Medical expert of the article
New publications
Pharyngoscopy
Last reviewed: 03.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
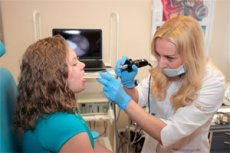
The standard procedure for examining the pharynx – pharyngoscopy – is performed by an otolaryngologist to determine its condition and diagnose diseases.
Types of pharyngoscopy
Depending on the location of the examination of the parts of the pharynx - upper (nasal), middle (oral) or lower (laryngeal) - there are different types of pharyngoscopy.
Oropharyngoscopy, upper pharyngoscopy or mesopharyngoscopy involves examining the oral part – the oropharynx.
Examination of the nasal part (nasopharynx) and its distal sections is called epipharyngoscopy or posterior rhinoscopy, which can be indirect and direct.
Hypopharynxoscopy (called indirect laryngoscopy) involves examining the lower part of the pharynx, the hypopharynx, or laryngopharynx.
Today, pharyngoscopy is also performed using a pharyngoscope, which is an electronic fiber-optic device equipped with a camera that transmits an image to a monitor. Modern endoscopic pharyngoscopy makes it possible to examine all parts of the pharynx and the upper part of the respiratory tract. For example, its use allows you to find out the anatomical causes of snoring and obstructive sleep apnea and decide how to get rid of this problem.
Indications for the procedure
Pharyngoscopy is an integral part of the examination of the pharynx, and indications for its implementation may be complaints of: irritation and pain in the throat (increasing with swallowing); sensation of a lump (foreign body) in the throat and difficulty swallowing; hoarseness or nasal voice; dryness and burning in the nasopharynx; difficulty breathing through the nose.
In the same cases, as well as in cases of acute respiratory diseases and acute respiratory viral infections, a pharyngoscopy is performed on the child.
The presence of the listed symptoms is characteristic of many acute and chronic diseases of the throat, and without a visual examination of the throat it is impossible to establish the true cause of the patient's complaints.
If an otolaryngological disease is suspected, pharyngoscopy is used to detect acute and chronic inflammatory processes in the mucous membrane of the pharynx, as well as pathologies of the tonsils, problems with the vocal cords, stenosis and neoplasms of the laryngopharynx.
Technique pharyngoscopies
The most common type of pharyngoscopy performed by otolaryngologists, therapists and pediatricians is oropharyngoscopy, and the technique for performing this examination is simple.
The doctor needs a spatula for pharyngoscopy and good lighting. ENT doctors use artificial lighting and a head reflector - a light-reflecting round mirror with a hole in the center.
The patient should open his mouth wide (and breathe through his nose), after which the doctor presses the back of the tongue downwards with a spatula and examines the walls of the oropharynx, palatine arches and tonsils. By pressing on the arch of the palatine tonsil (gland), the presence of the contents of its crypts is checked. And in order to lift the lateral glosso-epiglottic folds for better visualization of the pharynx (entrance to the pharynx), as well as to determine the degree of mobility of the soft palate, the patient is asked to say "a-a-a". [ 1 ]
If the patient has an increased gag reflex, the back of the throat is irrigated with an anesthetic spray containing lidocaine.
When examining the nasopharynx through the mouth - indirect epipharyngoscopy (posterior rhinoscopy) - nasopharyngeal mirrors of various diameters with a long handle and a spatula are used. Also, the nasopharynx can be examined through the nose - by direct epipharyngoscopy using a flexible endoscope, before inserting which the mucous membrane in the nose is treated with an anesthetic solution. In this way, pharyngoscopy of the adenoids is performed - the pharyngeal (adenoid) tonsil located in the back wall of the nasopharynx.
The algorithm for performing pharyngoscopy of the lower part of the pharynx (hypopharyngoscopy) is somewhat different from the types of examination already mentioned. Indirect (mirror) hypopharyngoscopy uses a laryngeal mirror, and the examination is performed with the tongue stuck out of the mouth, which is held and slightly pulled forward (using a gauze napkin, this can be done by a doctor or an adult patient). The doctor focuses the light with a forehead reflector and inserts a laryngeal mirror. For direct hypopharyngoscopy, a directoscope mirror is used. [ 2 ]
Pharyngoscopic signs of some diseases
Pharyngoscopy for angina (acute tonsillitis) visualizes the mucous membrane of the walls of the middle part of the pharynx (which is often called the throat), the uvula (the soft palate) and the palatine tonsils.
Pharyngoscopic signs of catarrhal tonsillitis include: pronounced redness and enlargement of the palatine tonsils, swelling of the arches, the presence of focal infiltrates or fibrinous film on the tonsils.
The most characteristic pharyngoscopic signs of follicular tonsillitis are: hyperemia and swelling of the palatine tonsils and arches, tonsillar fossa and soft palate; the presence of a large number of rounded yellowish-white (the size of a match head) suppurating lymphoid follicles on the tonsils.
Obvious pharyngoscopic signs of lacunar tonsillitis are manifested in the form of the same hyperemia and swelling of the palatine tonsils, as well as the presence of a yellowish-white coating on them and accumulation of pus in their lacunae (crypts).
Pharyngoscopic signs of acute pharyngitis /exacerbation of chronic pharyngitis are intense hyperemia and swelling of the mucous membrane of the pharynx (often the tonsils, arches and uvula) and serous plaque on the tonsils.
Pharyngoscopic signs of a retropharyngeal abscess – accumulation of pus in the retropharyngeal space at the level of the upper and middle parts of the pharynx – can be visualized as focal redness of the mucous membrane of the posterior pharyngeal wall and its protrusion. When a retropharyngeal abscess is localized at the level of the hypopharynx, diagnosis is made by X-ray or CT of the neck.
Complications after the procedure
Usually there are no consequences or complications after examination of the larynx. However, an allergy to local anesthesia is not excluded, as well as a reaction in the form of a gag reflex - if the spatula was inserted too deeply and touched the root of the tongue, innervated by the glossopharyngeal nerve.
Reviews
Feedback from doctors and patients regarding pharyngoscopy, as the main objective method of clinical examination in otolaryngology, confirms its essential role in the diagnosis of various diseases.

