Medical expert of the article
New publications
HPV type 45: what is it and how dangerous is it?
Last reviewed: 04.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
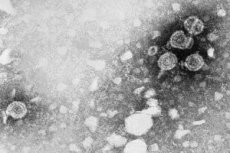
Having lived most of their life, by the age of 50, a person usually acquires a decent baggage of various diseases. Some of them are the result of poor nutrition, an unhealthy lifestyle, bad habits, etc., others are formed under the influence of various viruses and infections that enter the human body and parasitize inside it. Some types of such viruses, for example, HPV type 45, first described in 1987, in turn provoke the development of life-threatening health pathologies, which are usually called oncological. And since only those who are warned and have information are considered protected, we will try to provide the reader with the maximum amount of necessary information about such an insidious virus.
How dangerous is HPV type 45?
HPV is an abbreviation for a pathogenic factor known to us as human papillomavirus or papillomavirus. It is present in the body of a large number of people, since it is capable of moving from person to person quite quickly.
The papillomavirus is the cause of skin growths that people call warts. It would seem that there is nothing dangerous about it, because warts do not harm health, causing only some physical and psychological discomfort. But it is not that simple.
The fact is that the human papilloma virus has many varieties, each of which affects human health differently (according to various sources, from 100 to 600 strains, which is why they had to be numbered). For this reason, different types of the virus were divided into 4 classes, indicating how dangerous a given variety is for humans.
The safest non-oncogenic class of HPV includes types 1,2,4,5, 7, 10, 28, 41,53 and some others. These viruses cause the appearance of vulgar, flat and plantar warts on the body, which practically do not degenerate into malignant neoplasms.
HPV types 3, 6, 11, 13, 32, 42, 44 and some others are considered to be representatives of the class with low oncogenic risk. That is, pathology associated with these viruses detected at early stages does not develop into an oncological problem with timely and effective treatment. Otherwise, the risk of developing cancer still remains.
HPV 30, 35, 52 and several other types are a class of medium oncogenic risk. These types of the virus do not always lead to cancer, but under the influence of unfavorable factors over time, the disease is highly likely to develop into a malignant form.
Viruses 16, 18, 31, 33, 39, 45, 50 and some other types are considered to be high oncogenic factors. The presence of these viruses in the human body is very dangerous due to the high probability of developing oncological pathologies.
Let's be honest, the presence of HPV type 45 in the body increases the risk of benign neoplasms turning into malignant ones by tens of times, although the most oncogenic in this regard are still types 16 and 18 (for example, HPV type 45 is detected in only 5% of cervical cancer cases). However, this is not a reason to panic, because from the moment the virus enters the body until the start of the cell malignization process, more than one year usually passes. And even then, cell degeneration in this case occurs only under suitable conditions.
HPV type 45 is one of the viruses capable of causing pathological degeneration of cells of the vaginal mucosa and cervix in women. This means that it becomes one of the main causes of cervical cancer, and in particular cervical cancer. But do not think that once the virus enters the body, it will immediately cause the development of cancer. This is a long process that takes place in several stages, from the primary infection of the basal layer of the epithelium to irreversible changes in its structure, when cells begin to divide uncontrollably, thereby increasing the number of pathogenic clones. About 10 years can pass from the moment of infection with the virus to the appearance of malignant neoplasms against the background of reduced immunity.
Thus, if you undergo regular medical examinations, drawing the doctor's attention to the appearance of suspicious symptoms, such as the appearance of warts and condylomas on the body, inflammatory processes in the internal female genital organs, etc., you can prevent the transition of the disease to a malignant form.
Once in the human body, the papillomavirus remains there for a long time. It is almost impossible to remove it from the body, because the virus penetrates into cellular structures and lives there for a long time. To prevent the development of diseases caused by HPV, it is enough to introduce the virus into an inactive state, observing further measures that prevent its return to the active stage.
In some cases, after a while, the virus was not detected in the body even without treatment. But if it was diagnosed 3 or more times during the year due to an exacerbating disease, then the risk of developing epithelial cancer increases more than 10 times.
Structure HPV type 45
The human papilloma virus is presented in the form of spherical forms of very small size. The diameter of the HPV molecule does not exceed 55 nm. The molecules have a simple structure: a core containing a ring-shaped closed DNA consisting of 2 chains, and a protein shell (capsid).
The DNA of the papillomavirus contains two types of genes: early ones, designated by the letter E, and late ones, designated by the letter L. E-genes are responsible for the transfer of genetic information (replication of the genome) and cell modifications, and L-genes (regions of the genome L1 and L2) participate in the formation of the cell membrane. Between these regions is the region of long-term control (LCR), which regulates the synthesis of viral proteins.
Proteins E6 and E7 are considered responsible for the emergence of malignant neoplasms. They are capable of attaching to tumor-forming genes (p53 and Rb), causing cell transformation and their uncontrolled division. Moreover, in highly oncogenic viruses, such attachment occurs more actively.
The classification of HPV by type is based on the fact that different strains of the virus have different sequences of the E6 and L1 genes, due to which their behavior differs significantly: some do not manifest themselves in any way throughout a person’s life, others cause the appearance of benign neoplasms, and others, such as HPV type 45, provoke the transition of the latter to a malignant form, penetrating the structure of healthy cells of the body and gradually causing their malignization.
The life cycle of any virus is based on survival. And to do this, it needs to reproduce many similar molecules with the same properties (replication process). The virus itself cannot live, therefore, penetrating into a living organism, it begins to look for a host cell, forming one thing in common with it. The protein shell of the virus is able to bind to specific proteins of the host cell shell, where it forms a small gap through which it penetrates inside. It is on the basis of the host cell material that the virus forms its offspring.
Cell replication occurs in 2 stages: first, the chromosome set is doubled, and then the cell itself is divided into mother and daughter. When the cell divides, the daughter molecule acquires the properties of the mother molecule.
Damage to the cell's DNA can occur at both stages, and this is considered a natural accident. The cell program is such that with various damages the replication process is suspended, and at this time the p53 and Rb genes begin to correct errors. The attachment of viral oncoproteins E6 and E7 to them disrupts the process, and cell division ends with malignant mutations.
In principle, while the virus does not find the host cell, the E6 and E7 proteins are under the control of other proteins of the early and control region. But when they get into another environment, the oncoproteins lose control and begin to actively synthesize their own kind. Eventually, this situation leads to a disruption in the functioning of the host cell.
When penetrating the host cell, the virus can exist in it in 2 forms:
- The episomal form is characterized by the fact that the virus exists outside the chromosome set of the cell, and therefore is not capable of changing its characteristics. The infectious process in this case can proceed both in a hidden (latent) form and with the formation of benign warts and papillomas, which is considered a kind of protective reaction of the body.
- The integrated form is the introduction of the virus into the chromosome set of the host cell, which leads to a change in its properties and confuses the human immune system, which does not know how to treat such formations and loses control over their division. Uncontrollably multiplying, atypical cells cause tumor growth.
By the way, such a phenomenon as neoplasia or tissue dysplasia can be observed in both forms of HPV existence, while a benign process under the influence of certain factors can at any time change its character to malignant.
Routes of HPV penetration into the human body
The human papillomavirus, regardless of its type or strain, can live and reproduce only by parasitizing a living organism. It has several ways to penetrate the body.
HPV type 45, as one of the varieties of papillomavirus, can enter the body in several ways:
- during sexual intercourse (the virus is transmitted from an infected person sexually in the absence of protection during any type of sexual intercourse), the probability of infection is more than 50%,
- contact route (touching the genitals and secretions of the virus carrier, wearing his clothes, shaking hands),
- household route: through infected instruments (in a nail and dental salon, in a hospital if the equipment is not properly processed, when using cosmetic instruments and hygiene items of a person with papillomavirus, etc.), through air and water in public places (swimming pools, saunas, gyms),
- when passing through the birth canal (the baby can become infected from the mother if she had the virus in her body at the time of birth). Later, the mother can transmit HPV to the baby by contact, often touching the baby's naked body and genitals,
- There is also a possibility of self-infection by transferring virus cells to other parts of the body (usually during epilation or shaving, scratching the skin), medical workers can become infected with the virus as a result of medical procedures.
And yet, the most common cause of infection with the papillomavirus is considered to be unprotected sexual contact with people who are carriers of the virus (sometimes without even knowing it). At the same time, the virus entering the body does not necessarily mean that it will necessarily cause the development of some pathology or malignant process.
Thus, for HPV type 45 to lead to the development of oncopathology, one or more risk factors must be present:
- weakened immunity (in turn, a decrease in the body's immune response and resistance to infection, including viral infections, is facilitated by multiple diseases of internal organs and immune pathologies, a lack of vitamins in the body, bad habits, and previous therapy with cytostatics),
- the presence of an infectious factor in the body (bacteria, fungi, viruses) causing inflammatory processes in it, special attention should be paid to sexually transmitted infections and gynecological pathologies (chlamydia, gonorrhea, bacterial vaginosis, etc.),
- early onset of sexual activity, a large number of sexual partners, among whom may be virus carriers, people with cervical cancer, etc.,
- hormonal imbalances (during pregnancy and menopause, during and before menstruation, with diabetes, as well as while taking steroids and hormone therapy) and metabolic processes in the body,
- weakening of the nervous regulation of processes occurring in the body, under the influence of frequent stress and nervous tension,
- medical procedures on the genitals,
- hereditary predisposition to cancer (the risk of developing cancer is always higher in those people who have had cases of cancer of various etiologies in their family).
Symptoms
Human papillomavirus is a rather insidious form of a living organism that cannot imagine life without a donor. But even having entered the human body, the viral infection can behave differently depending on its condition.
Any type of HPV causes the appearance of various neoplasms (growths) on the skin and mucous membranes: warts, pointed and flat condylomas, papillomas, but not all types of the virus are capable of causing progressive tissue neoplasia (cancer). HPV type 45 is a type of virus with oncogenic properties.
However, this type of human papillomavirus does not always lead to the development of cancer. It is worth saying that in most cases, papillomavirus infection occurs in a latent form, i.e. there are no symptoms of the pathology. It is possible to detect cell mutation under the influence of the virus only through laboratory tissue testing.
Different types of the virus cause external symptoms in different parts of the body. With HPV type 45, neoplasms can be found on the skin and mucous membranes in the anal and genital area, as well as on the integuments of the internal genital organs in women. With the latent form of viral pathology type 45, the presence of the virus can be detected in the membranes of the cervix and vagina, although no external changes are noted.
Under the influence of provoking factors, the disease can become subclinical, when only individual, unexpressed symptoms of the pathology appear. Patients may complain of unpleasant sensations and itching in the genital area, experience discomfort during sex and urination, and discover strange growths in the genital area and anus. Later, similar neoplasms in the form of pointed or flat (especially dangerous) condylomas may be found on the inner surface of the vagina, cervix, and colon. Histological and cytological studies show the presence of hyperkeratosis (tissue compaction), and in some cases, even viral DNA is detected.
All this time, the virus is in human cells, not interacting with their DNA, but only causing increased proliferation of limited areas. But as soon as the immune system fails, the parasitic molecules integrate their DNA into the chromosome set of the host cell. The 3rd stage of pathology development begins - clinical (integrated form of virus existence).
At this stage, it is possible to observe a change in the structure of cells - koilocytosis, which is a sign that dysplasia of the vaginal or cervical tissues is caused by the human papilloma virus. So far, histological studies and colposcopy do not show the presence of malignant cells, but there is a noticeable proliferation of tissues on the genitals.
At stage 4 of the pathology, special laboratory tests and colposcopy will show the presence of mutated structures and cancer cells themselves, which, breaking away from the site of localization, can spread with the lymph flow throughout the body (invasive cancer).
Now, other symptoms are added to the existing ones, indicating severe pathological processes in the body: weakness, dizziness, deterioration of the skin, bloody discharge from the genitals, pain in the lower abdomen in women. Similar symptoms can be observed at stage 3 of the development of a viral infection, and it is possible to determine whether it is dysplasia or cancer only with the help of histological studies, colposcopy and biopsy (the latter is considered the most reliable method for diagnosing cancer).
HPV type 45 in women
Since HPV type 45 infection occurs both sexually and through contact, women, men, and even children can “catch” it. According to various sources, the incidence of human papillomavirus is from 60 to 90% of the population, and gender does not play a decisive role here.
However, we have already mentioned that for the virus carrier to develop into cancer, certain conditions are needed: reduced immunity, susceptibility to stress, the presence of inflammatory pathologies (most often gynecological and venereal), hormonal imbalances. Having studied the list of disease-provoking factors, it is easy to understand that women are more susceptible not so much to HPV infection (here the partners are in equal conditions), but to its transition to an integrated form with the development of malignant processes, in particular, cervical cancer and vaginal mucosa.
In most cases, the viral infection lurks for a long time in the body affected by gynecological pathologies of an inflammatory nature (vulvovaginitis, cervicitis, atypical type of cervical erosion, or pseudo-erosion). The virus often coexists with sexually transmitted infections (chlamydia, genital herpes, gonorrhea, etc.).
HPV type 45 in women can manifest itself with the following symptom complex:
- a sensation of itching or burning in the genital area without discharge, characteristic of candidiasis (fungal infection),
- the appearance of abundant, translucent, odorless discharge, sometimes with streaks of blood,
- unpleasant, often painful sensations when urinating,
- discomfort and pain during sexual intercourse,
- proliferation of tissues of the internal genital organs of an inflammatory nature (condylomatosis),
- the appearance of pointed condylomas or flat painful rashes of reddish or white color on the internal and external genitalia, in the perineum, on the mucous membrane of the large intestine,
- bleeding during a gynecological examination at later stages due to disruption of the epithelial structure and rupture of sensitive tissues during mechanical impact on them.
By the way, condylomas themselves are not a dangerous symptom that requires urgent treatment. They bring discomfort rather than harm. However, this is a signal symptom that should not be ignored under any circumstances.
The most dangerous symptom of HPV is dysplasia of the genital tissues, because it is considered a precancerous condition. The virus can wait for decades for the right moment to show its most insidious features, and neoplasia is a suitable environment for this, as soon as the immune system weakens.
HPV type 45 develops during pregnancy in the same way as in a normal state. However, hormonal changes in the body during this period can trigger the pathogenetic development of the human papilloma virus, which is fraught with cervical cancer.
Carrying the virus and its consequences do not affect the ability to have a child, or the birth process, or the intrauterine development of the fetus and its health. The thing is that the virus does not affect human reproductive function and cannot pass through the placental barrier, affecting the baby's tissues, even if the woman is diagnosed with dysplasia or cervical cancer.
Most often, infection with HPV type 45 does not entail miscarriage or various complications. As for newborns, only isolated cases of babies being born with laryngeal papillomatosis have been recorded, and only if the mothers were diagnosed with extensive papillomatous rashes on the genitals (contact route of infection transmission).
Risk factors for HPV to develop into a serious pathology include age over 35, the presence of sexually transmitted infections, pathologies of the cervix, ovaries and vagina, and immunodeficiency states.
 [ 9 ], [ 10 ], [ 11 ], [ 12 ], [ 13 ]
[ 9 ], [ 10 ], [ 11 ], [ 12 ], [ 13 ]
HPV type 45 in men
Men can get infected with HPV type 45 just like women, for example, through sexual contact. And since many representatives of the male population are polygamous and do not worry much about their health, the likelihood of infection with the virus increases even more, as does the risk of subsequently infecting their regular sexual partner (girlfriend, fiancée, wife).
Men are less susceptible to stress factors, and hormonal imbalance is diagnosed in them extremely rarely, so the chance of getting a serious pathology against the background of HPV is somewhat lower than in women. Nevertheless, even men are not immune from decreased immunity against the background of various health problems and bad heredity, and their widespread passion for smoking and drinking alcoholic beverages equalizes the chances of both sexes for complications in the form of cancer.
HPV type 45 is especially dangerous in terms of the development of oncological pathologies, and one should not think that cancer threatens only women. Men also have a certain risk of getting penile cancer with uncontrolled tissue growth in some of its areas, although it is lower than in women (average oncogenicity). Fortunately, pathology can be detected in men much earlier than in women, whose main genital organs are hidden deep inside.
Symptoms of the development of papillomavirus infection in men can be considered:
- genital discomfort (itching, some pain),
- the appearance of discharge from the penis not associated with ejaculation,
- pain during sexual intercourse and urination,
- condylomatous eruptions in the genital area (usually on the frenulum, head or foreskin of the penis) and perineum, as well as on the mucous membrane of the anus and large intestine.
Grayish or pink growths on the penis are easily injured, hurt and start bleeding. Sometimes they merge into groups, creating additional discomfort. Against the background of reduced immunity, there is an overgrowth of epidermal tissues of the organ, in which cancer cells can be detected over time (squamous cell carcinoma is most often diagnosed).
Diagnostics
Infection with HPV type 45 is not a situation that should not be ignored. Given the prevalence and high oncogenicity of this virus, as well as its ability to develop into cancer when the body's defenses are reduced, at the first symptoms of the pathology it is recommended to contact the appropriate doctor (for women, this is a gynecologist, for men, a urologist) for consultation and treatment. It is even better if the papillary virus infection is detected at an early stage during regular medical examinations, while it has not yet shown its parasitic abilities.
During the diagnostic period, if you suspect HPV of a highly oncogenic type, you should limit all sexual contacts to avoid infecting your partner. Remember that it is much easier to get infected with the virus than to get rid of it.
All diagnostic measures carried out during and after the initial examination are aimed at identifying oncologically dangerous types of the virus, since it is impossible to determine from external manifestations which type of virus caused the observed epithelial changes. For this purpose, the genotype of the virus, the duration of its presence in the human body and directly at the site where changes in tissues are noted (penis in men, vagina and cervical canal in women), the prevalence of the virus (the number of cells affected by it) are determined. It is also important to determine how deeply the virus has penetrated the cells and whether it has caused chromosomal changes.
If the presence of oncogenic viruses is suspected, cytological and histological examinations are performed (analysis of a smear taken from the cervical canal in women or the urethra in men). If there is neoplasia of organ tissue, colposcopy (urethroscopy) using reagents to which malignant cells are sensitive, and a biopsy of the material are mandatory.
Fans of anal sex will also have to provide a smear from the anus.
To establish the presence of the virus and determine its type, an accessible method of polydimensional chain reaction (PCR analysis) is used. The material for analysis is a scraping of epithelial cells of the cervical canal or urethra (in the absence of symptoms), and in the presence of unusual discharge, they are used as material (smear).
PCR analysis allows not only to detect the presence of HPV in the body, but also to determine its type. Thus, highly oncogenic types of the virus, which include HPV type 45, are quite easily determined in the material being studied.
Unfortunately, it is impossible to determine the degree of virus penetration into cells (viral load) using PCR analysis. A more modern method of research, the Daigen test, helps to cope with this task. It makes it possible to determine the type of virus (detect DNA of HPV 45 and other types with their characteristic features of the chromosomal set), its quantitative indicators and clinical load. Additionally, after some time, you can find out what is the risk of degeneration of epithelial cells into malignant ones.
It is important not only to detect the virus and identify it, but also to determine what kind of changes in the epithelial cells the patient has, whether there are atypical cells in the neoplasia area or whether the process is benign. The choice of further treatment regimen largely depends on this.
To determine the nature of changes in epithelial cells, the Papanicolaou method (or PAP testing) is used, with the help of which it is possible to determine the presence of macularized cells in the cervical canal.
Based on the testing results, the following conclusion is made:
- only normal cells are present,
- clear signs of an inflammatory process,
- there are single copies of atypical cells, which requires additional testing for malignancy,
- there is a sufficient number of atypical cells, which gives every reason to suspect oncology,
- There are a lot of atypical cells, which indicates the development of squamous cell carcinoma.
The ideal is to conduct the Daigen and PAP tests sequentially. If it is not possible to take the Daigen test, it is replaced by the PRP analysis.
Differential diagnosis
Differential diagnostics are carried out with such pathologies as molluscum contagiosum (infection caused by the smallpox virus), micropapillomatosis (softer non-infectious rashes on the genitals compared to papillomas), pearly papules on the penis (harmless neoplasms), seborrheic keratosis (benign pathology), intradermal nevi, carcinoma of the cervix (malignant pathology unrelated to papillomavirus infection).
If malignant cells are detected, patients are referred for consultation with an oncologist or oncogynecologist.
Treatment
Once a human papillomavirus infection enters the body, it tries to stay there forever, and since the virus is embedded in the body's cellular structures, it is currently impossible to remove it from there. The only way out is to put the virus into a dormant state.
The virus's activity can be suppressed by the body's own cellular immunity, but the disease will still be recurrent. It is believed that removing genital warts can reduce the risk of cell degeneration and help prevent transmission of the infection to a sexual partner. However, a certain risk remains in this case.
It is quite difficult to remove the virus from human blood, and it is not always possible. Therefore, more effective measures are still considered to be increasing cellular immunity, removing neoplasms, and treating cervical erosion and dysplasia in women.
Removal of genital warts and condylomas can be done using several methods:
- electrocoagulation or electroexcision (cauterization of growths with electricity, relapses are possible),
- laser removal (the most effective method),
- radio wave coagulation (also allows you to get rid of growths on the genitals forever),
- exposure to local chemicals,
- surgical removal (most often practiced for large condylomas, especially effective for cancer-hazardous neoplasms caused by HPV type 45 and similar forms of the human papillomavirus).
Cryodestruction is used only in cases where the neoplasms are small in size and there are few of them.
The procedures are performed under local or general anesthesia.
If there are no external manifestations of the disease, treatment is not carried out at all; only taking immunostimulants is recommended, which will help keep the virus under control.
If pointed or flat cancer-hazardous growths are found on the genitals of patients, then in addition to their removal, systemic antiviral therapy and strengthening of the immune system with appropriate means are carried out.
The goals of drug therapy are considered to be: destruction of HPV type 45 DNA and strengthening the body's defenses to mobilize them to fight the viral infection.
To combat the virus and prevent relapses of the disease, which are possible even after removal of condylomas and warts, antiviral drugs are used: Panavir, Acyclovir, Zorirax, Viferon, Groprinosin. It is good if the drugs have different forms of release, so that it is possible to affect the virus from all sides (local and systemic treatment).
As immunostimulants, you can use the drugs "Immunal", "Immunomax", "Lavomax", tincture of echinacea or eleutherococcus, vitamin complexes.
By the way, many drugs have both antiviral and immunomodulatory effects, which makes it possible to effectively solve the problem of HPV therapy.
Quite often, a bacterial infection joins a viral infection, which is most likely indicated by an inflammatory process in the vagina and cervical canal of the cervix. In this case, antibiotic therapy is carried out first, and then antiviral treatment.
If malignant cells are detected in the area of tissue neoplasia, depending on the stage of the pathology, surgical treatment will be used (modified radical hysterectomy plus lymphadenectomy of the pelvic lymph nodes to prevent the spread of processes within the body), chemotherapy and radiation therapy.
Treatment of external condylomas caused by HPV type 45 can also be carried out using folk methods (after consulting a doctor). To remove neoplasms, use fresh celandine juice (lubricate the condylomas 6 to 12 times a day) or oil based on this plant (mix equal parts of the crushed plant and vegetable oil and leave for 1 month in a dark place, lubricate the growths 2-3 times a day).
You can also lubricate condylomas and warts with dandelion or Kalanchoe juice.
For internal and external papilloma-like growths, you can take a decoction of herbs (lemon balm, horsetail, plantain, nettle plus dandelion root). The herbs are crushed and mixed in equal proportions. 1 tbsp. of the collection is poured with 1 glass of water, after which the composition is brought to a boil and kept for 10 minutes. After removing from the heat, the decoction is placed in a warm place for 3 hours, after which it can be taken orally an hour before meals 3 times a day. Single dose - 3 tbsp.
Any folk treatment is permissible only after consultation with a doctor. Its use is permissible within the framework of traditional treatment.
The effectiveness of treatment is monitored once every six months to a year by taking cytological and histological tests, as well as checking for the presence of the virus using PCR and PAP tests.
Prevention HPV type 45
The incidence of papillomavirus infection is approximately 6-9 people out of 10, depending on the region of residence. Such a widespread infection makes you think about how to protect yourself from its influence.
Currently, scientists have developed vaccines that prevent the development of genital cancer in both women and men. The Gardasil and Cervarix vaccines activate the immune system to fight cancer-causing viruses, but type 45 was not included in their list. Later, Gardasil was improved (the modified vaccine is called Gardasil 9), and now it can destroy even HPV type 45.
Usually, teenagers who are not yet sexually active are vaccinated, which means that presumably there is no HPV virus in their body. Most adults are already carriers of the virus, so vaccination is only possible with a negative HPV test result.
Other measures for preventing the human papilloma virus include rules that prevent infection and improve the immune system:
- limiting sexual contacts to one trusted partner,
- strict hand and skin hygiene,
- taking vitamin complexes and immunostimulating drugs (for prevention, it is better to use herbal infusions),
- timely treatment of inflammatory pathologies in the body (especially gynecological ones) and diseases that reduce immunity (ARI, ARVI, flu, gastrointestinal pathologies, etc.).
- a balanced diet rich in vitamins and minerals necessary for the body to function,
- healthy active lifestyle,
- limiting psychological stress (which is not always possible) and the ability to respond correctly to stress factors.
It is important to remember that without a strong immune system, it is impossible to effectively fight the virus. Therefore, special attention will have to be paid to the immune system throughout life.
Forecast
As for the prognosis for virus carriers, despite the high oncogenicity of HPV type 45, it can be fought quite successfully. The development of cancer under the influence of the papillomavirus is quite long (about 5-10 years), in addition, the symptoms of inflammation and viral infection appear much earlier, which provides good opportunities to prevent the transition of the disease to a malignant form. The main thing is not to neglect the pathology and strictly follow the doctor's instructions, both in terms of diagnosis and therapy.

