Medical expert of the article
New publications
Malaria
Last reviewed: 04.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Malaria (English malaria; French paludisme) is an acute anthroponotic transmissible protozoan disease with a transmissible mechanism of infection, characterized by pronounced symptoms of intoxication, a cyclical course with alternating attacks of fever and periods of apyrexia, an enlarged spleen and liver, the development of hemolytic anemia with a progradient course, and relapses of the disease.
Epidemiology
The source of the infectious agent is a sick person or a parasite carrier whose blood contains gametocytes. Malaria is a transmissible infection transmitted by a mosquito bite. Gametocytes of P. vivax, P. ovale and P. malariae are found in the blood in the first days of the disease; their number increases after several cycles of erythrocytic schizogony. When infected with P. falciparum, a person becomes a source of infection 10-12 days after the onset of parasitemia and can remain so for 2 months or more.
With malaria, various mechanisms of infection transmission are possible:
Transmission mechanism (mosquito bite)
This mechanism is the main one, ensuring the existence of plasmodia as a biological species. The source of infection is a person (sick with malaria or a parasite carrier), in whose blood there are mature gametocytes (male and female reproductive cells of the parasite). Malaria carriers are only female mosquitoes of the genus Anopheles.
In the mosquito's stomach, where the male and female gametocytes inside the erythrocytes enter along with the blood, their further maturation (after the lysis of the erythrocytes), fusion and multiple division occur with the formation of sporozoites, which accumulate in the mosquito's salivary glands. Asexual forms of the parasite (trophozoites, schizonts), having entered the mosquito's stomach, die.
Thus, in the human body, an asexual path of parasite development (schizogony) occurs with the formation and accumulation of gametocytes, and in the mosquito body, a sexual path (sporogony) occurs, the fusion of male and female gametocytes with their further development and the formation of sporozoites.
 [ 4 ], [ 5 ], [ 6 ], [ 7 ], [ 8 ], [ 9 ]
[ 4 ], [ 5 ], [ 6 ], [ 7 ], [ 8 ], [ 9 ]
Vertical transmission mechanism
Vertical transmission mechanism (from mother to fetus) or from mother to newborn (during childbirth - parenteral mechanism). With vertical transmission, the fetus is rarely infected through the placenta. More often, infection occurs during childbirth when a certain amount of maternal blood enters the newborn's bloodstream, in the erythrocytes of which there are asexual forms of the parasite.
Parenteral mechanism of transmission
The parenteral mechanism of infection leads to the development of so-called schizont malaria. It is realized during blood transfusions or, less often, during violations of asepsis during injections (for example, among drug addicts using the same syringe). In case of infection during blood transfusion, the source of infection is a donor-parasite carrier, often with sublatent parasitemia (the number of parasites is less than five in one μl of blood). Therefore, in regions of the world endemic for malaria, it is necessary to use, along with parasitological methods (detection of the parasite in thick drop preparations and blood smears), serological (immunological) methods of laboratory diagnostics of malaria (RNIF, ELISA, etc.) to control donor blood. Considering that with parenteral infection, usually only a few parasites are introduced (especially with injections), the incubation period can be extended to 3 months (with massive infection, the incubation period, on the contrary, can be very short - several days), which is important to know when diagnosing malaria in patients who have undergone surgery and drug addicts.
Conditions of malaria spread
For malaria to spread in a certain region (country, territory, area), the following conditions are necessary:
- Source of infection (a patient with malaria or a parasite carrier).
- The presence of an effective carrier (mosquitoes of the genus Anopheles). Susceptibility to malaria parasites is the main quality of a specific species of mosquitoes of the genus Anopheles. The number of mosquitoes of the genus Anopheles among populations of other species is not as high as non-malaria mosquitoes, and they rarely seriously bother with their bites. However, even small species under other favorable circumstances (the proximity of mosquito breeding sites to human dwellings) can play a fairly serious role. More than 70 species of mosquitoes of the genus Anopheles (out of more than 200 known species) can serve as effective carriers of malaria.
- Favorable climatic conditions: average daily air temperature above 16 °C and the presence of breeding sites for mosquitoes: water bodies, water reservoirs, irrigation structures, etc. The minimum average daily air temperature required for development in the body of the Pl. vivax mosquito is 16 °C, for Pl. falciparum - 18 °C, at a lower temperature sporogony does not occur. The duration of sporogony is shorter, the higher the temperature (up to a certain level, since an average daily temperature of 30 °C and above is unfavorable for sporogony). At an optimal average daily temperature (25-26 °C), sporogony in Pl. vivax takes 8-9 days, in Pl. falciparum - 10-11 days.
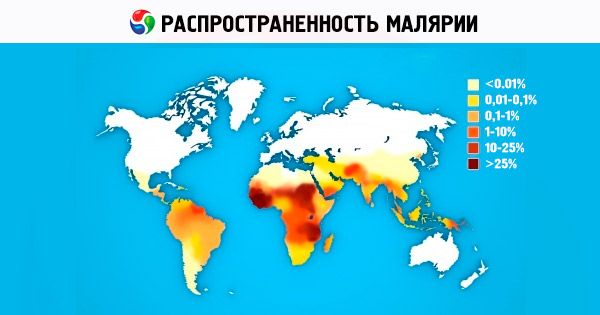
The entire area of distribution of malaria on the globe (between 45° N and 40° S to 64° N and 45° S in different years) is occupied by vivax malaria. The areas of falciparum malaria and malariae malariae are somewhat smaller due to the higher temperature required for effective sporogony; the area of ovale malaria is located in two regions that are not territorially connected with each other: tropical Africa and the states of the western part of the Pacific Ocean (Indonesia, Vietnam, the Philippines, New Guinea, etc.). In mountainous countries, foci of malaria can form at altitudes of up to 1000 m in the temperate climate zone and up to 1500-2500 m in the subtropical and tropical zone, with foci of only vivax malaria occurring at high altitudes (1000-1500 m and higher).
Malaria is characterized by pronounced seasonality. In temperate and subtropical climates, the malaria season is divided into periods of effective mosquito infection, infection transmission, and mass manifestations of the disease. The beginning of the period of effective mosquito infection (in the presence of a source of infection - patients, parasite carriers) coincides with the moment of a stable increase in the average daily temperature to 16 °C. The beginning of the transmission period is associated with the completion of sporogony in the mosquito's body, which depends on the specific average daily temperatures of a given year. In the Moscow region, the transmission period of vivax malaria can reach 1.5-2 months or more, until the first autumn frosts. The boundaries of the period of mass manifestations are less defined. In foci where only three-day malaria is transmitted, mass morbidity can begin long before the beginning of the transmission period. The observed cases are primary manifestations of vivax malaria with a long incubation period (3-10 months) due to infection in the previous season and the preservation of hypnozoites in the liver (without primary manifestations with a short incubation period), as well as distant exoerythrocytic relapses (after a series of attacks of malaria with a short incubation period in the previous season, without adequate anti-relapse therapy).
Susceptibility to malaria is universal. The outcome of infection after the pathogen enters the bloodstream and the clinical course of the disease are determined by the individual immunological status, the activity of non-specific innate resistance factors, the intensity of post-infection immunity, and for newborns - the level of specific antibodies of class G received from the mother. The exception is the indigenous people of West Africa and New Guinea, who are mostly immune to infection by Pl. vivax, which is associated with the genetically determined absence of erythrocyte isoantigens of the Duffy group, which act as receptors for Pl. vivax merozoites. Accordingly, in this region, cases of infection with vivax malaria are observed significantly less frequently than in other regions of tropical Africa.
People who carry abnormal hemoglobin (thalassemia, sickle cell anemia, hemoglobin E, C, etc.), with abnormalities in the structure of the erythrocyte cytoskeleton (hereditary spherocytosis, southeastern ovalocytosis, hereditary elliptocytosis) or who have a deficiency of the enzyme glucose-6-phosphate dehydrogenase of erythrocytes have relative resistance to infection by all types of plasmodia. In case of infection with malaria, they are mildly ill, the number of parasites in the blood remains at a relatively low level, and cases of malignant progression (cerebral malaria - falciparum) are practically absent. On the other hand, people with a deficiency of glucose-6-phosphate dehydrogenase are at risk of developing acute hemolysis when using a number of antimalarial drugs (primaquine, quinine, etc.). The mechanisms of natural resistance to various types of malaria are still largely unclear and continue to be studied.
Newborns also have a certain resistance to infection with all forms of malaria. This is due to:
- the presence of passive immunity due to class G antibodies received by the newborn from a hyperimmune mother (in areas with a high incidence of malaria);
- maintaining specific immunity after birth due to class A antibodies received by the newborn with breast milk;
- the presence of fetal hemoglobin in the newborn, which is of little use for feeding the malaria parasite.
After the first three to six months of life, newborns have a significantly increased risk of developing severe, malignant forms of falciparum malaria (change of red blood cells containing fetal hemoglobin to red blood cells containing normal hemoglobin; transition to mixed feeding - intake of para-aminobenzoic acid, necessary for the development of the parasite, which is absent in mother's milk).
 [ 10 ], [ 11 ], [ 12 ], [ 13 ]
[ 10 ], [ 11 ], [ 12 ], [ 13 ]
Immunity in malaria
Immunity to malaria is non-sterile, species- and strain-specific, unstable and short-lived. To maintain the protective level of antibodies, constant antigen stimulation in the form of repeated malaria infections is necessary. Immunity to Pl. malariae and Pl. vivax is established earlier and maintained longer than to Pl. falciparum. Antimalarial immunity includes cellular and humoral responses. The immune processes that stimulate antibody synthesis begin with phagocytosis of malaria parasites by macrophages. This is manifested by hyperplasia of the histiophagocytic system of the spleen, liver, and bone marrow.
Prevalence of malaria
Of the four species of human malaria pathogens, P. vivax is the most common in the world. In the subtropics and tropics, sporozoites predominate in the gene pool of the P. vivax population. They cause the disease after a short incubation (10-21 days). On the African continent, P. vivax is constantly found in the countries of East Africa among Arabs, Indians, Ethiopians, and Europeans. In the countries of West Africa, which is populated mainly by representatives of the Negroid race, P. vivax is not found, which is explained by the genetically determined innate immunity of African blacks to P. vivax [erythrocytes lack a receptor for P. vivax merozoites - Duffy isoantigens (Fy d or Fy b )]. The range of P. ovale is small and consists of two parts. The main, African part occupies tropical Africa from Gambia in the north to Congo in the south of the continent. The second part of the range is the countries of the Western Pacific Ocean and Southeast Asia. The geographic range of tropical malaria reaches 40° north latitude and 20° south latitude. P. falciparum causes up to 50% of malaria cases in the world. Four-day malaria is currently found in Africa, some areas of Central and South America, and the Caribbean. Southeast Asia.
Most people are susceptible to malaria. The exception is the indigenous population of West Africa. Hyperendemic areas of tropical Africa, where P. falciparum predominates, are characterized by a relatively stable immune structure of the indigenous population:
- Children under 6 months of age do not get sick due to passive immunity received from the mother:
- Most children aged 6-24 months are infected with P. falciparum; passive immunity has faded, active immunity has not yet developed; this group has the highest mortality from malaria:
- In children over 2 years of age, P. falciparum is detected less frequently, the course of malaria is mitigated as a result of acquired immunity, and the intensity of parasitemia decreases with age:
- In adults, P. falciparum is rarely detected due to high immune tension; when infected, there are no clinical manifestations.
Tropical malaria is also easily tolerated by carriers of abnormal hemoglobin S (sickle cell anemia) and people with certain other genetically determined abnormalities of hemoglobin and red blood cell enzymes (G-6-PDH deficiency).
History of malaria research
The study of malaria (one of the most ancient human diseases) is inextricably linked with the history of human civilization. It is assumed that malaria began to spread on Earth (from the African region of the Mediterranean) about 10,000 years ago due to the intensive development of agriculture, trade, and the exploration of new lands. In ancient Egyptian papyri, ancient Chinese literature, and the canons of classical ancient Indian medicine (Ayurveda), descriptions of the clinical picture and epidemics of malaria have survived to this day; even then, assumptions were made about a possible connection between the development of the disease and mosquito bites. Later (5th-6th centuries BC), ancient Greek doctors: Hippocrates, Heradotus, Empedocles described the clinical picture of malaria in detail. Hippocrates is credited with distinguishing malaria from the group of febrile diseases: he proposed distinguishing 3 forms of the disease: “quotidian” (daily attacks), “tertian” (attacks every other day) and “quartan” (attacks every 2 days).
The beginning of the era of scientific discoveries in the study of malaria is associated with 1640, when the Spanish doctor and conquistador Juan del Vego first used an infusion of cinchona bark to treat patients with malaria, previously used by the Indians of Peru and Ecuador as an antipyretic. The credit for naming the disease "malaria" (Italian: "mal aria" - bad air) goes to the Italian Lancisi (1717), who associated the infection of people with malaria through "poisonous" vapors from swamps. In 1880, the French doctor A. Laveran, working in Algeria, described in detail the morphology of the malaria pathogen. In 1897, the English military doctor Ronald Ross in India established the transmission mechanism of malaria.
Currently, malaria is one of the most serious health problems for more than 100 countries in Africa, Asia and South America, about half of the world's population lives at risk of contracting malaria. Almost all countries in Europe and North America annually register hundreds of imported cases of malaria among people arriving from regions where it is widespread, the number of cases of so-called airport malaria is growing. According to WHO, 200-250 million people in the world fall ill with malaria every year, at least 80% of all malaria cases are registered in African countries located south of the Sahara. Every year, 1 to 2 million people die from malaria, mainly children under 5 years of age. Social and economic losses in Africa alone are estimated at 2 billion US dollars per year. Since 1998, under the auspices of WHO, the World Bank, and UNICEF, a scientific and practical program (Roll Back Malaria Initiative) on malaria control (mainly in developing countries) has been implemented. The program is scheduled to run until 2010-2015. Developments to create an effective anti-malarial vaccine are actively underway, but this will require at least another 10-15 years. The search, development and improvement of drugs for the treatment of malaria are one of the priority programs of the WHO, various pharmaceutical companies, and research institutes around the world. In recent years, Russia has seen an increase in imported cases of malaria as a result of increased migration and intensive development of international tourism.
Causes malaria
The name of the disease "malaria" actually generalizes four separate protozoan diseases caused by four types of pathogens, respectively.
Malaria is caused by parasites belonging to the Protozoa type, Sporozoa class, Plasmodiidae family, Plasmodium genus. Four types of the pathogen parasitize humans: P. vivax causes three-day malaria, P. malariae causes four-day malaria, P. falciparum causes tropical malaria; P. ovale causes three-day ovale malaria.
Malaria pathogens
Exciter |
Form of malaria (according to ICD-10) |
Plasmodium (Laverania) falciparum |
Malaria caused by Plasmodium falciparum (falciparum malaria) |
Plasmodium (Plasmodium) vivax |
Malaria caused by Plasmodium vivax (malaria-vivax) |
Plasmodium (Plasmodium) ovale |
Malaria caused by Plasmodium ovale (malaria-ovale) |
Plasmodium (Plasmodium) malariae |
Malaria caused by Plasmodium malariae (malaria-malariae) |
In most domestic publications (textbooks, manuals, reference books), the previous names of the forms of malaria are retained: tropical malaria (malaria-falciparum), three-day malaria (malaria-vivax), oval-malaria (malaria-ovale) and four-day malaria (malaria-malariae).
Each of the four forms of malaria is characterized by its own clinical, pathogenetic and epidemiological features. The most important place is occupied by falciparum malaria, which accounts for 80-90% of all malaria cases in the world, the causative agent of which belongs to a special subgenus (Laverania). Only falciparum malaria can proceed malignantly, leading to a fatal outcome.
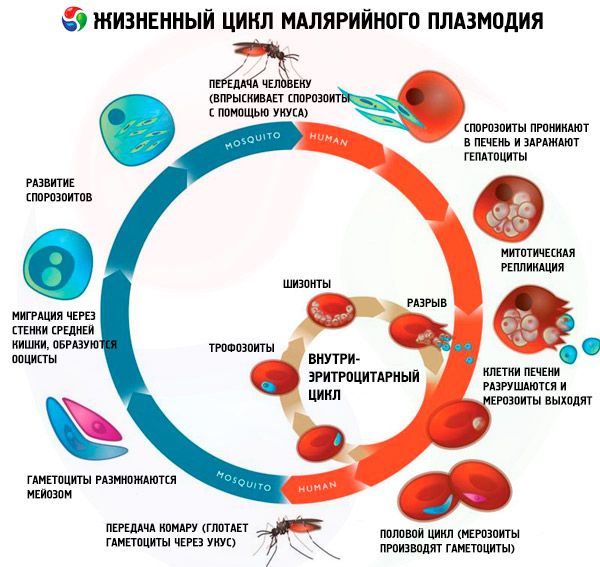
During their life cycle, malaria pathogens undergo the following development cycle with a change of hosts:
- asexual development (schizogony) occurs in the body of the intermediate host - a human;
- Sexual development (sporogony) occurs in the body of the final host - the female mosquito of the genus Anopheles.
Sporozoites enter the human body through the bite of an infected malaria mosquito. After entering the blood, sporozoites penetrate into hepatocytes from the sinusoidal vessels of the liver in 15-45 minutes and begin the exoerythrocytic cycle (tissue schizogony). The selectivity and speed of invasion are due to the presence of specific receptors on the membranes of hepatocytes. The parasites increase in size, divide repeatedly and form many small mononuclear formations - merozoites. The minimum duration of the exoerythrocytic cycle is 5-7 days for P. falciparum, 6-8 days for P. vivax, 9 days for P. ovale and 14-16 days for P. malariae. Then the merozoites leave the hepatocytes into the blood and penetrate into the erythrocytes, where erythrocyte schizogony occurs. Three-day and ovale malaria are characterized by a special type of exoerythrocytic development: all parasites or some of them are capable of being in hepatocytes for a long time (7-14 months or more) in a "dormant" state (hypnozoites), and only after this period they begin to transform into merozoites capable of infecting erythrocytes. Thus, this determines the possibility of long-term incubation and the occurrence of remote relapses up to 3 years.
Erythrocyte schizogony is accompanied by cyclic development and multiple division of parasites, with malarial plasmodia going through the following stages: young trophozoite (has a ring shape); developing trophozoite; mature trophozoite (has a large nucleus): developing schizont; mature schizont. After the completion of the schizogony process, the erythrocyte is destroyed. Free merozoites actively penetrate new erythrocytes, but most of them die from the effects of the host's protective immune mechanisms. The duration of erythrocyte schizogony is 48 hours in P. vivax, P. ovale, P. falciparum, and 72 hours in P. malariae. During the erythrocyte cycle, some merozoites transform into sexual forms - female (macrogametocytes) or male (microgametocytes).
Gametocytes enter the body of the mosquito-carrier when it feeds on the blood of a malaria patient or a parasite carrier. containing mature gametocytes. In the stomach of the mosquito, after 9-12 minutes, the male gametocyte ejects eight thin mobile flagella. Free flagella (microgametes) penetrate the female cell (macrogamete); after the fusion of the nuclei, a zygote is formed - a round fertilized cell. Then ookinetes, oocysts with sporozoites develop successively, their maturation occurs in the salivary glands of the mosquito. At an optimal ambient air temperature (25 °C), sporogony lasts 10 days in P. vivax, 12 days in P. falciparum, 16 days in P. malariae and P. ovale; at an air temperature below 15 °C, sporozoites do not develop.
Pathogenesis
All symptoms of malaria are caused by erythrocytic schizogony - the growth and reproduction of asexual erythrocytic forms of the parasite in the blood. Tissue schizogony is not clinically manifested.
A malarial attack is associated with the completion of erythrocytic schizogony, mass disintegration of erythrocytes and the entry into the blood of a large number of merozoites, metabolic products of parasites with pyrogenic and toxic properties that provoke the development of a febrile reaction. Due to the cyclic nature of erythrocytic schizogony, febrile attacks are repeated every 48 hours in three-day, oval- and tropical malaria and every 72 hours in four-day malaria. When a person is infected, a heterogeneous population of malarial parasites enters the body, and schizogony in the initial period occurs asynchronously, due to which the type of fever may be irregular. As immune reactions develop, the ability to parasitize in erythrocytes is preserved in one main generation of plasmodia, which determines the fever rhythm characteristic of this species. Only in tropical malaria can there be several (2-3) main generations of plasmodia, therefore the fever is often irregular.
Anemia, characteristic of malaria, is a consequence of the destruction of red blood cells by parasites located in them. It is known that P. vivax and P. ovale penetrate mainly into young red blood cells, P. malariae - into mature ones. P. falciparum infects red blood cells of varying degrees of maturity, which contributes to their more significant damage and hemolysis, therefore, in tropical malaria, hemolysis plays a leading role in the genesis of anemia. Additional factors in the hemolysis of red blood cells are also autoimmune mechanisms that damage uninfected red blood cells. Hyperplasia of the reticuloendothelial elements of the spleen, developing in malaria, inhibits hematopoiesis, which increases anemia and thrombocytopenia.
The enlargement of the liver and spleen is initially caused by congestion in the organs, but soon lymphoid and reticuloendothelial hyperplasia occurs in them. As a result of hemolysis of erythrocytes, as well as damage to hepatocytes, jaundice develops. A decrease in carbohydrate absorption and inhibition of gluconeogenesis in the liver causes hypoglycemia. Activation of anaerobic glycolysis leads to the accumulation of lactate in the blood, cerebrospinal fluid and the occurrence of lactic acidosis, which is one of the causes of severe tropical malaria.
In tropical malaria, the properties of erythrocytes change, which results in disruption of microcirculation (cytoadhesion, sequestration, rosetting). Cytoadhesion is the adhesion of infected erythrocytes to endothelial cells, the cause of sequestration in capillaries and postcapillary venules. The main role in cytoadhesion is given to specific ligand proteins (their expression on the surface of erythrocytes is induced by the parasite) and receptors located on the outer surface of endothelial cells. Occlusion of blood vessels causes ischemia of the affected organs. Protuberances (knobs) appear on the membranes of erythrocytes, which contact with pseudopod-shaped outgrowths formed on endothelial cells. Some varieties of P. falciparum cause healthy erythrocytes to adhere to infected ones, resulting in the formation of "rosettes". Red blood cells become rigid, which worsens the rheological properties of the blood and aggravates the microcirculation disorder. An important damaging factor is hypoxia caused by insufficient oxygen-transport function of infected red blood cells. Brain tissue is the least resistant to hypoxia, which contributes to the development of cerebral malaria. Disorders in the blood coagulation system occur: in severe tropical malaria, signs of DIC syndrome, thrombocytopenia and hypofibrinogenemia are observed. A certain role in the pathogenesis of tropical malaria is given to the generalized nonspecific inflammatory reaction. Vascular damage is caused mainly by the action of inflammatory mediators. The most active are lipid peroxidation products and proteases secreted by granulocytes. In the pathogenesis of severe malaria, considerable attention is paid to cytokines, in particular TNF and IL (IL-2 and IL-6). The most characteristic changes in severe tropical malaria occur in the brain, where edema, swelling of the brain matter, perivascular and periganglionic growths of neuroglia (Durk's granulomas) are observed. Capillaries are blocked by invaded erythrocytes and parasites; extensive hemostasis is observed. Perivascular edema with hemorrhages and focal necrosis develops. Based on the pathological picture, it can be concluded that in cases of malarial coma, specific meningoencephalitis develops.
Malaria infection can disrupt the host's immune response, which triggers a cascade of immunopathological reactions. Fixation of immunoglobulins and complement on the glomerular basement membranes causes acute nephropathy. Nephrotic syndrome, which develops in patients with four-day malaria, is classified as an immune complex glomerulopathy.
Life cycle of all malaria pathogens
The life cycle of all malaria pathogens includes two hosts: humans (schizogony - asexual development cycle) and mosquitoes of the genus Anopheles (sporogony - sexual development cycle).
Traditionally, three stages are distinguished in the schizogony cycle of all species of malaria parasites: exoerythrocytic schizogony (EESh), erythrocytic schizogony (ESH) and gametocytogony. In addition, a separate stage is distinguished in the life cycles of Pl. vivax and Pl. ovale - hibernation - due to the possible introduction of a morphologically heterogeneous group of sporozoites (tachysporozoites and bradysporozoites or only bradysporozoites) into the human body during a mosquito bite. In these cases, bradysporozoites (hypnozoites) are preserved in hepatocytes for a long time in an inactive state until the onset of EES.
 [ 19 ], [ 20 ], [ 21 ], [ 22 ]
[ 19 ], [ 20 ], [ 21 ], [ 22 ]
Exoerythrocytic schizogony
Sporozoites introduced into the human body with mosquito saliva very quickly (within 15-30 minutes) enter the liver with the bloodstream, where they actively penetrate hepatocytes without damaging them. Sporozoites of Pl. falciparum, Pl. malariae and tachysporozoites of Pl. vivax and Pl. ovale immediately begin EES with the formation of a large number of exoerythrocytic merozoites (up to 40,000 from one sporozoite in falciparum malaria). Hepatocytes are destroyed, and merozoites again enter the bloodstream with subsequent rapid (within 15-30 minutes) penetration into erythrocytes. The duration of EES for falciparum malaria is usually 6 days, for vivax malaria - 8 days, for ovafe malaria - 9 days, for malariae malaria - 15 days.
 [ 23 ], [ 24 ], [ 25 ], [ 26 ], [ 27 ], [ 28 ], [ 29 ]
[ 23 ], [ 24 ], [ 25 ], [ 26 ], [ 27 ], [ 28 ], [ 29 ]
Dormant stage
In vivax malaria and ovale malaria, bradysporozoites that have penetrated hepatocytes transform into inactive forms - hypnozoites, which can remain without dividing for several months or even years until subsequent reactivation (division and formation of merozoites). Thus, hypnozoites are associated with long incubation (up to 3-10 months or more) and the development of remote exoerythrocytic relapses, which are characteristic only of these forms of malaria.
Erythrocyte schizogony
After the introduction of merozoites into erythrocytes, malaria parasites repeatedly (cyclically) sequentially pass through the stages of: trophozoite (feeding, mononuclear cell), schizont (dividing multinuclear cell) and morula (formed parasites located inside the erythrocyte). Subsequently, after the destruction of erythrocytes, merozoites enter the blood plasma. The largest number of daughter merozoites is formed in tropical malaria - up to 40 in one erythrocyte. The ES stage lasts a strictly defined time: 48 hours for falciparum malaria, vivax malaria, ovale malaria and 72 hours for malariae.
Features of the erythrocytic schizogony cycle and the main pathogenetic mechanisms of development of severe and complicated forms of falciparum malaria:
- accumulation (sequestration) of invaded erythrocytes containing adult trophozoites (from the amoeboid trophozoite stage), schizonts in the vessels of internal organs, primarily the brain, as well as the kidneys, liver, intestines, bone marrow, placenta, etc.;
- the formation of so-called rosettes, consisting of invaded and uninfected erythrocytes;
- development of microcirculation disorders, tissue hypoxia, metabolic acidosis (significant accumulation of lactic acid);
- activation of the MFS (primarily Th-1 immune response) with increased synthesis of tumor necrosis factor-a, y-interferon, interleukin-1 and other cytokines that damage the vascular endothelium and cause adhesion of erythrocytes to the endothelium of blood vessels.
In recent years, the special role of increased synthesis of nitric oxide (NO) by cerebral vascular endothelial cells in the development of the cerebral form of falciparum malaria has been considered.
An important pathophysiological mechanism in the development of severe forms of falciparum malaria, compared to other forms of malaria, is hypoglycemia, which aggravates microcirculatory and metabolic disorders (metabolic acidosis) in patients, especially in children and pregnant women. Three main factors are distinguished in the development of hypoglycemia in falciparum malaria: decreased glucogenesis in the liver, glucose utilization by parasites, and stimulation of insulin secretion. At the same time, hypoglycemia may be a consequence of hyperinsulinemia developing after the administration of quinine to stop attacks of falciparum malaria.
As a consequence of prolonged persistence of the parasite (without adequate therapy) in malaria-malariae, nephrotic syndrome may develop as a result of an immune mechanism (deposition of immune complexes containing parasite antigens on the basal membrane of the renal glomeruli).
It should be noted that the main clinical manifestations of all forms of malaria (intoxication, enlarged liver and spleen, anemia) are associated with the stage of erythrocyte schizogony (repeated asexual reproduction of parasites in erythrocytes), and the higher the content of parasites in a patient's 1 μl of blood, determined by thick blood film microscopy, the more severe the malaria usually is. Therefore, in laboratory diagnostics of malaria, it is important not only to establish the type of malarial plasmodium, but also to determine the level of parasitemia. According to the maximum level of parasitemia, the forms of malaria are distributed in descending order: falciparum malaria (up to 100 thousand in μl or more), vivax malaria (up to 20 thousand in μl, less often more), ovale malaria and malariae malaria (up to 10-15 thousand in μl). In falciparum malaria, occurring with a high level of parasitemia (100 thousand per μl and higher), the risk of developing severe, fatal complications increases significantly, which determines the tactics of intensive (parenteral) antimalarial therapy.
The occurrence of febrile paroxysms in malaria is caused by hemolysis of erythrocytes, the release of merozoites into the plasma, the destruction of some of them (the other part of the merozoites is again introduced into erythrocytes), activation of the MFS and increased synthesis of interleukin-1, -6, tumor necrosis factor a and other endogenous pyrogens (inflammatory cytokines) that affect the thermoregulation center of the hypothalamus.
In the presence of one generation of plasmodia in the blood, regularly alternating paroxysms occur from the first days of the disease. Often, with falciparum malaria and vivax malaria (in hyperendemic regions with intensive transmission of malaria), non-immune individuals experience an initial (starting) fever associated with the development of several generations of pathogens in the erythrocytes of patients at once with different times for the end of the development cycle, which leads to the layering of attacks, smoothing out the period of apyrexia, and distortion of the typical paroxysm.
As the disease develops, specific and non-specific defense factors increase (by the end of the 1st-2nd week), some of the generations die, and one (two) leading generations of parasites remain with the development of typical paroxysms every other day (or every day).
Enlargement of the liver and spleen in all forms of malaria is associated with their significant blood filling, edema, and hyperplasia of the metastatic joint.
Malaria, as a rule, always leads to hemolytic hypochromic anemia, in the pathogenesis of which a number of factors are important:
- intravascular hemolysis of infected erythrocytes;
- phagocytosis of both infected and uninfected erythrocytes by reticuloendothelial cells of the spleen;
- sequestration (accumulation) of erythrocytes containing mature parasites in the bone marrow, suppression of hematopoiesis;
- immune mechanism (destruction of unaffected erythrocytes as a result of adsorption of immune complexes containing the C-3 fraction of complement on the erythrocyte membrane).
The gametocytogony stage is a kind of branch from the ES stage. Some of the merozoites (a genetically determined process), instead of repeating the asexual development cycle after being introduced into the erythrocyte, turn into sexual forms - gametocytes (male and female).
Features of the gametocytogonial stage in falciparum malaria:
- gametocytes appear in the peripheral blood no earlier than 10-12 days of illness;
- Gametocytes, accumulating during the course of the disease, can circulate in the bloodstream for a long time (up to 4-6 weeks or more).
In other forms of malaria (vivax, ovale, malariae), gametocytes can be detected in the peripheral blood from the first days of the disease and quickly (within a few hours to days) die.
Symptoms malaria
Taking into account the species characteristics of malaria parasites and the corresponding symptoms of malaria, four forms of the disease are distinguished: three-day malaria (vivax-malaria, malaria tertiana), four-day malaria (malaria quartana), tropical malaria (falciparum-malaria, malaria tropica), three-day oval malaria (ovale-malaria).
The course of primary malaria includes the initial period of the disease, the period of the peak of the disease and recovery. Without treatment or with inadequate etiotropic therapy, malaria goes into a period of relapse. There are exoerythrocytic and erythrocytic relapses, according to the time of development - early and late. Erythrocytic relapses are observed in infection with all types of plasmodia. Early ones occur within 2 months after the primary attacks; relapses that develop at a later date are considered late. Without treatment or with improper treatment of three-day and ovale malaria, a "lull" occurs lasting 6-11 months with the disappearance of parasites from the blood and clinical well-being. Then come late relapses (caused by the activation of hypnozoites in the liver), again replaced by a latent period without treatment, after which the disease recurs again.
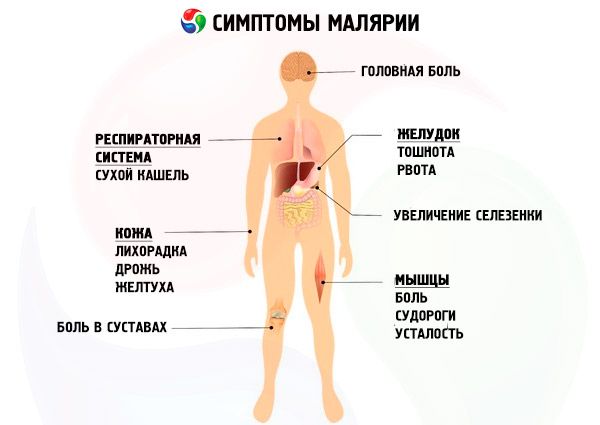
P. falciparum live in the human body (without treatment) for up to 1.5 years, P. vivax and P. ovale - up to 3 years, P. malariae - for many years, sometimes for life.
What's bothering you?
Forms
According to WHO recommendations, malaria is divided into uncomplicated, severe and complicated. Malignant forms of malaria and complications are characteristic mainly of infection with P. falciparum. The disease caused by P. vivax, P. ovale and P. malariae, as a rule, has a benign course.
Three-day malaria
The incubation period of three-day malaria is from 10-21 days to 6-14 months. Prodromal symptoms of malaria before the primary malarial attack are rarely observed, but they often precede relapses and are expressed by a feeling of general malaise, weakness, fatigue, pain in the lumbar region, limbs, a slight increase in body temperature, loss of appetite, headache. The duration of the prodromal period is on average 1-5 days.
At first, the temperature curve is irregular (initial fever), which is associated with the asynchronous release of several generations of P. vivax into the blood. Subsequently, typical malarial attacks begin with intermittent three-day fever, indicating the formation of the main generation of parasites in the blood. In a malarial febrile attack, three phases are clinically clearly expressed, immediately following one another: the stage of chills, heat and sweat. A malarial attack begins with chills, its intensity can vary - from mild shivering to stunning chills. At this time, the patient goes to bed, unsuccessfully tries to warm up, but the chills increase. The skin becomes dry, rough or "goose-like" to the touch, cold, the extremities and visible mucous membranes are cyanotic. The following symptoms of malaria are observed: severe headache, sometimes vomiting, pain in the joints and lumbar region. The chill stage lasts from several minutes to 1-2 hours, and is replaced by the fever stage. The patient takes off his clothes and underwear, but this does not bring him relief. The body temperature reaches 40-41 °C, the skin becomes dry and hot, the face turns red. Headache, pain in the lumbar region and joints intensify, delirium and confusion are possible. The fever stage lasts from one to several hours and is replaced by a period of sweating. The temperature drops critically, sweating is often profuse, so the patient has to change his underwear repeatedly. Weakened by the attack, he soon falls asleep. The duration of the attack is 6-10 hours. The onset of attacks of the disease in the morning and afternoon hours is considered typical. After the attack, a period of apyrexia begins, lasting about 40 hours. After 2-3 temperature attacks, the liver and spleen are clearly enlarged. Changes in the blood: anemia, developing gradually from the second week of the disease, leukopenia, neutropenia with a shift of band cells to the left, relative lymphocytosis, aneosinophilia and increased ESR.
In the natural course of the disease without etiotropic treatment, after 12-14 attacks (4-6 weeks), the intensity of the fever decreases, the attacks gradually subside, the size of the liver and spleen decreases. However, after 2 weeks to 2 months, early relapses occur, characterized by a synchronous temperature curve, an increase in the liver and spleen, and anemia. Subsequently, with the growth of immunity, the parasites disappear from the blood and a latent period begins. If treatment with histoschizotropic drugs is not carried out at this time, then after 6-8 months (and sometimes after 1-3 years), activation of the "dormant" tissue forms of parasites occurs and remote relapses develop. They are characterized by an acute onset, a milder course, an early increase in the spleen, a short number of attacks (up to 7-8), less intensity and duration of parasitemia, the presence of gametocytes in the blood.
Ovale malaria
In many clinical and pathogenetic features, ovale malaria is similar to three-day vivax malaria. The incubation period of ovale malaria is 11-16 days. With ovale malaria, the pathogen tends to primary latency. The incubation period can last from 2 months to 2 years or more. Symptoms of malaria include intermittent three-day fever, less often it is daily. Febrile attacks often occur in the evening hours, rather than in the first half of the day, as is typical for other forms of malaria. Ovale malaria is characterized mainly by a mild course with a small number of paroxysms that occur without pronounced chills and with a lower temperature at the peak of the attacks. It is characteristic that paroxysms during the primary attack very often stop spontaneously. This is explained by the rapid formation of stable immunity. If treatment with histoschizotropic drugs is not carried out, 1-3 relapses are possible with an inter-relapse interval from 17 days to 7 months.
Quartan
It usually proceeds benignly. The incubation period is from 3 to 6 weeks. Prodromal symptoms of malaria are rarely observed. The onset of the disease is acute. From the first attack, intermittent fever is established with a periodicity of attacks every 2 days. The paroxysm usually begins at noon, its average duration is about 13 hours. The period of chills is long and pronounced. The period of heat lasts up to 6 hours, it is accompanied by headache, myalgia, arthralgia, sometimes nausea, vomiting. Sometimes patients are restless and delirious. In the interictal period, the condition of patients is satisfactory. Anemia, hepatosplenomegaly develop slowly - not earlier than 2 weeks after the onset of the disease. Without treatment, 8-14 attacks are observed, but the process of erythrocytic schizogony at a low level lasts for many years. Most often, the infection occurs in the form of parasite carriage without activation of erythrocyte schizogony, which makes such individuals potentially dangerous donors. In endemic foci, four-day malaria causes nephrotic syndrome with an unfavorable prognosis in children.
Tropical malaria
The most severe form of malaria infection. The incubation period is 8-16 days. At the end of it, some non-immune individuals experience prodromal symptoms of malaria lasting from several hours to 1-2 days: malaise, weakness, fatigue, body aches, myalgia and arthralgia, headache. In most patients, tropical malaria begins acutely, without a prodromal period, with a rise in body temperature to 38-39 °C. If the cycles of erythrocytic schizogony in several generations of P. falciparum in an infected organism do not end simultaneously, this is often clinically expressed by the absence of a cyclical periodicity of febrile attacks. Attacks, occurring with an alternate change of phases, begin with chills lasting from 30 minutes to 1 hour. During this period, the skin is pale upon examination, cold to the touch, often with a roughness like "goose bumps". Chills are accompanied by a rise in body temperature to 38-39 °C. With the cessation of chills, the second phase of the paroxysm begins - fever. Patients experience a slight sensation of warmth, sometimes they experience a feeling of true heat. The skin becomes hot to the touch, the face is hyperemic. The duration of this phase is about 12 hours, it is replaced by mild sweating. Body temperature drops to normal and subnormal values and after 1-2 hours rises again. In some cases, the onset of tropical malaria is accompanied by nausea, vomiting, diarrhea. Sometimes catarrhal symptoms of malaria from the upper respiratory tract are recorded: cough, runny nose, sore throat. At a later stage, herpetic eruptions are observed on the lips and wings of the nose. In the acute stage, patients note hyperemia of the conjunctiva, in severe cases of the disease it can be accompanied by petechial or larger subconjunctival hemorrhages.
During the peak of tropical malaria, chills are less pronounced than in the first days of the disease, their duration is 15-30 minutes. Fever continues for days, periods of apyrexia are rarely recorded. In a mild course of the disease, the body temperature at its peak reaches 38.5 ° C, the duration of fever is 3-4 days; with a moderate degree of severity - 39.5 ° C and 6-7 days, respectively. Severe course of the disease is characterized by an increase in body temperature to 40 ° C and above, and its duration is eight or more days. The duration of individual paroxysms (and in fact the layering of several) in tropical malaria reaches 30-40 hours. The irregular type of temperature curve predominates, less often observed remittent, occasionally - intermittent and constant types.
Liver enlargement is usually determined on the 3rd day of the disease, spleen enlargement - also from the 3rd day, but it is usually recorded only by percussion; clear palpation becomes possible only on the 5th-6th day. During ultrasound examination of the abdominal organs, liver and spleen enlargement is determined already on the 2nd-3rd day after the clinical manifestations of tropical malaria have appeared. Pigment metabolism disorders are observed only in patients with severe and, less often, moderate tropical malaria. More than a threefold increase in serum aminotransferase activity is regarded as an indicator of an unfavorable prognosis. Metabolic disorders in tropical malaria include changes in the hemostasis system and hypoglycemia. Cardiovascular disorders are functional in nature and are expressed by tachycardia, muffled heart sounds, and hypotension. Occasionally, a transient systolic murmur is heard at the apex of the heart. In severe forms of the disease, changes in the ECG are observed in the form of deformation of the terminal part of the ventricular complex: flattening and inverse configuration of the T wave, lowering of the ST segment. At the same time, the voltage of the R waves in standard leads decreases. In patients with the cerebral form, changes in the P wave are of the P-pulmonale type.
In tropical malaria, CNS disorders associated with high fever and intoxication are often observed: headache, vomiting, meningismus, convulsions, drowsiness, sometimes delirium-like syndrome, but the patient's consciousness is preserved.
Characteristic signs of moderate and severe malaria infection are hemolytic anemia and leukopenia, eosinophilia and neutropenia, relative lymphocytosis are noted in the leukocyte formula. In severe forms of the disease, neutrophilic leukocytosis is possible; ESR is constantly and significantly elevated. Thrombocytopenia is a sign typical of all types of malaria. As with other infectious diseases, patients experience transient proteinuria.
Recurrent tropical malaria is caused by either inadequate etiotropic treatment or resistance of P. falciparum to the chemotherapeutic agents used. The natural course of tropical malaria with a favorable outcome lasts no more than 2 weeks. In the absence of etiotropic therapy, relapses occur after 7-10 days.
Pregnancy is a generally recognized risk factor for tropical malaria. This is due to the higher incidence of pregnancy, a tendency to severe clinical forms, a risk to the health and life of the child, and a limited therapeutic arsenal. Tropical malaria in children under five years of age should be considered a potentially fatal disease. In children of younger age groups (up to 3-4 years), especially in infants, malaria has a unique clinical picture: it lacks the most striking clinical symptom - malarial paroxysm. At the same time, such symptoms of malaria as convulsions, vomiting, diarrhea, abdominal pain are observed, with a rapidly progressing deterioration in the child's condition. The appearance of convulsions and other cerebral symptoms does not necessarily mean the development of cerebral malaria - this is often one of the symptoms of neurotoxicosis. Parasitemia in young children is usually high: P. falciparum can affect up to 20% of red blood cells. The disease can quickly become malignant and end in the death of the child.
Complications and consequences
Registered in all stages of tropical malaria. Prognostically unfavorable symptoms of malaria, indicating the possibility of developing a malignant form of malaria. - daily fever, lack of apyrexia between attacks, severe headache, generalized convulsions recurring more than twice in 24 hours, decerebrate rigidity, hemodynamic shock (systolic blood pressure below 70 mm Hg in an adult and less than 50 mm Hg in a child). This is also evidenced by high parasitemia (more than 100 thousand P. falciparum in 1 μl of blood), detection of various age stages of the parasite in the peripheral blood, the presence of gametocytes, increasing leukocytosis (more than 12.0x10 9 /l). Hypoglycemia less than 2.2 mmol/L, decompensated metabolic acidosis, more than a threefold increase in serum aminotransferase activity, as well as a decrease in the glucose level in the cerebrospinal fluid and a lactate level of more than 6 μmol/L are also prognostically unfavorable.
Severe CNS lesions in tropical malaria are united under the name "cerebral malaria", its main symptom is the development of a comatose state. Malarial coma can be a complication of primary, repeated and recurrent malaria, but it is more often observed in primary malaria, mainly in children, pregnant women and young and middle-aged people.
The cerebral form is the most common complication of severe falciparum malaria. In modern conditions, the cerebral form develops in 10% of all cases of falciparum malaria in the world, and 60-80% of all fatal outcomes of the disease are associated with this complication. The cerebral form can develop from the first days, but is more often recorded in the 2nd week of the disease due to the absence of specific or inadequate therapy. A fatal outcome can occur within 1-2 days. In the clinical picture of cerebral malaria, three periods are distinguished: stunning, stupor and true coma.
The stupefaction stage is characterized by mental and physical lethargy of the patient, rapid exhaustion. He orients himself in time and space, but reluctantly makes contact, answers questions in monosyllables, quickly tires. Tendon reflexes are preserved.
The sopor stage is expressed by deep prostration of the patient with rare flashes of consciousness. Ataxia, amnesia, convulsions, sometimes of an epileptiform nature, are possible. Corneal reflexes are preserved, pupils are normal. Tendon reflexes are increased, pathological reflexes occur.
In a coma, the patient is unconscious and does not respond to external stimuli. Convergence disorder, divergent strabismus, floating movements of the eyeballs with open eyelids (as if the patient is looking at the ceiling), horizontal and vertical nystagmus, paralysis of the sixth pair of cranial nerves are observed; tendon and abdominal reflexes are absent, vegetative functions are sharply impaired. Meningeal symptoms of malaria and pathological reflexes of Babinski, Rossolimo, etc. are expressed. Incontinence of urine and feces is noted. A lumbar puncture reveals an increase in intracranial pressure without pronounced disturbances in the protein and cellular composition of the cerebrospinal fluid. A high degree of parasitemia with various age stages of P. falciparum is determined in a thick drop and blood smear of patients with comatose malaria. At the same time, cases of fatal outcomes of cerebral malaria with a very low level of parasitemia are known. Cerebral malaria in children is often accompanied by anemia. Anemia worsens the neurological and somatic condition of the child. With effective treatment, consciousness usually returns suddenly.
In cerebral malaria, psychoses may develop as a consequence of dystrophic changes in the brain parenchyma. In the acute period, psychoses occur in the form of delirium, amentia, epileptic seizures, manic states. Post-malarial psychoses are characterized by depression, mental weakness, hysteria, schizophrenia-like syndromes, and in children, temporary delay in mental development. Sometimes, remote consequences of cerebral malaria are observed: hemiplegia, ataxia, focal symptoms of the cranial nerves, extrapyramidal disorders, mono- and polyneuritis.
A common complication of all forms of malaria infection is hypochromic anemia. Severe anemia is diagnosed when the hematocrit falls below 20% and the hemoglobin level is less than 50 g/l. The degree of anemia depends on the type of parasite, as well as the intensity and duration of the infection. The severity of malaria in indigenous peoples of tropical countries is often aggravated by a deficiency of iron and folic acid in the diet. After the first attacks of malaria, anemia may develop, which is more pronounced in tropical malaria than in other forms.
Infectious toxic shock (ITS) with the development of DIC syndrome is a complication characteristic of malaria-fаlсiраrum, occurring with high parasitemia. The development of acute adrenal insufficiency is characteristic. The course of infectious toxic shock in hot climates is accompanied by hypovolemia.
The development of acute renal failure is usually observed in malignant, complicated course of falciparum malaria. The development of oliguria and anuria with an increase in creatinine and urea in the blood is characteristic; urine analysis reveals pronounced proteinuria, cylindruria, pyuria, and microhematuria.
Nephrotic syndrome is a characteristic complication of malariae, characterized by a slow, steadily progressive course, accompanied by edema, arterial hypertension, proteinuria, and the development of renal failure.
Hemoglobinuric fever is a consequence of massive intravascular hemolysis both with intense invasion and as a result of the use of some antimalarial drugs (quinine, primaquine, sulfonamides) in individuals with a deficiency of the enzyme glucose-6-phosphate dehydrogenase. In its severe form, intense jaundice, severe hemorrhagic syndrome, anemia and anuria develop, accompanied by chills, fever (40 °C), pain in the lumbar region, repeated vomiting of bile, myalgia. arthralgia. Urine acquires a dark brown color, which is due to the presence of oxyhemoglobin. The number of erythrocytes in severe cases is reduced to 1x10 12 /l, and the hemoglobin level is down to 20-30 g /l. There are very few parasites in the blood with malarial hemoglobinuria or they are not detected at all. With rapid withdrawal of the antimalarial drug that caused hemolysis of red blood cells, the patient's condition improves without serious consequences. In severe cases, due to the development of acute renal failure, the prognosis may be unfavorable. In recent years, the autoimmune nature of the development of acute hemolysis associated with long-term and frequent use of antimalarial drugs - quinine and primaquine - has been considered. High fever is noted (with minor parasitemia), urine becomes black, anemia, leukocytosis, accelerated ESR are determined in the blood test, renal failure progresses rapidly, which leads to a fatal outcome in the absence of adequate therapy.
Malarial algid is characterized by clinical manifestations typical of infectious toxic shock: hemodynamic and microcirculation disorders, hemostasis system disorders, multiple organ failure and hypothermia. Unlike cerebral malaria, consciousness is preserved, although coma may develop later. Algid can develop against the background of pulmonary edema, metabolic acidosis and severe dehydration. A high level of parasitemia is noted. The prognosis largely depends on timely and correct treatment.
Acute pulmonary edema in patients with tropical malaria often leads to death. The mechanism of this severe complication has not been fully studied. Pulmonary edema can be provoked by excessive rehydration, but it can also develop against the background of normal pressure in the pulmonary circulation. Currently, most researchers consider acute respiratory failure in tropical malaria as a manifestation of adult respiratory distress syndrome.
A rare but serious complication of any clinical form of malaria with or without hyperreactive splenomegaly is splenic rupture. Rupture may be caused by torsion of the splenic pedicle with acute blood stasis and development of subcapsular hematoma.
In tropical malaria, lesions of the cornea of the eye, iritis, iridocyclitis, opacification of the vitreous body, optic neuritis, chorioretinitis and retinal hemorrhages are possible; there are reports of paralysis of the eye muscles caused by lesions of the III, IV and VI pairs of cranial nerves, and paralysis of accommodation.
Malaria relapses
The level of parasitemia during a relapse is usually lower than during primary symptoms of malaria. Due to the increased pyrogenic threshold during the course of the infection, clinical manifestations during a relapse usually occur with higher parasitemia. Relapses, as a rule, proceed benignly, with a moderately expressed toxic syndrome and a regular alternation of malarial paroxysms from the beginning of the relapse; the number of paroxysms is significantly less than during primary manifestations of the disease. According to the time of onset, early (development of clinical manifestations during the first 2 months after the primary manifestations of malaria) and late (after 2 months) relapses are distinguished. According to the origin, relapses are divided into erythrocytic (all forms of malaria) and exoerythrocytic (only in malaria-vivax and ovale).
Diagnostics malaria
Diagnosis of malaria is based on epidemiological data (stay in a malaria hotbed, absence or insufficiency of chemoprophylaxis), on the clinical picture of the disease (characteristic attacks) and is confirmed by laboratory tests.
Diagnosis of malaria should take into account:
- acute onset of the disease, pronounced symptoms of intoxication, cyclical course with alternating attacks of fever and periods of apyrexia, enlargement of the liver and spleen, development of progressive hemolytic anemia;
- epidemiological history data (stay in an area with a high risk of malaria, blood transfusion, drug addiction);
Duration of malaria, taking into account the development of relapses with a single infection and without adequate etiotropic therapy
Form of malaria |
Duration of infection |
|
Normal |
Maximum |
|
Malaria-falciparum |
Up to 1 year |
Up to 3 years |
Malaria-malariae |
Up to 2-3 years |
Possible for life |
Malaria-vivax and ovale |
Up to 1.5-2 years |
Up to 4-5 years |
- laboratory test results:
- hemogram results: decreased hemoglobin levels, leukopenia, lymphomonocytosis, increased ESR;
- results of microscopy of a thick blood drop (viewing at least 100 fields of view in cases of low parasitemia): detection of plasmodia and determination of the level of parasitemia in 1 µl of blood (100 fields of view - 0.2 µl of blood).
This is necessary:
- To select the degree of intensity of specific antimalarial therapy (with a high level of parasitemia in patients with tropical malaria, parenteral administration of drugs is preferable).
- To monitor the effectiveness of specific therapy.
The level of parasitemia can also be assessed by counting the percentage of affected erythrocytes per 100 leukocytes in a thick drop of blood (in this case, to assess the number of parasites in 1 μl, it is necessary to know the total number of leukocytes and erythrocytes in 1 μl in the patient);
- microscopy data of a blood smear to determine the type of plasmodium. The thick drop and blood smear are stained using the Romanovsky-Giemsa method.
As a result of the accumulation of invaded erythrocytes containing adult trophozoites and schizonts in the vessels of internal organs, when examining a thick drop preparation in mild falciparum malaria, only young (juvenile) trophozoites at the ring stage are determined in erythrocytes. The appearance in the peripheral blood of invaded erythrocytes containing adult stages of parasite development (adult or amoeboid trophozoites, schizonts) is an unfavorable laboratory sign indicating a severe (complicated) course of falciparum malaria.
Degrees of parasitemia in malaria
Degrees of parasitemia |
Conventional designation |
Number of parasites in the visual fields |
The number of parasites in 1 µl of blood |
IV |
+ |
1-20 in 100 fields |
5-50 |
III |
+ + |
10-100 in 100 fields |
50-500 |
II |
+ + + |
1-10 in 1 field |
500-5000 |
I |
+ + + + |
More than 10 in 1 field |
More than 5000 |
In individuals who have had first contact (non-immune) with this infection, young children, the first attacks may occur with very low parasitemia, sometimes not detectable by microscopy; this requires a repeat blood test (thick drop) after 6-12 hours, but not later than 24 hours.
Laboratory diagnostics of malaria involves microscopic examination of blood samples (thick drop and thin smear methods) stained according to Romanovsky-Giemsa.
The following patients are subject to examination for malaria: febrile patients with an unspecified diagnosis for 3 days during the epidemic season and 5 days during the rest of the year; patients with continuing periodic increases in body temperature despite treatment in accordance with the established diagnosis; blood recipients with an increase in body temperature in the last 3 months after transfusion; persons living in an active focus, with any increase in body temperature. It should be taken into account that during the first attacks of malaria, the number of parasites in the peripheral blood is small, so the most thorough examination is necessary. Malaria with low parasitemia also occurs in persons who took antimalarial drugs for prophylactic purposes (suppressive therapy) or drugs (tetracycline, sulfonamides) that have a suppressive effect on malaria plasmodia before the disease. Blood sampling for examination is recommended to be performed both during fever and apyrexia. To detect parasites, a thick drop is examined, since the volume of blood in it is 30-40 times greater than in a thin smear. In case of high parasitemia, the malaria pathogen is detected even when examining a thin smear. The morphological features and tinctorial properties (stainability) of different age stages of asexual forms in erythrocytes are clearly distinguishable in a thin smear. It is necessary to determine the type of parasite: this is especially important for P. falciparum. In uncomplicated tropical malaria, P. falciparum is observed in the peripheral blood only in the stage of young ring-shaped trophozoites. In case of primary infection, more mature stages of the parasite are detected in the peripheral blood when the disease has a severe malignant course. Parasitemia increases faster than with infection by other types of pathogens. Gametocytes of P. falciparum mature slowly, but live a long time (up to 6 weeks), while gametocytes of other species die several hours after their maturation. Gametocytes detected in tropical malaria help to determine the period of the disease: in the early period (with an uncomplicated course), only ring-shaped trophozoites are detected, during the peak period - rings and gametocytes (with primary infection in the absence of treatment, this indicates that malaria lasts at least 10-12 days); in the recovery period, only gametocytes are found. During treatment, the level of parasitemia in the peripheral blood is determined in dynamics. A day after the start of etiotropic treatment, it should decrease by 25% or more, and on the 3rd day it should not exceed 25% of the original. The presence of parasites in the blood preparation on the 4th day after the start of treatment, subject to all the conditions for successful treatment, is a sign of the pathogen's resistance to the drug used.
In recent years, rapid tests (immunochromatographic methods) based on the detection of the specific protein HRP-2a and the enzyme pLDH of P. falciparum have been used in endemic foci to quickly obtain a preliminary answer. Tests of one of the well-known rapid tests KAT-PF (KAT MEDICAL, South Africa) have shown high efficiency and specificity with respect to P. falciparum. Comparison of the results of the rapid test, microscopy and PCR showed that its diagnostic efficiency reaches 95-98%. The use of rapid tests allows you to find out the result in just 10 minutes. Laboratory personnel can master the reaction in 1-2 hours. Rapid methods make it possible for people living or traveling in endemic regions to carry out self-diagnosis; they can be carried out in the field. In Russia, rapid diagnostics of malaria is currently limited to individual clinical studies.
In modern conditions, especially in mass studies, the PCR method based on detection of malaria parasite DNA is of particular importance. The method can be used to determine carriage at low parasitemia and mixed infection with different types of plasmodia, as well as to differentiate relapse of drug-resistant falciparum malaria from reinfection with P. falciparum. Currently, it is used mainly in epidemiological studies.
What tests are needed?
Differential diagnosis
Differential diagnostic search for malaria is carried out depending on the severity of clinical manifestations of the disease and its duration. First of all, malaria is differentiated from diseases that occur with prolonged fever, enlargement of the liver, spleen, and possible development of anemia: typhoid fever and paratyphoid fever, brucellosis, leptospirosis, sepsis, lymphogranulomatosis. In the first 5 days from the onset of the disease, a common erroneous diagnosis for malaria in non-endemic regions is influenza (or other acute respiratory viral infections).
In tropical countries of South America, Africa, Southeast Asia, and India, differential diagnosis of malaria with hemorrhagic viral fevers (yellow fever, dengue fever, etc.) is carried out.
In the cerebral form of malaria-falciparum, differential diagnostics of malaria is carried out with encephalopathy (coma) developing with decompensated diabetes mellitus, liver and kidney failure, as well as edema and swelling of the brain with meningitis or meningoencephalitis of bacterial or viral etiology.
Who to contact?
Treatment malaria
Treatment of malaria includes stopping acute attacks of the disease, preventing relapses and gamete carriage, and restoring impaired body functions.
Antimalarial drugs are divided into the following groups depending on their effect on a particular stage of parasite development: hematoschizotropic agents, effective against asexual erythrocyte stages of plasmodia; histoschizotropic agents, effective against asexual tissue stages of plasmodia; gamotropic drugs, causing the death of gametocytes in the patient's blood or disrupting the maturation of gamemonts and the formation of sporozoites in the mosquito's body.
Etiotropic treatment
Etiotropic treatment of malaria in patients with malaria should be prescribed immediately after establishing a clinical and epidemiological diagnosis and taking blood for parasitological examination.
The drugs currently used belong to six groups of chemical compounds: 4-aminoquinolines (chloroquine - delagyl, chloroquine phosphate, nivaquine), quinolinemethanols (quinine - quinine dihydrochloride, quinine sulfate, quinimax, mefloquine), phenanthrenemethanols (halfan, halofantrine), artemisinin derivatives (artesunate, artemether, arteether), antimetabolites (proguanil), 8-aminoquinolines (primaquine, tafenoquine). In addition, combined antimalarial drugs are used: savarin (chloroquine + proguanil), malarone (atovaquone + proguanil), coartem or riamet (artemether + lumefantrine).
If P. vivax, P. ovale or P. malariae are detected in the patient, drugs from the 4-aminoquinoline group are used, most often chloroquine (delagyl). Treatment of malaria is as follows: the first two days the drug is used in a daily dose of 10 mg/kg of the base (four delagyl tablets at a time), on the 3rd day - 5 mg/kg (two delagyl tablets) once. There are isolated reports of resistance of P. vivax strains to chloroquine in Burma, Indonesia, Papua New Guinea and Vanuatu. In such cases, treatment should be carried out with mefloquine or quinine according to the treatment regimen for uncomplicated malaria. Attacks stop after 24-48 hours, and parasites disappear from the blood 48-72 hours after the start of chloroquine intake.
For radical cure (prevention of remote relapses) of malaria caused by P. vivax or P. ovale, after the end of the chloroquine course, a tissue schizontocide, primaquine, is used. It is taken for 14 days at a dose of 0.25 mg/kg (base) per day. P. vivax strains resistant to primaquine (the so-called Chesson-type strains) are found on the Pacific islands and in the countries of Southeast Asia. In these cases, one of the recommended regimens is taking primaquine at a dose of 0.25 mg/kg per day for 21 days.
If P. falciparum is detected in the blood of non-immune individuals in mild cases, the drugs of choice, according to WHO recommendations, are mefloquine and artemisinin derivatives (artemether, artesunate, arteether); halofantrine can also be used. In the absence of mefloquine and halofantrine and/or in the presence of contraindications to the use of these drugs, quinine is prescribed in combination with antibiotics (tetracycline, doxycycline). Tetracycline is taken 0.5 g twice a day for 7-10 days; it can be replaced with doxycycline in a daily dose of 0.1 g, the duration of administration is 7-10 days. In regions where P. falciparum is resistant to mefloquine and quinine, a combination of mefloquine and artemisinin preparations (artes}nate, artemether) is recommended for the treatment of uncomplicated tropical malaria. A combination of fansidar and artesunate is effective in treating uncomplicated tropical malaria. Artemisinin preparations are widely used to treat multidrug-resistant tropical malaria in Southeast Asia, a number of countries in South America and Africa. They act very quickly on both the blood stages and gametocytes. However, these drugs are quickly eliminated from the body, which is why malaria relapses occur. It is more appropriate to prescribe them in combination with mefloquine in the following doses:
- artesunate: 4 mg/kg twice daily for 3 days; mefloquine: 15 mg/kg once on day 2 or 25 mg/kg in two doses on days 2 and 3;
- artemether: 3.2 mg/kg once daily for 3 days; mefloquine: 15 mg/kg once on day 2 or 25 mg/kg in two doses on days 2 and 3.
Treatment regimens for uncomplicated malaria
Application schemes |
|||
Preparation |
First dose, mg/kg |
Subsequent doses, mg/kg (interval, h) |
Course duration, days |
Chloroquine |
10 (grounds) |
10- 1-2 day 5 - 3 day |
3 |
Fansidar (sulfadoxine + pyrimethamine) |
2.50-1.25 |
- |
1 |
Quinine, Kinimax, Kinoform |
10 (grounds) |
7.5 (8) |
7-10 |
Mefloquine |
15 (grounds) |
- |
1 |
Halofantrine |
8 (salt) |
8 (6) |
1 |
Artesunate |
4 |
2 (12) |
7 |
Artemether |
3.2 |
1.6 (24) |
7.0 |
Quinine -tetracycline |
10.0-1.5 |
10.0 (8)+5.0 (6) |
10.0+7.0 |
Coartem (artemether + lumefantrine) |
1.3+8 0 |
1.3-8.0 (8) |
3.0 |
When the type of pathogen is not established, treatment is recommended to be carried out according to the treatment regimens for tropical malaria. If the patient vomits earlier than 30 minutes after taking the prescribed antimalarial drug, the same dose should be taken again. If vomiting occurs 30-60 minutes after taking the tablets, then half the dose of this drug is additionally prescribed.
Patients with severe tropical malaria should be hospitalized in an intensive care unit or resuscitation department. Quinine remains the drug of choice for the treatment of severe tropical malaria. When treating complicated forms (cerebral malaria, algid), the first dose (7 mg/kg) of quinine base is administered intravenously over 30 minutes. Then another 10 mg/kg is administered intravenously by drip over 4 hours. Thus, the patient receives 17 mg/kg of quinine base over the first 4.5 hours after the start of treatment. According to another scheme, the initial dose of 20 mg/kg of quinine base is administered over 4 hours. Both schemes are tolerated satisfactorily by patients - without cardiovascular or other disorders. A maintenance dose of 10 mg/kg of quinine base is administered at 8-hour intervals, the duration of administration is 1.5-2 hours. It is advisable to combine quinine with tetracycline (250 mg four times a day for 7 days) or doxycycline (0.1 g per day for 7-10 days). For the treatment of children, it is recommended to administer a loading dose (15 mg/kg) of quinine base intravenously by drip in a 5% glucose solution for 4 hours. A maintenance dose (10 mg/kg) is administered for 2 hours at 12-hour intervals. The same dose is used for intramuscular administration, but quinine is recommended to be diluted five times in distilled water and divided into two injections in different buttocks.
Artemether is used as an alternative drug for the treatment of complicated tropical malaria at a daily dose of 3.2 mg/kg on the first day of treatment. In the following six days, it is administered at a dose of 1.6 mg/kg intramuscularly in combination with one dose of mefloquine.
Patients with severe and complicated forms of malaria are prescribed intensive pathogenetic therapy. When performing rehydration, one should be wary of pulmonary and cerebral edema, but hypovolemia is no less dangerous. If rehydration is unsuccessful, such patients may experience tissue perfusion insufficiency, acidosis, hypotension, shock, and renal failure. Developing anemia is usually not life-threatening, but if the hematocrit is reduced to 15-20%, then red blood cells or whole blood should be transfused. Transfusion of fresh whole blood or concentrates of coagulation factors and platelets is used in DIC syndrome. In case of hypoglycemia, intravenous administration of a 40% glucose solution should be used.
The basis of treatment for cerebral edema is detoxification, dehydration, control of cerebral hypoxia and respiratory disorders (oxygen therapy, artificial ventilation). Anticonvulsants are administered as indicated. Experience in treating cerebral malaria has proven the ineffectiveness and even danger of using osmotic diuretics: low molecular weight dextrans; adrenaline; prostacyclin; pentoxifylline; cyclosporine; hyperimmune serums. Hyperbaric oxygenation is also not recommended.
In the case of acute renal failure or acute renal-hepatic failure, the daily dose of quinine should be reduced to 10 mg/kg due to possible drug accumulation and solutions should be administered at a rate of 20 drops per minute. In the initial period of acute renal failure, forced diuresis is performed, and if there is no effect and azotemia increases, hemodialysis or peritoneal dialysis is used, which usually gives good results. In the case of hemoglobinuric fever, the drug that caused hemolysis is discontinued. If necessary, it is replaced with other antimalarial drugs, and glucocorticosteroids (prednisolone 1-2 mg/kg) and detoxification therapy are prescribed at the same time.
In case of spleen rupture, which usually develops in cases of rapid and significant enlargement of the organ, emergency surgical intervention is indicated.
To treat relapses of tropical malaria, a previously unused drug is selected or the previous one is used, but in combination with other antimalarial drugs. Gamete carriage is eliminated with primaquine for 1-3 days in normal therapeutic doses.
The effectiveness of malaria treatment is monitored by examining a thick blood drop with a parasitemia count in 1 μl. These studies are performed daily from the 1st to the 7th day after the start of etiotropic treatment. If the parasites disappear during this time, further studies of blood preparations are performed on the 14th, 21st and 28th days after the start of treatment.
Evaluation of effectiveness
The effectiveness of etiotropic treatment of malaria in patients with malaria is assessed by three parameters: early failure (EF), late failure (LF) and effective treatment.
After taking an antimalarial drug, the patient may vomit (especially in children). It is important to remember that if vomiting occurs less than 30 minutes after taking the drug, the same dose should be taken again, and after 30-60 minutes - half the dose of the drug used.
Evaluation of the effectiveness of malaria treatment (WHO, 1996)
Early failure (EF) |
Worsening or persistence of clinical signs of malaria in the presence of parasitemia during the first 3 days from the start of specific therapy |
Late failure (LF) |
Reappearance of characteristic clinical signs of malaria (including the development of a severe condition) in the presence of parasitemia from the 4th to the 14th day from the start of specific therapy |
Treatment effectiveness |
Absence of parasitemia after 14 days from the start of specific therapy in the absence of RN and PN criteria |
Radical treatment of malaria
Radical treatment of malaria is carried out simultaneously with arresting treatment or immediately after it.
- For the prevention of exoerythrocytic relapses of vivax malaria and ovale malaria, in order to affect hyptozoites, primaquine is prescribed at 45 mg (27 mg of base) per day (3 tablets) - a course of 14 days or 6 tablets - 1 time per week - 6-8 weeks (in case of glucose-6-phosphate dehydrogenase deficiency). The drug tafenoquine is undergoing clinical trials - an analogue of primaquine, but with higher clinical efficacy and a lower frequency of side effects.
- To prevent the transmission of falciparum malaria (by affecting gametocytes), primaquine is used at 45 mg (27 mg of base) per day (3 tablets) - 3 days. Treatment is carried out in regions endemic for tropical malaria. When using Fansidar in the treatment of patients who have had falciparum malaria, primaquine is not prescribed due to the effective effect of pyrimethamine, which is part of Fansidar, on Pl. falciparum gametocytes.
Treatment of severe and/or complicated falciparum malaria is carried out in intensive care units. If oral administration of medications is not possible, parenteral therapy is carried out with one of the following medications:
- quinine dihydrochloride - 10-20 mg/kg (up to 2.0 g per day) intravenously in 500 ml of 5% glucose solution, slowly, 2-3 times per day until the patient recovers from a serious condition, then one of the oral drugs according to the treatment regimen for uncomplicated falciparum malaria;
- In modern conditions, new herbal preparations are used in some countries to treat severe forms of falciparum malaria (these preparations are not certified in Russia): Artemether (Artenam) - 160 mg intramuscularly on the first day, then 80 mg for 6 days; Artesunate - 50 mg intramuscularly (intravenously) 2 times a day for 7 days; Artemisinine - 1200 mg intramuscularly for 7 days.
The pathogenetic treatment of malaria depends on the severity of malaria and the development of complications. Detoxification therapy, correction of metabolic acidosis, hypoglycemia, diuretics, antihistamines, glucocorticosteroids (as indicated), vitamins, cardiovascular and other drugs are prescribed. In case of anuria, peritoneal dialysis can be performed. In the treatment of hemoglobinuric fever, first of all, the drugs that caused hemolysis are discontinued, and red blood cell mass transfusion is performed.
Convalescents are discharged after the completion of a full course of etiotropic parasitological treatment (stopping therapy) in the presence of 2-3 negative results of blood tests (thick drop). Patients who have had vivax malaria and ovale malaria can undergo a subsequent course of treatment with primaquine on an outpatient basis. Patients who have had malaria are monitored for 1-1.5 months with repeated parasitological tests of a thick drop of blood every 7-10 days. Patients who have had vivax malaria, ovale malaria and malariae malaria are monitored for two years, with mandatory parasitological tests of a thick drop at any increase in temperature.
Prevention
WHO is combating malaria worldwide within the framework of the Roll Back Malaria Programme, adopted in 1998. Currently, WHO has set a new goal for the European Region - to eliminate three-day malaria (P. vivax) by 2010, and tropical malaria by 2015. The most important link in the complex of measures is the timely detection and treatment of sources of infection.
Preventive measures in the outbreak are aimed at timely detection and treatment of malaria, as well as parasite carriers (sources of infection), as well as combating malaria carriers. There are currently no effective vaccines for active immunization against malaria.
Individual malaria prophylaxis during stay in an endemic focus is aimed at preventing infection and preventing a malaria attack. Prevention of infection consists of taking measures to protect against mosquito bites (use of repellents, nets on windows and doors, bed curtains, clothing that covers the arms and legs when staying outdoors in the evening and at night). In accordance with WHO recommendations, prevention of a malaria attack consists of taking antimalarial drugs, it is recommended only for non-immune individuals traveling to foci with a high risk of malaria infection and lack of accessible medical care (remoteness of medical institutions, impossibility of rapid blood testing for malaria).
The need for use, duration and frequency of taking the drugs is determined only after consultation with an infectious disease specialist. It is important to identify contraindications for taking chemotherapy drugs, the presence of severe concomitant diseases. Pregnant non-immune women, young children should not visit regions endemic for malaria.
Given the high resistance of Pl. falciparum to chloroquine, the standard for the prevention of falciparum malaria, as recommended by WHO, is currently mefloquine (250 mg once a week, 2 weeks before leaving for an endemic region and for 4 weeks after returning). The use of other drugs (doxycycline, chloroquine in combination with proguanil, atovaquine in combination with proguanil, primaquine and others) is determined by an infectious disease specialist taking into account the epidemiological situation in the region of stay and other above-mentioned factors.
Forecast
In most cases, mortality is caused by tropical malaria, or more precisely, its cerebral form, which occurs in 10% of cases of severe falciparum malaria. Fatal outcomes from other types of malaria are very rare. But tropical malaria, with timely diagnosis and proper treatment of malaria, ends in complete recovery.
For patients who have had tropical malaria, it is recommended to establish dispensary observation for 1-1.5 months and conduct parasitological blood tests at intervals of 1-2 weeks. Dispensary observation of patients who have had malaria caused by P. vivax. P. ovale. P. malariae should be carried out for two years. Any increase in body temperature requires laboratory blood testing to promptly identify malarial plasmodia.

