Medical expert of the article
New publications
Diaper dermatitis in a newborn: what does it look like and how to treat?
Last reviewed: 04.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
Many parents face such a problem as diaper dermatitis in children in the first year of life, that is, inflammation of the skin of the buttocks and folds of the groin area.
This is what is commonly called diaper rash, but in fact, it is its consequence - diaper erythema or rash. And if, according to ICD-10, the code for diaper dermatitis is L22, then the code for erythematous diaper rash is L30.4.
Epidemiology
Mild diaper dermatitis develops in almost half of children from birth to one year of age, and it accounts for at least 20-25% of all diagnosed dermatitis among children of this age.
This skin lesion, as noted by domestic pediatricians, most often occurs in infants after six to seven months. However, as practice shows, diaper erythema with a rash in the perianal area can also develop in newborns - that is, at the age of one to two months.
Causes diaper dermatitis
Dermatologists cite the following main causes of diaper dermatitis in infants: prolonged over-moistening of the skin (in conditions of lack of air access) and its constant contact with urine containing salts, uric and hippuric acids, as well as urea, which is broken down with the release of ammonia. Fecal enzymes also cause irritation, and bacteria, usually present in feces, can increase the breakdown of urea due to the urease they secrete, which leads to an alkaline pH, which further irritates the skin.
Irritation also occurs due to mechanical damage to the integumentary epithelium when the skin is rubbed by diapers or clothing (especially synthetic).
Risk factors
Risk factors for the development of diaper rash in the groin and buttocks and the development of diaper dermatitis include untimely changes of wet diapers and violation of basic hygiene rules when caring for the baby's skin after urination and bowel movements. Intestinal upset with diarrhea also increases the risk of skin irritation in this area.
In addition, children who are fed with formula-based substitutes for breast milk develop diaper dermatitis more often due to the higher enzyme content in their stool. Although, as is known, the acidity of stool during breastfeeding is significantly higher than during artificial feeding, and its frequency in the neonatal period is twice as high as the number of bowel movements in artificially fed infants.
Diaper dermatitis in adults – contact urinary dermatitis – occurs in bedridden patients (especially the elderly) with loss of control over urination and defecation.
 [ 9 ]
[ 9 ]
Pathogenesis
The pathogenesis of diaper dermatitis in infants is explained very simply: at this age, the child's skin is not yet able to withstand external aggressive influences due to the weakness of the protective functions of the epidermis.
In the first months of life, the baby's skin and its stratum corneum are very thin and have increased hydrophilicity; the density of the epidermis is insufficient due to the lack of a strong connection with the dermis. The process of formation of the basal membrane of the epidermis continues over the loose subcutaneous tissue, which contains a lot of moisture, but almost no collagen and elastin fibers. And the sebaceous glands of the skin - despite their sufficient number and development - do not yet provide a fatty protective barrier (hydrolipid mantle) of the skin of the body.
In addition, the acid mantle of the skin is also absent, since instead of the skin pH at 5.5, the skin of a baby during the first two months after birth fluctuates between 6.2-6.8. All this determines the vulnerability of the skin of children under one year to various irritating factors.
Symptoms diaper dermatitis
The first signs of skin irritation are its redness (erythema), which can be continuous or patchy, localized in the area of the buttocks and groin, on the inner thighs and around the external genitalia.
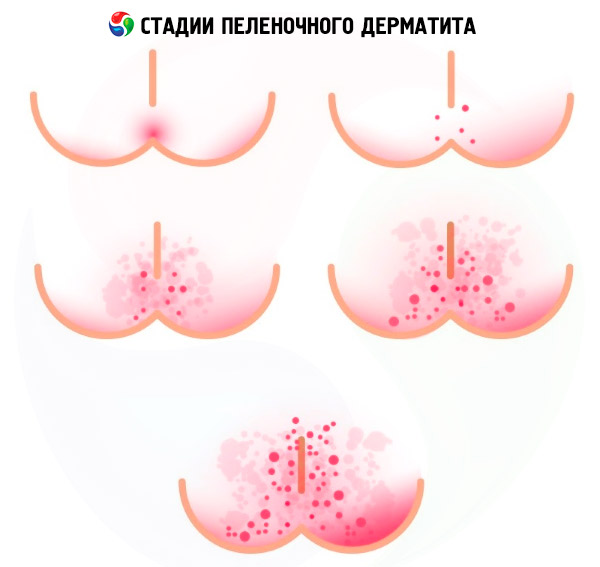
If the process does not go beyond the first stage of the inflammatory reaction of the skin (thanks to the measures taken), then this is considered a mild form of diaper dermatitis. But this pathology has two more stages (forms).
Symptoms of stage two diaper dermatitis (moderate form) are manifested by more intense redness and rashes in the form of small papules or pustules with exudate. When their integrity is compromised and exudate and intercellular fluid are released, weeping (maceration zones) and small focal erosions appear.
The third stage (severe form) of the inflammatory process is considered to be a significant expansion of the affected areas and the appearance of edema and hemorrhagic ulcers. Some dermatologists call this form erosive diaper dermatitis of Jacquet.
In addition to skin symptoms, the child is bothered by itching, which manifests itself in anxiety, crying, sleep and feeding disturbances.
In principle, diaper dermatitis in adults manifests itself with the same skin symptoms.
Complications and consequences
Diaper erythema can easily be accompanied by any infection - bacterial or fungal. If the affected areas of the child's skin are infected with streptococci or staphylococci, then a complication such as bacterial diaper dermatitis develops, which is characterized by a subfebrile body temperature, as well as the formation of purulent pustules, and then purulent crusts and extensive erosions, that is, the development of a clinical picture of staphylococcal (bullous) impetigo.
And when the skin is affected by the Candida fungus, and the skin around the affected areas begins to peel, candidal diaper dermatitis is diagnosed. In both cases, antibacterial or antifungal therapy will be required.
Differential diagnosis
Differential diagnostics aims to distinguish diaper dermatitis from allergic dermatitis, such as diaper allergy or atopic dermatitis; bullous impetigo; perianal streptococcal dermatitis (which may occur with diarrhea in newborns); enteropathic acrodermatitis (caused by congenital zinc deficiency in the body), congenital syphilis, etc.
Who to contact?
Treatment diaper dermatitis
Treatment for diaper dermatitis should be prescribed by a doctor, since it depends on the stage (form) of the pathology. The main components of therapy are compliance with the rules of hygienic care. Thus, with a mild form of diaper erythema, it is enough to change wet and dirty diapers in a timely manner and wash the groin and gluteal area of the body with warm water and baby soap after each urination or bowel movement, and then dry it well by blotting. Pediatricians also advise leaving the child naked for several minutes (at a room temperature of at least + 22-25 ° C): such air baths ensure the evaporation of residual moisture from the skin (especially from the folds in the groin and on the inner thighs). Dry skin should be lubricated with mineral or vegetable oil. The following oils are recommended for diaper dermatitis: Vaseline, stone (almond), sea buckthorn. You can also use baby cream with chamomile or string extract.
To dry out wet areas of the skin, it is common practice to use powders for diaper dermatitis, which contain zinc oxide: it not only dries the skin, but also fights infection. For the same purpose, brilliant green is traditionally used for diaper dermatitis (once a day), as well as zinc ointment - two to three times a day.
But the cream Zinnovit (with zinc pyrithione and a derivative of glycyrrhizic acid) also contains exfoliating lactic acid and oils and is intended to combat pimples and acne. The product should not be used on children under one year of age.
One of the best remedies for getting rid of diaper erythema is a cream with dexpanthenol Bepanten (other trade names - Dexpanthenol, D-Panthenol, Pantestin, Pantoderm).
More information in the material - Ointments for diaper rash and in the article - Treatment of diaper rash in adults
An effective remedy is Sudocrem, which contains zinc oxide and benzyl compounds with antibacterial and antifungal properties. But this cream should not be used on wet skin, as a film forms after its application.
Topical medications with antibiotics and antifungal components are necessary if a bacterial or fungal infection joins the diaper dermatitis. And they are used only as prescribed by a dermatologist. For example, to treat candidal diaper dermatitis, it is best to use 1% Clotrimazole cream (Lotrimin, Oronazole), which is applied to the affected areas of the skin three times a day until the rash disappears, and then for at least another two weeks - once a day.
Bacterial diaper dermatitis is successfully treated with Levomekol ointment (with chloramphenicol and methyluracil) - once or twice a day. The drug Baneocin - thanks to the presence of antibiotics neomycin and bacitracin, copes well with weeping skin inflammations. But neomycin, absorbed into the skin of an infant, can cause a toxic effect on the kidneys and reduce hearing. Therefore, even adults cannot apply it to large areas of skin. The same applies to Baneocin in powder form, which is used as a dusting powder for bacterial diaper dermatitis in adults.
The active ingredients in Pimafukort ointment are the antibiotics neomycin and natamycin, as well as hydrocortisone. Hydrocortisone is well absorbed by the skin, and in small children the degree of absorption is even higher, which increases the risk of its negative systemic effects in the form of decreased pituitary and adrenal function, the development of hypercorticism, the removal of calcium from the body and growth retardation. The use of GCS can lead not only to the development of reactive dermatosis, disruption of skin trophism and its atrophy, but also to the activation of infection. In addition, the ointment contains neomycin, the side effects of which have already been discussed earlier. This ointment, according to the official instructions, is not prescribed to children under one year.
Triderm ointment contains a potent corticosteroid betamethasone (relieves inflammation and itching), an antibiotic gentamicin and clotrimazole, which is effective against candidal infection. Its contraindications include dermatoses (including diaper dermatosis) in children in their first year of life.
Akriderm ointment, in addition to betamethasone, contains the antibiotic gentamicin and is contraindicated for children under one year of age.
Advantan (0.1% ointment, cream, emulsion) also refers to topical corticosteroids, since its active ingredient is the potent GCS methylprednisolone. But, as indicated in the instructions, its use (once a day) in children with diaper dermatitis without maceration is permissible - after four months.
It should be borne in mind that foreign pediatricians do not prescribe corticosteroids to children under two years of age. Our doctors consider it possible for children under one year to use 1% hydrocortisone externally, but on small areas of skin.
Folk remedies
Folk remedies for treating diaper dermatitis include a decoction of bay leaf (two leaves per 200 ml of water, boil for about 10 minutes), which is used to treat the affected areas. Infusions or decoctions of oak bark and birch leaves are suitable in such cases.
Also, with slight hyperemia of the skin, you can carry out herbal treatment: wash the buttocks and groin folds with decoctions of chamomile, succession, sage, calendula, plantain (two to three tablespoons of dry plant per liter of water).
There is an undeniable benefit to bathing infants with herbal infusions added to the bath, and this is a simple and proven physiotherapeutic treatment at home.
Forecast
Parents should not worry: the prognosis for the development of diaper dermatitis is favorable and does not pose a threat to the baby’s health.
 [ 29 ]
[ 29 ]


