Medical expert of the article
New publications
Bleeding navel in a newborn: causes
Last reviewed: 04.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
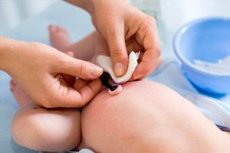
If a newborn's belly button is bleeding, this is a common cause for concern for parents. In some cases, this can really be a serious pathology, but sometimes it is just a long-healing belly button. Parents should definitely know when the symptoms indicate a disease and when they need to see a doctor immediately.
Causes umbilical discharge in a newborn baby
Why does a newborn's belly button bleed? Many parents have this problem after being discharged from the hospital, and it raises many questions and concerns. But this does not always indicate a disease, sometimes it is just the peculiarities of the umbilical wound healing. When should you not worry? Children born physiologically without complications are discharged from the hospital after three days. As a rule, the umbilical wound of most babies is already starting to heal and is dry, and in some it even falls off before three days. But it also often happens that when caring for the umbilical wound, it can be damaged or just when bathing, the navel is slightly touched. In this case, it can bleed a little, which is a normal reaction to an unhealed wound. How long does a newborn's belly button bleed? It should be dry and clean, and within five to fifteen days it should heal and fall off. This is the period considered normal for those cases when it can bleed. If it lasts longer, then you should definitely consult a doctor.
What other reasons are there for the navel to bleed? The most common cause is hemorrhagic disease of the newborn. The pathogenesis of the disease lies in the peculiarities of the child's body in relation to the hemostasis system. These features include functional deficiency of platelets, which can be the basis for the development of hemorrhagic conditions in newborns. In addition, attention should be paid to the reduced concentration of individual blood clotting factors in newborns - II, VII, IX, X, XI, XII, antithrombin and plasminogen. All these features are also characteristic of the hemostasis system of premature infants. Physiological deficiency of platelets or plasma clotting factors can become pathological and lead to the development of hemorrhagic disease of the newborn. There are some features of the child's body that contribute to the development of blood clotting disorders. A slight decrease in factors II, VII, IX, X is observed in children in the first three days after birth. But this deficiency is not constant, by the end of the first week of life the child can restore all the deficient factors. The body of a pregnant woman also has a deficiency of vitamin K, which affects the formation of blood clots and reduces the rate of blood clotting in a newborn baby. In a small number of newborns (2-5% of all children), the level of K-vitamin-dependent blood clotting factors may be lower, which is one of the reasons for the development of bleeding. This may be due to the prescription of indirect anticoagulants, anticonvulsants, acetylsalicylic acid to the pregnant woman, as well as the pathological condition and toxicosis of the pregnant woman against the background of low estrogen levels, impaired formation or absorption of vitamin K in the mother's intestine. Breast milk in the first days of life cannot compensate for the deficiency of vitamin K, since it is available in small quantities. Therefore, it is important to populate the child's intestines with normal microflora, which produces this vitamin, in eliminating this deficiency. This is why the deficiency of K-vitamin-dependent factors is eliminated in children by the end of the 2nd week of pregnancy. And one of the most common and early symptoms of this disease is the symptom when the navel begins to bleed.
Another reason may be other forms of hemorrhagic diseases. Hereditary forms of hemorrhagic diseases of newborns may be caused by both a disorder of platelet function and a decrease in the concentration of individual plasma coagulation factors. Hereditary hemorrhages of platelet nature - thrombocytopenic purpura. Hemorrhages occur only in cases of its most severe forms: umbilical hemorrhage, cerebral hemorrhage. Congenital hypoplastic thrombocytopenia may also sometimes occur.
Hereditary hemorrhages of coagulation nature are severe forms of hereditary deficiencies of plasma coagulation factors V, VII, VIII, IX, X, XI, XII, the deficiency of which may cause hemorrhagic phenomena leading to the death of newborns. The cause of death in newborns is hemorrhage in the brain, profuse gastrointestinal bleeding, hemorrhage from the umbilical cord. With an insufficient amount of plasma factor XIII, newborns may experience "umbilical syndrome" - slow closure of the umbilical wound and bleeding from it within 2-3 weeks of life. With an insufficient amount of this factor, newborns often experience hemorrhages in the gastrointestinal tract, brain and its membranes. The majority of hemorrhagic conditions in newborns are acquired forms. Some of them are associated with a violation of the function of platelets, others are of a coagulation nature.
Secondary vitamin K deficiency hemorrhagic syndrome: occurs in children with mechanical jaundice (atresia of the bile ducts and bile ducts, bile thickening syndrome), enteropathy, intestinal dysbacteriosis; associated with impaired absorption of fat-soluble phylloquinones.
DIC syndrome in newborns can occur in various pathological conditions, signifies a severe catastrophe. It can be the cause of serious bleeding from the navel. In this case, pronounced blood clotting is observed, which closes the vessels with loose masses of fibrin and blood cell aggregates, and then, having exhausted the supply of procoagulants, the ability to clot disappears, leading to profuse bleeding. Causes of DIC syndrome: septicemia, late toxicosis of pregnancy in the mother, physiological immaturity of the reticuloendothelial system in the fetus, asphyxia, acidosis, hypothermia, traumatic injuries during childbirth, etc.
The main phases of development: hypercoagulation and blood clotting already begins inside the vessels, as well as hypocoagulation. In general, DIC syndrome is largely associated with damage and disruption of blood flow in small vessels due to platelet aggregation, blockage of vessels with blood cells, disruption of cellular respiration and acidosis, and platelet pathology. In DIC syndromes of various genesis, the mechanism of bleeding formation is not the same: in some forms, platelet-microcirculatory disorders come to the fore, in others - coagulation shifts, in the third case - disorders in all links of hemostasis. Hemorrhages are caused by the consumption of coagulation factors, blockade of fibrinogen, platelets by fibrin degradation products, fibrinogen, increased vascular permeability due to hypoxia, activation of the kinin system, a decrease in the number and function of platelets.
Risk factors
Risk factors for developing belly button problems include:
- Premature babies are more likely to develop hemorrhagic disease;
- unfavorable obstetric history: long-term infertility, somatic diseases, extragenital pathology;
- pathological course, pregnancy threat of termination, urogenital diseases, acute respiratory viral infections, exacerbation of chronic foci, prolonged hypoxia;
- obstetric interventions, endometritis during childbirth;
- artificial feeding from the first days;
- children with hereditary pathologies of the hemorrhagic system;
- Skin infections in children increase the risk of belly button infection;
- congenital immunodeficiencies and HIV infection;
- congenital pathologies of the gastrointestinal tract.
All these risk factors should be taken into account by the pediatrician first of all, warning parents about the consequences and possible pathologies.
 [ 3 ]
[ 3 ]
Symptoms umbilical discharge in a newborn baby
If we are talking about simple trauma and the newborn's navel bleeds after bathing, then the first signs may be a small amount of blood. This usually ends with the blood clotting after a few minutes and everything goes away. After this, the navel remains dry again with small bloody masses around. If this does not happen again, there are no other manifestations of pathology and an increase in body temperature, then this is a normal phenomenon and over time the navel will tighten and heal.
When a newborn's navel bleeds and purulently or the navel is wet and bleeding, this is already a very serious cause for concern. In this case, we are talking about infection and inflammation with the development of omphalitis. This is an inflammation of the skin and tissue around the navel caused by bacterial flora. For newborns, this is a particularly dangerous condition, since children are often discharged home and their umbilical wound has not yet healed, or the navel has not fallen off at all. This can be a gateway for infection, which spreads very quickly here. Clinically, against the background of an increase in body temperature, you can see that fluid begins to come out of the navel or it turns red. If the navel of a newborn bleeds and smells, then this can also be regarded as a symptom of omphalitis.
Hemorrhagic disease of the newborn can very often manifest itself as a problem with the navel, since this is a weak spot in a newborn that has not yet fully healed. Therefore, if the navel is bleeding, especially in a premature baby, then you need to think about it. A characteristic symptom of this disease is bleeding from other organs - the stomach, intestines, hemorrhage in the brain. Therefore, if there is bleeding from the navel and another source of bleeding, then there is a high probability that the child may develop late hemorrhagic disease of the newborn.
Hereditary thrombocytopathy, in addition to causing bleeding from the navel, may also be accompanied by skin manifestations of hemorrhagic rash.
Symptoms of acute DIC syndrome are characterized by acute dysfunction and dystrophy of internal organs, hemocoagulation shock (syndrome), thromboembolism and hemorrhagic syndrome. Thromboembolic syndrome is observed in chronic, subacute, acute DIC syndrome with clinical manifestations of venous, arterial thromboses caused by vascular wall defects (in children - infectious-toxic, immune-allergic vascular lesions).
Hemorrhagic manifestations (local or widespread) develop in the hypocoagulation phase of acute DIC syndrome. Local bleeding is when the navel bleeds, which can be one of the first symptoms. Widespread hemorrhages are caused by local disorders: hematomas, petechiae on the skin, in the subcutaneous tissue, hemorrhages in the brain, meninges, heart, pericardium, lungs, pleura, peritoneum, gastrointestinal, renal, hepatic bleeding. If bleeding occurs from all possible places and blood clots form in parallel, then this is a sign of DIC syndrome.
These are the main symptoms that may occur along with the appearance of bloody discharge from the navel.
Diagnostics umbilical discharge in a newborn baby
Diagnostics should first of all exclude serious diseases that may be accompanied by this symptom. If the navel is bleeding and there are no other symptoms, then there is no need for invasive interventions or laboratory tests. When the body temperature rises or there are some purulent discharges from the navel along with bloody ones, then it is necessary to exclude infectious complications. A blood test can show inflammatory changes, which will be manifested by an increase in ESR, an increase in the number of band leukocytes.
For a more complete diagnosis, when studying the anamnesis, it is necessary to pay attention to the absence of bleeding in relatives and the normal course of pregnancy and childbirth in the mother. If there are no manifestations on the skin of relatives, then it is necessary to study the coagulogram.
In case of pathology in the coagulogram, prothrombin time, blood clotting time and plasma recalcification are increased, and the level of prothrombin and factors IX, X are significantly reduced. Bleeding time, the level of factors V and VIII, the number of platelets, the fragility of the vascular wall and the time of clot retraction remain normal, taking into account the age and maturity of the newborn. These studies exclude hemorrhagic diseases - almost all hereditary thrombocytopenia and DIC syndrome.
Instrumental diagnostics are rarely necessary, since all problems can be identified using laboratory indicators. Sometimes, if there is a suspicion of hemorrhage in organs or the brain, there may be a need for ultrasound diagnostics or ultrasonography of the brain.
 [ 8 ]
[ 8 ]
Differential diagnosis
Differential diagnostics should first of all exclude complex pathologies that threaten the child's life due to bleeding. If the navel of a newborn boy is bleeding, then differential diagnostics should be carried out with hemophilia. This hereditary disease can only manifest itself in boys. In addition to blood discharge from the navel, it is accompanied by large hemorrhages in the brain, joints, and bleeding into parenchymatous organs. The bleeding does not stop on its own.
Who to contact?
Treatment umbilical discharge in a newborn baby
The approach to treatment depends on what is causing the symptoms. What should you do if a newborn's belly button is bleeding? First of all, you should not apply anything before consulting a doctor and you should not rinse it with water. If there is no purulent or mucous discharge and the belly button is bleeding because it has not yet healed, then you just need to treat it correctly. How to treat a newborn's belly button if it is bleeding? The most common and safe remedy is considered to be brilliant green. It has antiseptic properties and is able to kill pathogenic flora. To treat the belly button, you need to wash your hands well and treat them with an antiseptic. After that, lubricate a cotton swab in the solution and open the umbilical wound with two fingers and lubricate it well with brilliant green. As a rule, one time is enough for all problems with the belly button to go away.
When it comes to hemorrhagic pathologies or DIC syndrome, the treatment in this case is complex and includes many drugs.
Treatment of DIC syndrome is complicated by the multifactorial nature of its occurrence. The main direction should be its prevention - elimination of those factors that can cause it. List of drugs in the treatment of DIC syndrome: intravenous administration of heparin, disaggregants, protease and plasminogen inhibitors, blood substitutes, plasma therapy, thrombolytic therapy. The use of this or that drug will be effective only in case of correct assessment of the clinical situation, based on the basic laws of hemostasis and possible variants of disorders in newborns. Phyloquinones at the rate of 1 ml / kg of body weight twice a day for three days and two days - for premature babies. Feeding children with ground milk should be carried out with breast milk cooled to room temperature. They are prescribed a solution of thrombin and androxon in epsilon-aminocaproic acid (an ampoule of dry thrombin is dissolved in 50 ml of a 5% solution of epsilon-aminocaproic acid and 1 ml of a 0.025% solution of androxon is added) or a 0.5% solution of sodium bicarbonate, 1 teaspoon 3 times a day. For emergency hemostatic action and an increase in prothrombin complex factors, it is necessary to administer single-group fresh frozen plasma at a rate of 10-15 ml / kg with simultaneous intravenous administration of 3-5 mg of vikasol (vitamin K3), more effectively vitamin K1. Infusion therapy is carried out to maintain hemodynamics.
- Heparin is considered the main treatment for blood clotting disorders in the case of DIC syndrome. The mechanism of action of heparin is to promote thrombin inactivation by activating antithrombin III, suppresses VIIa, Χa, ΧIIa, ΧIIa blood clotting factors, as well as plasmin and kallikrein. Inhibits the activity of hyaluronidase, thereby reducing vascular permeability. The hypolipidemic effect of heparin is manifested by an increase in the activity of lipoprotein lipase. Suppresses the interaction of T- and B-lymphocytes (immunosuppressive effect). Inhibits platelet aggregation. Somewhat increases the fibrinolytic activity of the blood. Inhibits the proliferation of vascular wall SMC. Has anti-inflammatory and diuretic effects. Improves collateral circulation. Heparin is practically not absorbed in the gastrointestinal tract, is well absorbed with intravenous and subcutaneous administration. Does not penetrate the placental barrier. Binds to LP, less - to blood proteins. Heparin is metabolized in the liver, kidneys and connective tissue. It is excreted unchanged by the kidneys when administered intravenously. The dosage of the drug is 100 units per kilogram of the child's body weight, the method of administration is subcutaneous, every six hours. Side effects - can lead to hemorrhagic syndrome, allergic reactions, headache, arthralgia, myalgia, urticaria, skin itching, toxic diarrhea. In addition, heparin causes reverse alopecia, hypotension, osteoporosis, hypoaldosteronism, hematomas at the injection site, thrombocytopenia.
- Etamzilat is a hemostatic drug used for bleeding as a fast-acting drug. The drug promotes the formation of molecules that pass poorly through the vessels, which reduces bleeding. In addition, etamzilat has a hemostatic effect. The dosage of the drug is a 12.5% solution of 2 milliliters on glucose, the best method of administration is infusion drip.
- The use of antibiotics in the treatment of omphalitis, which is accompanied by bleeding from the navel, is mandatory.
Ceftibuten is an oral cephalosporin of the third generation, which does not die in the presence of bacteria that contain lactamases. The drug is well absorbed when taken orally and is immediately divided into fractions, circulating in the blood throughout the day. The mechanism of action of cefbuten is the activation of enzymes that promote the destruction of the bacterial wall and the release of bacterial endotoxin (disruption of the synthesis of polysaccharides in the cell wall of the microorganism). All this together ensures the death of the pathogen in omphalitis and prevents the development of further infection. Dosage - 9 mg / kg for children.
Considering that the approach to treatment is very differentiated, it is very difficult to analyze all the drugs necessary for treating a child with complex symptoms of DIC syndrome. Therefore, only the main principles of treatment with a mandatory individual approach are taken into account.
Folk remedies
Traditional methods of treatment can be used if the navel is simply bleeding and does not heal for a long time. Parents often wonder whether it is possible to bathe a newborn if the navel is bleeding? Bathing is a hygienic procedure that should be carried out in any case, especially if there are problems with the navel. You cannot bathe only if there are signs of inflammation or redness. In other cases, you can bathe the child and use anti-inflammatory herbs.
- The herb of succession and chamomile cleanses the baby's skin very well and has antiseptic properties. To brew, take one hundred grams of succession herb and one hundred grams of chamomile and pour hot water over them. Let it brew for twenty minutes, then add it to a warm bath before bathing. Rubbing the navel area or intensively washing with soap and a washcloth is not recommended; you can simply wash the baby in warm water with herbs.
- Marigolds also have good antiseptic properties. For a bath, it is better to take 50 grams of marigold flowers and infuse them in water. Add to the bath and gently bathe the child.
- An infusion of sage and oak bark should be prepared in the following way: 30 grams of oak bark and 50 grams of sage leaves should be infused, added to water before bathing and after the bath, you can lubricate the baby's skin with this solution with the addition of two drops of olive oil without much effort in the navel area.
Homeopathic treatment of this pathology is not used, since the condition is acute and goes away with proper care, if there is no disease.
Prevention
Prevention of any problems with the navel in newborns, including bloody discharge, consists of proper care of the child. It is very important when the navel is healing normally not to treat it with anything, not to injure it, to keep it dry and clean.
The most physiological means of preventing any hemorrhagic manifestations is to put the baby to the breast early after birth. A specific method of preventing hemorrhagic manifestations is the use of vitamin K. The dosage for full-term babies is 0.5 ml, and for a larger amount of vitamin is needed, since the depot of this vitamin has not yet had time to be deposited - the dose is 1 mg. It is believed that for children on artificial feeding it is necessary to use 1 mg of vitamin K, since artificial mixtures do not contain a sufficient amount of this vitamin. This prevents late manifestations of hemorrhagic disease.
 [ 13 ]
[ 13 ]
Forecast
The prognosis may be favorable with timely diagnosis and differentiation of umbilical disease or hemorrhagic disease. Otherwise, there may be complications with the risk of developing sepsis and DIC syndrome, which has a fairly high percentage of fatal cases.
A newborn's navel may bleed due to simple trauma, in which case simple hygienic measures can help in treatment. But if this symptom is accompanied by a hemorrhagic skin rash, increased body temperature, or a general deterioration in the child's condition, then it is imperative to consult a doctor.

