Medical expert of the article
New publications
Ultrasound for miscarriage
Last reviewed: 04.07.2025

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
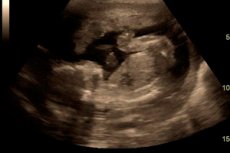
Currently, the most significant non-invasive research method in obstetrics and gynecology is ultrasound.
For visualization of congenital malformations of the uterus, the second phase of the menstrual cycle is more informative, when the endometrium in the secretory phase clearly outlines the contours of the uterine cavity.
A bicornuate uterus is represented by two formations connected to each other at a greater or lesser angle of a homogeneous structure during transverse scanning. The intrauterine septum is not always clearly visualized during ultrasound, and the uterus appears as a single formation with 2 M-ECHO. The M-ECHO defect depends on the degree of severity of the septum, if the defect was along the entire length, then the septum was complete, with a partial defect - incomplete. A saddle-shaped uterus is not always detected during ultrasound outside pregnancy, most often it looks like a single formation with a small indented contour in the area of the fundus of the uterine body.
Reliable differences were obtained for the following parameters: the thickness of the myometrium in congenital malformations and uterine hypoplasia is reduced by 25-40% compared to normal values.
In case of uterine hypoplasia, the length of the uterine body has significantly decreased by 15-26.6% and the cervix by 31-34%. A decrease in these indicators cannot but affect the functional capabilities of the uterus and determines a high degree of risk of complications during pregnancy.
The informativeness of echography, according to our data, was from 50 to 100%: the lowest for intrauterine adhesions, the highest for uterine myoma. With echography, organic isthmic-cervical insufficiency can be detected if the width of the cervical canal exceeds 0.5 cm, which is reliably higher than the standard parameters.
According to research data, a cervical width of over 1.9 cm indicates the presence of isthmic-cervical insufficiency.
Using the echography method, chronic endometritis is detected, especially when using a transvaginal sensor - an expansion of the uterine cavity to 0.3-0.7 cm and a small amount of fluid are noted.
The use of transvaginal ultrasound allows us to assess the condition of the endometrium, its readiness for implantation, and the dynamics of changes in the structure and thickness of the endometrium throughout the menstrual cycle.
Of extreme interest for practical use is the assessment of the biophysical profile of the uterus based on echography and Doppler data, developed at the Women's Healts Center Chicago.
Further examination is carried out taking into account the parameters that were identified at stage I and relate mainly to the clarification of pathogenetic mechanisms, selection of therapy and assessment of the effectiveness of the therapy and is carried out individually for patients. For example, if the main genesis of miscarriage is infectious, then the second stage includes an assessment of the immune status, interferon status, and the level of proinflammatory cytokines.
When changes are detected in the hemostasiogram, the cause of the thrombophilic condition is clarified: lupus anticoagulant, congenital hemostasis disorders, etc. These studies will be reflected when considering the tactics of managing patients with various causal factors of miscarriage.

