Medical expert of the article
New publications
Herpetic keratouveuitis and glaucoma
Last reviewed: 18.10.2021

All iLive content is medically reviewed or fact checked to ensure as much factual accuracy as possible.
We have strict sourcing guidelines and only link to reputable media sites, academic research institutions and, whenever possible, medically peer reviewed studies. Note that the numbers in parentheses ([1], [2], etc.) are clickable links to these studies.
If you feel that any of our content is inaccurate, out-of-date, or otherwise questionable, please select it and press Ctrl + Enter.
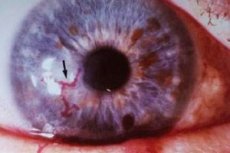
Infection of the eye caused by the herpes simplex virus (HSV) is manifested as recurrent unilateral blepharoconjunctivitis, epithelial and stromal keratitis and uveitis. Damage to the eye can also be observed during primary infection with herpes zoster (chicken pox), but more often it occurs with herpes zoster ophthalmicus - reactivation of the herpes zoster virus with damage to the eye branch of the V pair of cranial nerves in adults.
Uveitis caused by HSV and herpes zoster virus makes up about 5% of all adult uveitis, usually developing on the background of herpetic keratitis. A characteristic feature of recurrent herpetic uveitis is an increase in intraocular pressure, which can lead to the development of secondary glaucoma.
Epidemiology
Approximately 0.15% of US residents have a history of ocular manifestations of HSV infection. In 2/3 of the cases of herpes zoster ophthalmicus infection, eye damage is observed. Stromal keratitis and uveitis are conditions that lead to the greatest impairment of visual function, compared with other forms of recurrent herpetic lesion of the eye. Stromal keratitis and uveitis develop in less than 10% of patients with primary infection of the eye with the herpes simplex virus. Uveitis and ocular hypertension in patients with herpes zoster ophthalmicus may be combined with epithelial or stromal keratitis. The frequency of increase in intraocular pressure in patients with herpetic uveitis is 28-40%. The incidence of secondary glaucoma in patients with uveitis caused by herpes simplex or herpes zoster is 10-16%.
Causes of herpetic keratouveitis
Whether the development of uveitis associated with herpes simplex keratitis, secondary to corneal lesions or associated with viral invasion in the anterior choroid at the moment is unknown. The increase in intraocular pressure during herpes simplex and herpes zoster uveitis occurs as a result of a violation of the outflow of intraocular fluid due to trabeculitis - inflammation of the trabecular network. When uveite caused by herpes zoster, ischemia develops associated with occlusive vasculitis, which can also lead to an increase in intraocular pressure. In case of herpetic, the herpes simplex was isolated from the moisture of the anterior chamber, the presence of which probably correlates with the development of ocular hypertension. Increased intraocular pressure in herpetic pain may also be associated with prolonged intake of glucocorticoids.
Symptoms of herpetic keratouveuitis
Patients suffering from herpetic uveitis usually complain of redness of one eye, pain, photophobia and decreased visual acuity. Often there is a history of recurrent keratitis. Patients suffering from herpes zoster uveitis, as a rule, older patients with a history of herpes zoster ophthalmicus. In rare cases, bilateral damage to the eye of HSV is observed, and damage to the eye of herpes zoster is only one-sided.
Course of the disease
Like other manifestations of herpetic lesions of the eyes, herpetic uveitis is recurrent and can occur on the background of recurrent keratitis. With exacerbation of intraocular inflammation, an increase in intraocular pressure is usually observed, which, as uveitis resolves, may normalize or remain elevated. In approximately 12% of cases, a persistent increase in intraocular pressure develops, requiring the use of antiglaucoma therapy or an operation aimed at improving filtration.
 [21]
[21]
Ophthalmologic examination
An external examination reveals signs of iridocyclitis) skin lesions herpes zoster, conjunctival and ciliary injection. The sensitivity of the cornea on the affected eye is often reduced. When examining the cornea in patients suffering from herpetic keratouveitis, they reveal changes that indicate a previous lesion of the epithelium or corneal stroma (tree epithelial foci, tree opacities, active disciform or necrotic stromal keratitis, neovascularization or scarring). With two forms of herpetic uveitis, diffuse non-granulomatous stellate or pigmented granulomatous precipitates on the cornea can be detected. In severe herpetic uveitis, the posterior synechia and the anterior chamber angle can be detected. With uveite, caused by both the herpes simplex virus and herpes zoster, characteristic atrophy of the iris develops. With the defeat of HSV atrophy occurs in the central part of the iris closer to the pupil, often has a spotted appearance, and with the defeat of herpes zoster atrophy of the iris has a segmental character and is localized closer to the periphery. It is believed that when herpes zoster is damaged, the cause of atrophy of the iris is occlusive vasculitis in the stroma.
 [22]
[22]
Laboratory research
The diagnosis of herpetic uveitis is made on the basis of clinical data, usually does not require laboratory research methods. In the absence of antibodies to HSV and varicella zoster, the diagnosis of herpetic uveitis is excluded. Detection of viral DNA in the intraocular fluid by the method of polymerase chain reaction confirms the diagnosis of herpetic uveitis, but does not allow to put it.
Treatment of herpetic keratouveitis
For uveitis associated with HSV or herpes zoster, local glucocorticoids are prescribed. In case of pain associated with ciliary spasm, cycloplegic drugs may be required. To reduce the risk of recurrence of epithelial keratitis, in addition to local glucocorticoids, antiviral medication should be prescribed. It has been shown that when taking acyclovir orally, the incidence and severity of tree keratitis, stromal keratitis and uveitis in patients with herpes zoster ophthalmicus are reduced. With an increase in intraocular pressure should be antiglaucoma therapy. Sometimes it may be necessary to perform an operation aimed at improving filtration. It is believed that in case of herpetic, argon laser trabeculoplasty is not effective.

