Medical expert of the article
New publications
Electrical cardioversion
Last reviewed: 29.06.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
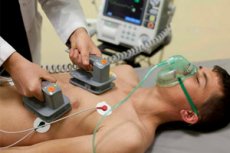
Electrical cardioversion is a medical procedure that uses a short electric shock directed at a patient's heart to restore a normal heart rhythm. This procedure is usually performed to treat serious arrhythmias (non-sinus rhythms of the heart) that may be dangerous to the patient's health or life.
Indications for the procedure
Indications for electrical cardioversion may include the following conditions and situations:
- Atrial Fibrillation (Atrial Fibrillation): ECV may be performed to restore normal heart rhythm in patients with atrial fibrillation, especially if other treatments such as medications have not produced the desired result. Atrial fibrillation may increase the risk of blood clots and stroke.
- Ventricular fibrillation: In ventricular fibrillation, especially if it causes unconsciousness or is life-threatening, ECV may be performed immediately to restore normal heart rhythm.
- Chamber arrhythmias: ECV may be indicated to correct chamber arrhythmias, such as chamber tachycardia or chamber fibrillation, if they cause serious symptoms or are life-threatening to the patient.
- Wide QRS tachycardia: For wide QRS tachycardias that are not amenable to medication and may cause serious symptoms, ECV may be considered as an intervention.
- Arrhythmias during surgery: If a patient is undergoing surgery and a cardiac arrhythmia occurs, ECV can be used to immediately restore normal rhythm.
- Physician judgment: Occasionally, a physician may decide to perform an ECV based on an extensive clinical evaluation and individual patient characteristics.
Indications for an EKV should always be evaluated by a physician, and the procedure is performed in the specialized setting of a medical clinic or hospital under the supervision of qualified professionals.
Preparation
The procedure is performed with specialized equipment and medical supervision, and requires preparation on the part of both the medical staff and the patient. Here are the basic steps to prepare for electrical cardioversion:
- Patient Assessment: Before performing electrical cardioversion, the physician should assess the patient's condition, including a history, physical examination, and necessary laboratory and instrumental tests. This helps ensure that the patient is suitable for the procedure and that it is safe for the patient.
- Diagnosis: The physician must accurately diagnose the arrhythmia and determine whether electrical cardioversion would be the most appropriate treatment.
- General anesthesia or local anesthesia: Depending on the clinical situation and the physician's recommendations, the procedure may be performed under general anesthesia so that the patient is completely immune to pain and unaware of cardioversion. In other cases, local anesthesia may be used to anesthetize the area where the electrodes will be placed.
- Continuous monitoring: Before, during and after the procedure, the patient will be under constant medical supervision to monitor their condition and response to cardioversion.
- Equipment Preparation: Medical personnel should prepare specialized equipment, including a defibrillator and electrodes that will be used to perform cardioversion.
- Physician commands: The physician and medical staff should prepare for the procedure and be ready to perform the necessary commands and actions during cardioversion.
- Patient Preparation: The patient may be given instructions regarding diet and medication prior to the procedure. It is important to inform the physician of all medications taken and any allergies.
- Consent for the procedure: The patient must give informed consent for electrical cardioversion after discussing the risks and benefits of the procedure with the physician.
Electrical cardioversion is a procedure that should be performed by medical professionals in specialized clinics or hospitals, and it requires strict training and supervision. It is important to trust experienced doctors and medical staff to perform this procedure.
Technique of the electrical cardioversion
The technique of electrical cardioversion (ECV) requires specialized training and medical equipment, and it is usually performed in specialized medical facilities such as hospitals and clinics. Here is a general overview of EKV techniques:
-
Patient Preparation:
- The procedure is explained to the patient and informed consent is obtained.
- The patient's medical history is evaluated, including allergies and other medical conditions.
- Sedation or general anesthesia is provided to the patient to ensure comfort and prevent pain during the procedure.
-
Equipment Preparation:
- Medical personnel prepare a defibrillator, which is used to administer an electrical shock.
- The electrodes that are connected to the defibrillator are placed on the patient's body. Two electrodes are usually used, one placed on the chest to the right of the sternum and one on the left side of the chest, below the collarbone.
-
Parameter setting:
- The physician or medical staff sets the defibrillator parameters, including the strength and duration of the electrical discharge and the frequency of the pulses.
- These parameters are customized depending on the type of arrhythmia and the patient's condition.
-
Pulse Administration:
- Once the parameters are set, the doctor or medical staff presses a button or activates the defibrillator to deliver a short electrical shock through the electrodes to the patient's heart.
- This pulse can "reset" the arrhythmia and restore a normal heart rhythm.
-
Monitoring and Surveillance:
- After ECV, the patient is monitored by physicians and medical staff in a specialized observation unit.
- The patient's heart rate and condition are monitored to make sure the procedure is effective and to prevent complications.
-
Additional Procedures:
- In some cases, it may take several ECV sessions to achieve a stable normal heart rhythm.
It is important to note that performing ECV requires specialized training and equipment and should be performed by experienced medical professionals trained in the procedure. This helps to ensure the safety and effectiveness of the procedure.
Contraindications to the procedure
Electrical cardioversion (ECV) is a procedure that can be very useful in treating serious arrhythmias, but it has contraindications and limitations. Below are some of the main contraindications to ECV:
- No indication: ECV is only performed in the presence of specific arrhythmias such as atrial fibrillation (AF), atrial fibrillation (AF) or ventricular fibrillation (VF). If there is no clinical indication for ECV, it is not performed.
- Patient condition: ECV can be dangerous for patients with certain conditions such as acute myocardial infarction or severe heart failure. Before performing the procedure, the physician must evaluate the patient's general condition and decide whether ECV is appropriate in his or her case.
- Uninvestigated arrhythmias: Before performing an EKV, the physician should ensure that the arrhythmia has been correctly diagnosed and classified. Uncontrolled or undetermined arrhythmias may require additional testing.
- Active infections: If a patient has active infections, especially in the sternal area or close to the electrode site, ECV may be delayed to prevent the spread of infection.
- Other cont raindications: Depending on the specific circumstances and condition of the patient, there may be other contraindications to performing ECV. These may include severe bleeding disorders, uncontrolled arterial hypertension, etc.
It is important to note that the decision to perform an ECV should always be made by the physician after careful evaluation of the patient and consideration of the patient's medical history. The patient should be informed of the plans and risks associated with the procedure and make an informed choice.
Complications after the procedure
Various complications can occur after an electrical cardioversion procedure. However, most complications are rare and are often related to the special circumstances and condition of the patient. It is important to note that cardioversion is usually performed with all precautions in place to minimize risks. Some of the possible complications are listed below:
- Chest pain: After the procedure, the patient may experience some pain or discomfort in the chest area. This may be due to the electrical discharge that is used to restore the heart rhythm.
- Arrhythmias: Electrical cardioversion may cause temporary arrhythmias of the heart rhythm. These arrhythmias are usually short-term and may require additional therapy.
- Thromboembolism: There is a risk of blood clots (blood clots), especially in atrial fibrillation. Anticoagulant therapy may be required after cardioversion to prevent thromboembolic complications such as stroke.
- Burns: If the electrodes do not fit properly against the skin, burns may result. Doctors and medical personnel must place the electrodes correctly and monitor the skin during the procedure.
- Decrease in blood pressure: In rare cases, cardioversion may cause a decrease in blood pressure, which may require additional medical support.
- Drug Complications: If a patient is taking certain medications, such as antiarrhythmic drugs, drug interaction complications may occur that require close monitoring and treatment adjustments.
- Allergic Reactions: In rare cases, patients may develop an allergic reaction to medications or materials used during the procedure.
After cardioversion, the patient is usually monitored by medical staff to identify and address any complications in a timely manner. Doctors and medical staff are obligated to do everything possible to ensure the safety and effectiveness of the procedure. If you have any concerns or questions about possible complications, be sure to discuss them with your doctor before the procedure.
Care after the procedure
Care after an electrical cardioversion (EC) procedure plays an important role in the patient's recovery and minimizing the risk of complications. Here are some recommendations and guidelines for care after this procedure:
- Medical observer: After the CV, the patient will be under medical observation to monitor their heart rate, blood pressure and general condition. This may take a few hours to a few days, depending on the clinical situation.
- Pain relief: If you have pain in your chest or skin where the electrodes are attached, tell the medical staff. You may be offered pain medication or other methods of pain relief.
- Rest: You may need to rest and avoid physical activity for some time after CV. This is usually recommended for a few hours to a few days, depending on individual circumstances.
- Heart rhythm monitoring: Depending on the cause of CV, you may be prescribed antiarrhythmic drugs or anticoagulants to control your heart rhythm and prevent thromboembolic complications.
- Diet and medications: Follow your doctor's recommendations about diet and medications. You may need to have your blood levels of antiarrhythmic drugs monitored regularly.
- Avoid alcohol and nicotine: Smoking cessation and moderate alcohol consumption can help restore heart health.
- Observe the electrode site: If there are signs of skin irritation, rash or redness where the electrodes were attached, notify the medical staff.
- Follow yourdoctor's recommendations: It is important to strictly follow all of your doctor's recommendations after CV, including medications, lifestyle changes, and follow-up visits.
- Watch for changes: It is important to closely monitor your condition after CV and report any unusual symptoms such as dizziness, shortness of breath, chest pain, or worsening arrhythmias to your doctor immediately.
- Follow-up exams: You may be scheduled for follow-up exams after your CV to evaluate the effectiveness of the procedure and to continue treatment if necessary.
Care after electrical cardioversion varies depending on the patient's specific situation and the reason for the procedure. It is important to follow the recommendations of your health care team to ensure the best results and minimize the risk of complications.
Clinical guidelines for the performance of electrical cardioversion
May vary depending on specific arrhythmias, patient condition, and medical standards. However, here are some general clinical guidelines that may be considered when deciding whether to perform ECV:
-
Diagnosis and Indications:
- ECV is usually considered a treatment option for patients with serious arrhythmias such as atrial fibrillation (AF), atrial fibrillation (AF), or ventricular fibrillation (VF).
- The decision to perform ECV should be based on an accurate diagnosis, the type of arrhythmia, and its duration.
-
Patient Assessment:
- The doctor should assess the patient's general condition, including medical history, presence of comorbidities, level of physical activity, etc.
- The evaluation helps determine if ECV is appropriate for this patient and what the risks may be.
-
Bleeding control: Patients who are taking anticoagulants or have clotting disorders may require treatment adjustments prior to EKV.
-
Preparing for the procedure:
- Before an ECV is performed, the patient is given information about the procedure and possible risks.
- The medical staff provides sedation or general anesthesia to prevent pain and discomfort.
-
Monitoring:
- The procedure is performed in specialized medical units where equipment is available to monitor the patient's heart activity and blood pressure.
- After ECV, the patient is monitored for a period of time to monitor the condition of the heart.
-
Additional Recommendations:
- The decision to perform an ECV can be individualized for each patient, and it can depend on many factors.
- In some cases, additional diagnostics, such as transesophageal echocardiography (TEEG), may be needed to more accurately assess the heart.
Clinical recommendations and the decision to perform ECV should always be made by a qualified cardiologist or electrophysiologist, taking into account the specifics of each clinical case and patient. This helps to ensure the safety and efficacy of the procedure.

