of the skin over the affected joints).
In 5% of patients, a mutilating (osteolytic) form is observed - the "calling card" of psoriatic arthritis. Externally, this is manifested by shortening of the fingers and toes due to resorption of the terminal phalanges. In this case, multiple multidirectional subluxations of the fingers are observed, and a symptom of "looseness" of the finger appears. Osteolysis also affects the bones of the wrist, interphalangeal joints of the hands and feet, styloid processes of the ulna, and heads of the temporomandibular joints.
Dactylitis is found in 48% of patients with psoriatic arthritis, many of whom (65%) have toes involved, with subsequent formation of radiographic signs of destruction of the articular surfaces. It is believed that dactylitis develops both due to inflammation of the flexor tendons and as a result of inflammation of the interphalangeal, metatarsophalangeal or metacarpophalangeal/metatarsophalangeal joints of one finger. Clinical manifestations of acute dactylitis:
- severe pain;
- swelling, edema of the entire finger;
- painful limitation of mobility, mainly due to flexion.
In combination with periarticular phenomena, the axial inflammatory process in the joints forms a "sausage-shaped" deformation of the fingers. Dactylitis can also be not only acute, but also chronic. In this case, thickening of the finger is noted without pain and redness. Persistent dactylitis without adequate treatment can lead to the rapid formation of flexion contractures of the fingers and functional limitations of the hands and feet.
Spondylitis
Occurs in 40% of patients with psoriatic arthritis. Often, spondylitis is asymptomatic, while isolated spinal lesions (without signs of peripheral joint inflammation) are very rare: they occur in only 2-4% of patients. Changes are localized in the sacroiliac joints, the ligamentous apparatus of the spine with the formation of syndesmophytes, paravertebral ossifications.
Clinical manifestations are similar to Bechterew's disease. Pain of inflammatory rhythm and stiffness are characteristic, which can occur in any part of the spine (thoracic, lumbar, cervical, sacral region). In most patients, changes in the spine do not lead to significant functional disorders. However, 5% of patients develop a clinical and radiological picture of typical ankylosing spondylitis, up to the formation of a "bamboo stick".
Enthesitis (enthesopathy)
Epthesis is the site of attachment of ligaments, tendons and joint capsule to bone, enthesitis is a frequent clinical manifestation of psoriatic arthritis, manifested by inflammation at the sites of attachment of ligaments and tendons to bones with subsequent resorption of subchondral bone.
The most typical localizations of enthesitis:
- the posterior-superior surface of the calcaneus directly at the site of attachment of the Achilles tendon;
- the place of attachment of the plantar aponeurosis to the lower edge of the calcaneal tuberosity;
- tibial tuberosity;
- the attachment site of the rotator cuff muscles of the shoulder (to a lesser extent).
Entheses of other localizations may also be involved:
- 1st costochondral articulation right and left;
- 7th costochondral articulation right and left;
- Posterosuperior and anterosuperior iliac spines;
- Iliac crest;
- Spinous process of the 5th lumbar vertebra.
Radiologically, enthesitis manifests itself as periostitis, erosions, and osteophytes.
Where does it hurt?
Forms
There are five main clinical variants of psoriatic arthritis.
- Psoriatic arthritis of the distal interphalangeal joints of the hands and feet.
- Asymmetric mono/aligoarthritis.
- Mutilating psoriatic arthritis (osteolysis of the articular surfaces with the development of shortening of the fingers and/or feet).
- Symmetrical polyarthritis (“rheumatoid-like” variant).
- Psoriatic spondylitis.
Distribution into the specified clinical groups is carried out on the basis of the following characteristics.
- Predominant damage to the distal interphalangeal joints: more than 50% of the total joint count is made up of the distal interphalangeal joints of the hands and feet.
- Oligoarthritis/polyarthritis: involvement of less than 5 joints is defined as oligoarthritis, 5 joints or more as polyarthritis.
- Mutilating psoriatic arthritis: detection of signs of osteolysis (radiological or clinical) at the time of examination.
- Psoriatic spondyloarthritis: inflammatory pain in the spine and localization in any of the three sections - lumbar, thoracic or cervical, decreased mobility of the spine, detection of radiological signs of sacroiliitis, including isolated sacroiliitis.
- Symmetrical polyarthritis: more than 50% of affected joints (paired small joints of the hands and feet).
Diagnostics psoriatic arthritis
The diagnosis is made based on the detection of psoriasis of the skin and/or nails in the patient or his close relatives (according to the patient), characteristic lesions of the peripheral joints, signs of damage to the spine, sacroiliac joints, and enthesopathies.
When interviewing a patient, it is necessary to establish what preceded the disease, especially whether there were complaints from the gastrointestinal tract or genitourinary system, eyes (conjunctivitis), which is necessary for differential diagnosis with other diseases of the seronegative spondyloarthropathies group, in particular with reactive postenterocolitic or urogenic inflammation of the joints, Reiter's disease (sequence of joint involvement, presence of complaints from the spine, sacroiliac joints).
 [ 26 ], [ 27 ], [ 28 ], [ 29 ], [ 30 ]
[ 26 ], [ 27 ], [ 28 ], [ 29 ], [ 30 ]
Clinical diagnosis of psoriatic arthritis
During the inspection, pay attention to:
- the presence of skin psoriasis in a characteristic location:
- scalp, behind the ears:
- navel area:
- perineal area:
- intergluteal fold;
- armpits;
- and/or the presence of psoriasis of the lips.
When examining the joints, characteristic signs of psoriatic arthritis are revealed:
- dactylitis;
- inflammation of the distal interphalangeal joints.
Palpate the tendon attachment sites.
The presence or absence of clinical signs of sacroiliitis is determined by direct or lateral pressure on the wings of the iliac bones and the mobility of the spine is determined.
The condition of the internal organs is assessed in accordance with general therapeutic rules.
Laboratory diagnostics of psoriatic arthritis
There are no specific laboratory tests for psoriatic arthritis.
Dissociation between clinical activity and laboratory parameters is often observed. RF is usually absent. At the same time, RF is detected in 12% of patients with psoriatic arthritis, which creates certain difficulties in diagnosis, but is not a reason to reconsider the diagnosis.
Analysis of cerebrospinal fluid does not provide specific results; in some cases, high cytosis is detected.
The activity of peripheral joint inflammation in psoriatic arthritis is assessed by the number of painful and inflamed joints, the level of CRP, the severity of joint pain and the activity of the disease.
Instrumental diagnostics of psoriatic arthritis
X-ray examination data of the hands, feet, pelvis, and spine are of great help in diagnosis, as they reveal characteristic signs of the disease, such as:
- osteolysis of articular surfaces with the formation of changes of the “pencil in a glass” type;
- large eccentric erosions;
- resorption of the terminal phalanges of the fingers;
- bone proliferations:
- asymmetric bilateral sacroiliitis:
- paravertebral ossificates, syndesmophytes.
Various authors have proposed variants of classification criteria that take into account the most striking manifestations of psoriatic arthritis, such as:
- confirmed psoriasis of the skin or nails in the patient or his relatives;
- asymmetric peripheral psoriatic arthritis with predominant damage to the joints of the lower extremities:
- hip,
- knee.
- ankle,
- metatarsophalangeal,
- tarsal joints,
- interphalangeal joints of the toes.
- distal interphalangeal joint disease,
- presence of dactylitis,
- inflammatory pain in the spine,
- sacroiliac joint disease,
- enthesopathies;
- radiographic signs of osteolysis;
- presence of bone proliferations;
- absence of the Russian Federation.
In 2006, the International Psoriatic Arthritis Study Group proposed the CASPAR (Classification Criteria for Psoriatic Arthritis) criteria as diagnostic criteria. The diagnosis can be established in the presence of inflammatory joint disease (lesions of the spine or entheses) and at least three of the following five signs.
- Presence of psoriasis, history of psoriasis, or family history of psoriasis.
- The presence of psoriasis is defined as a psoriatic lesion of the skin or scalp confirmed by a dermatologist or rheumatologist.
- History of psoriasis may be obtained from the patient, family physician, dermatologist, or rheumatologist. A family history of psoriasis is defined as the presence of psoriasis in first- or second-degree relatives (according to the patient).
- Typical psoriasis lesions of the nail plates: onycholysis, "thimble sign" or hyperkeratosis - recorded during physical examination.
- Negative RF test result using any method other than latex test: solid-phase ELISA or nephelometry is preferred.
- Dactylitis at the time of examination (defined as swelling of the entire finger) or a history of dactylitis recorded by a rheumatologist.
- Radiographic evidence of bone proliferation (ossification of joint margins), excluding osteophyte formation, on radiographs of the hands and feet.
Indications for consultation with other specialists
Psoriatic arthritis is often associated with diseases such as:
- hypertension;
- ischemic heart disease;
- diabetes mellitus.
If signs of the above diseases appear, patients need to consult with the appropriate specialists: cardiologist, endocrinologist.
In the event of development of signs of progressive destruction and deformation of the joints of the hands, ischemic necrosis of the supporting (hip, knee) joints, consultation with an orthopedic surgeon is indicated to decide on performing endoprosthetics,
Example of diagnosis formulation
- Psoriatic arthritis, monoarthritis of the knee joint, moderate activity, stage II, functional insufficiency 2. Psoriasis, limited form.
- Psoriatic arthritis, chronic asymmetric polyarthritis with predominant damage to the joints of the feet, high activity, stage III, functional insufficiency 2.
- Psoriatic spondylitis, asymmetrical bilateral sacroiliitis, stage 2 on the right, stage 3 on the left. Paravertebral ossification at the level of Th10-11. Psoriasis is widespread, nail psoriasis.
To determine activity, radiographic stage and functional insufficiency, the same methods are currently used as for rheumatoid arthritis.
What do need to examine?
How to examine?
Differential diagnosis
Unlike rheumatoid arthritis, psoriatic arthritis is characterized by the absence of pronounced morning joint stiffness, symmetrical joint damage, frequent damage to the distal interphalangeal joints of the hands and feet, and the absence of RF in the blood.
Erosive osteoarthrosis of the distal interphalangeal joints of the hands with reactive synovitis may also resemble psoriatic arthritis (distal form). However, as a rule, osteoarthrosis is not accompanied by inflammatory changes in the blood, signs of spinal damage (inflammatory pain in any part of the spine), psoriasis of the skin and nails. Unlike Bechterew's disease, psoriatic spondyloarthritis is not accompanied by significant functional disorders, often asymptomatic, sacroiliitis is asymmetrical, often slowly progressing, coarse paravertebral ossifications are detected on X-rays of the spine.
Certain difficulties for differentiation are presented by psoriatic arthritis, if the latter occurs with keratoderma of the palms and soles, nail damage. Differentiation of these diseases should be based on the nature of the skin lesion, as well as on the basis of the chronological relationship between the occurrence of joint inflammation and the acute urogenital and intestinal infection. In psoriatic arthritis, the rash is persistent. Patients often have hyperuricemia, which requires exclusion of gout. Diagnostic assistance can be provided by examination of cerebrospinal fluid, tissue biopsy (if there are tophi) to detect uric acid crystals.
Who to contact?
Treatment psoriatic arthritis
The goal of therapy is adequate impact on the main clinical manifestations of psoriatic arthritis:
- psoriasis of the skin and nails;
- spondylitis;
- dactylitis;
- enthesitis.
Indications for hospitalization
Indications for hospitalization are:
- complex differential diagnostic cases;
- poly- or oligoarticular joint lesions;
- recurrent psoriatic arthritis of the knee joints; need for injection into the joints of the lower extremities;
- selection of DMARD therapy;
- conducting therapy with biological agents;
- assessment of the tolerability of previously prescribed therapy.
Non-drug treatment for psoriatic arthritis
The use of a set of therapeutic exercises both in hospital and at home is especially important for patients with psoriatic spondylitis in order to reduce pain, stiffness and increase overall mobility.
For patients with low activity, spa treatment using hydrogen sulphide and radon baths is recommended.
Drug treatment of psoriatic arthritis
Standard therapy for psoriatic arthritis includes NSAIDs, DMARDs, and intra-articular GC injections.
NSAIDs
Diclofenac and indomethacin are mainly used in average therapeutic doses. Recently, selective NSAIDs have been widely used in practical rheumatology to reduce adverse effects from the gastrointestinal tract.
Systemic glucocorticosteroids
There is no evidence of their effectiveness based on the results of controlled studies in psoriatic arthritis, except for expert opinion and descriptions of individual clinical observations. The use of glucocorticosteroids is not recommended due to the risk of exacerbation of psoriasis.
Intra-articular administration of glucocorticosteroids is used in the mono-oligoarticular form of psoriatic arthritis, as well as to reduce the severity of sacroiliitis symptoms by administering glucocorticosteroids into the sacroiliac joints.
Basic anti-inflammatory drugs
Sulfasalazine: effective against the symptoms of joint inflammation, but does not inhibit the development of radiographic signs of joint destruction, usually well tolerated by patients, prescribed at a dose of 2 g/day.
Methotrexate: Two placebo-controlled studies have been conducted. One showed the efficacy of intravenous pulse methotrexate at a dose of 1-3 mg/kg body weight, another showed the efficacy of methotrexate at a dose of 7.5-15 mg/week orally, and a third showed a higher efficacy of methotrexate at a dose of 7.5-15 mg/week compared with cyclosporine A at a dose of 3-5 mg/kg. Methotrexate had a positive effect on the main clinical manifestations of psoriatic arthritis and psoriasis, but did not inhibit the development of radiographic signs of joint destruction.
When methotrexate was used in high doses, one patient died from bone marrow aplasia.
Cyclosporine: No placebo-controlled studies have been conducted. Controlled comparative studies of cyclosporine at a dose of 3 mg/kg per day and other DMARDs have shown a positive effect on the clinical manifestations of joint inflammation and psoriasis, as assessed by the overall assessment of the activity of psoriatic arthritis by the physician and the patient (average total effect). With a follow-up period of 2 years, it was noted that the progression of radiographic signs of joint damage slowed down.
Leflunomide: the drug's efficacy was demonstrated in an international double-blind controlled study. Leflunomide had a positive effect on the course of psoriatic arthritis, according to the count of painful and swollen joints, global assessment of disease activity by the doctor and the patient. In 59% of patients, as a result of treatment, improvement was achieved according to the criteria of therapy effectiveness PsARC (Psoriatic Arthritis Response Criteria), the main indicators of quality of life improved, the severity of psoriasis decreased (weak overall effect). At the same time, leflunomide slowed the development of destructive changes in the joints.
The drug is prescribed orally at a dose of 100 mg/day for the first three days, then 20 mg/day.
Gold salts and aminoquinoline drugs (hydroxychloroquine, chloroquine) are ineffective for psoriatic arthritis.
TNF-a inhibitors
Indications for the use of TNF-a inhibitors: lack of effect from DMARD therapy, in combination or separately, in adequate therapeutic doses:
- constant high" disease activity (the number of painful joints is more than three, the number of swollen joints is more than three, dactylitis is counted as one joint);
- acute dactylitis;
- generalized enthesopathy;
- psoriatic spondylitis.
The efficacy of infliximab in psoriatic arthritis has been confirmed by multicenter, placebo-controlled, randomized studies, IMPACT and IMPACT-2 (Infliximab Multinational Psoriatic Arthritis Controlled Trial), which included more than 300 patients.
Infliximab is administered at a dose of 3-5 mg/kg in combination with methotrexate or as monotherapy (in case of intolerance or contraindications to the use of methotrexate) according to the standard regimen.
The algorithm of psoriatic arthritis therapy depends on clinical manifestations. The sequence of prescribing the main groups of drugs.
- Peripheral psoriatic arthritis:
- NSAIDs;
- DMARDs;
- intra-articular administration of glucocorticosteroids;
- TNF inhibitors and (infliximab).
- Psoriasis of the skin and nails:
- steroid ointments;
- PUVA therapy;
- systemic use of methotrexate;
- systemic use of cyclosporine;
- TNF-a inhibitors (infliximab).
- Psoriatic spondylitis:
- NSAIDs;
- injection of glucocorticosteroids into the sacroiliac joints;
- pulse therapy with glucocorticosteroids;
- TNF-a inhibitors (infliximab).
- Dactylitis:
- NSAIDs;
- intra-articular or periarticular administration of glucocorticosteroids;
- TNF-a inhibitors (infliximab).
- Enthesitis:
- NSAIDs;
- periarticular administration of glucocorticosteroids;
- TNF-a inhibitors (infliximab).
Surgical treatment of psoriatic arthritis
Surgical treatment methods are necessary in case of destructive damage to large supporting joints (knee and hip joints, hand and foot joints) with pronounced functional disorders. In these cases, endoprosthetics of the hip and knee joints, reconstructive operations on the hands and feet are performed. Persistent inflammatory processes of the knee joints are an indication for surgical or arthroscopic synovectomy.
Approximate periods of incapacity for work
The duration of disability for psoriatic arthritis is 16-20 days.
Further management
After discharge from the hospital, the patient should be under the supervision of a rheumatologist and dermatologist at the place of residence in order to monitor the tolerability and effectiveness of therapy, promptly treat exacerbations of inflammatory processes in the joints, and assess the need for biological therapy.
What should a patient know about psoriatic arthritis?
At the first signs of inflammation in the joints, a patient with psoriasis should consult a rheumatologist. If you have been diagnosed with psoriatic arthritis, but subject to adequate and timely treatment, you can maintain activity and work capacity for many years. The choice of a therapy program depends on the clinical form of the disease, the activity of the inflammatory process in the joints and spine, the presence of concomitant diseases. During treatment, strive to fully comply with all the recommendations of the rheumatologist and dermatologist, regularly see a doctor to monitor the effectiveness and tolerability of all prescribed drugs.
More information of the treatment
Drugs
Forecast
If psoriatic arthritis progresses rapidly, accompanied by the appearance of erosive changes with significant impairment of joint function, especially in the case of a mutilating form of the disease or the development of ischemic necrosis of large (supporting) joints, the prognosis of the disease will be serious.
The combined standard mortality rate among patients is higher than in the population by an average of 60% and is 1.62 (1.59 in women and 1.65 in men).
 [ 50 ]
[ 50 ]

